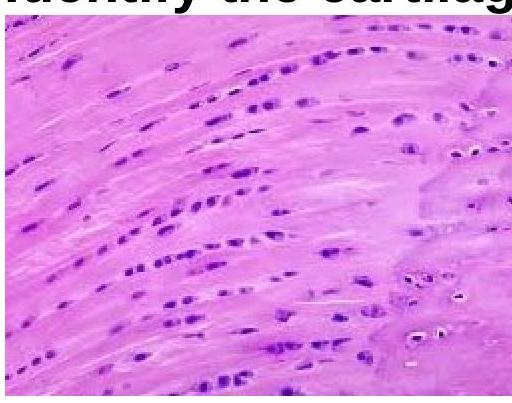
Identify the type of cartilage shown in the image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the type of cartilage shown in the image.

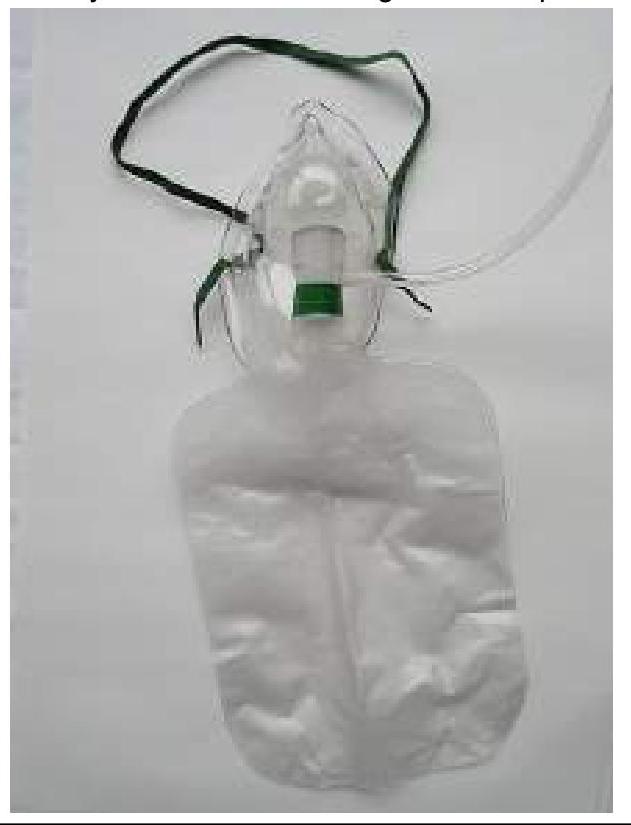
Identify the mask used for patients requiring high concentrations of oxygen.
Which of the following helps in the transport of fatty acids across the inner mitochondrial membrane?
An adolescent male patient presents to you with exercise intolerance. He gives a history of developing cramps on exertion. Which of the following enzyme deficiencies could be the cause?
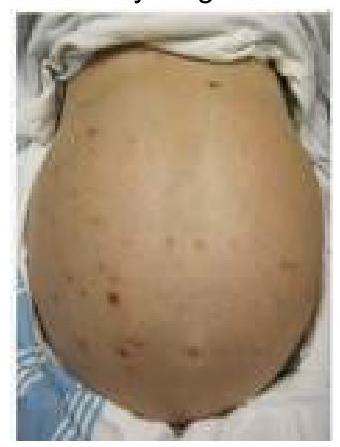
A patient with a history of chronic liver disease presents with abdominal distension, jaundice, and pruritis. Ascitic fluid analysis revealed a neutrophil count >650 per cubic mm. What is the most likely diagnosis?
Which of the following is not seen in MEN 2B syndrome?
A patient presents to you with fever, night sweats, ptosis, and bilateral facial nerve palsy. Investigations showed leukocytosis and bilateral hilar lymphadenopathy. Which of the following is the most likely diagnosis?
An 11-year-old child with a history of streptococcal pharyngitis presents you with fever and arthralgia. There is no past history of rheumatic heart disease or features of carditis or valvular disease. How often is 600,000 IU of benzathine penicillin recommended for prophylaxis of rheumatic heart disease?
A patient presents to the emergency department with a history of ingestion of ten tablets of paracetamol. He has developed oliguria and liver function tests show deranged values. In the context of paracetamol overdose, which of the following can be used in the management of this condition?
A female patient presents to you with a unilateral headache. It is associated with nausea, photophobia, and phonophobia. What is the drug of choice for acute management?