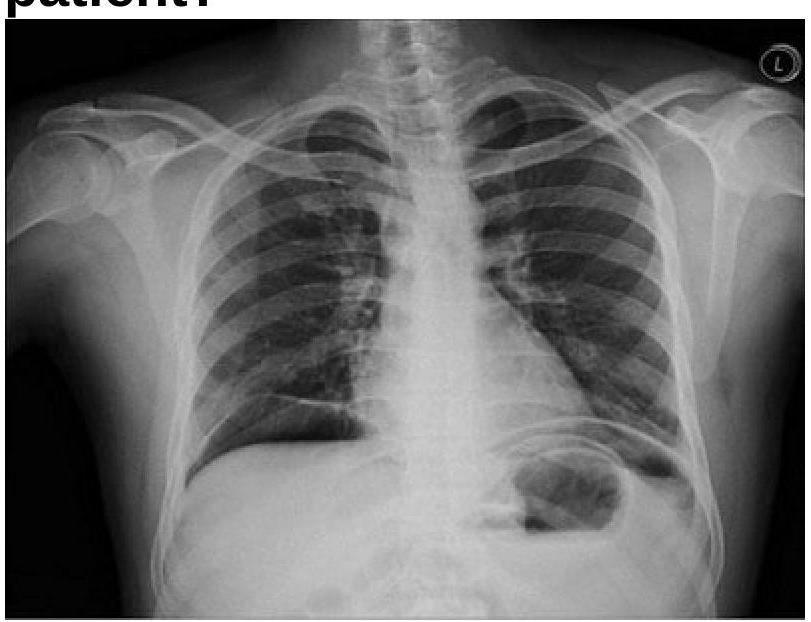
A 40 years old male was brought emergency with severe abdominal pain. On examination, pulse rate was 112/minute and systolic BP was 80 mmHg. Chest x-ray is given below. What is the most appropriate management?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
STEPwise approach to surveillance for Non-Communicable diseases step 2 is
A 22-year-old woman presents with diffuse hair loss for 1 month. She had a past history of enteric fever 4 months ago. What is the likely cause?
Pitting of nails is seen in:
A couple comes for evaluation of infertility. The HSG was normal but semen analysis revealed azoospermia. What is the diagnostic test to differentiate between testicular failure and vas deferens obstruction?
Hymenal tear following first sexual intercourse most commonly occurs at which position:
A blood specimen for neonatal thyroid screening is obtained on:
The mechanism of action of botulinum toxin A is best described by:
Most sensitive investigation for abdominal trauma in a hemodynamically stable patient is-
What is the role of fixer?
A 40 years old male was brought emergency with severe abdominal pain. On examination, pulse rate was 112/minute and systolic BP was 80 mmHg. Chest x-ray is given below. What is the most appropriate management?
