A 20 year old woman presented at 7 weeks of gestation, unwilling to continue the pregnancy. What are the drugs used for medical termination of pregnancy in this patient?
An intrauterine scan at the 13th week of pregnancy showed a fetus with multiple long bone fractures. What is commonly associated with this finding?
What will be the level of the uterus on the second day post delivery?
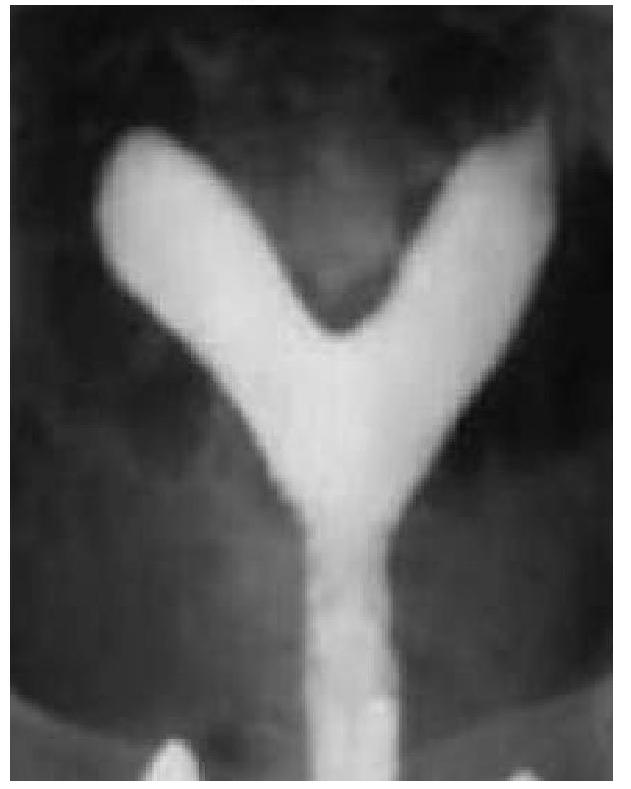
A 20 year old woman is evaluated for primary infertility. Hysterosalpingography was done and reveals an anomaly. What is the anomaly seen in the image?
Which of the following is NOT an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
A primigravida at 22 weeks of gestation presents with profuse vaginal bleeding. Her blood pressure and glucose levels are normal. At which of the following sites can placental implantation lead to this condition?
A female patient collapses soon after delivery. There is profuse bleeding and features of disseminated intravascular coagulation. Which of the following is the most likely etiology?
A female patient presents to you with six weeks of amenorrhea, associated with abdominal pain and vaginal bleeding with normal blood pressure. Investigations revealed beta-hCG to be 1400 mIU/mL. An ultrasound scan was done which showed a trilaminar endometrium with normal adnexa. What is the next best step in the management of this patient?
A couple comes for evaluation of infertility. The HSG was normal but semen analysis revealed azoospermia. What is the diagnostic test to differentiate between testicular failure and vas deferens obstruction?
Hymenal tear following first sexual intercourse most commonly occurs at which position: