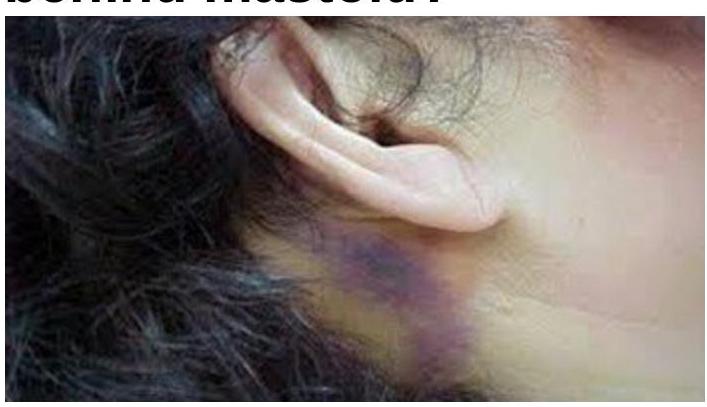
What does a bluish-purple discoloration behind the mastoid indicate?
Not a landmark of facial nerve identification in parotid surgery:
A patient presents with abdominal pain, blood in stools and a palpable mass on examination. A Barium Study was performed, probable diagnosis is?
Which one of the following is not a component of THORACOSCORE?
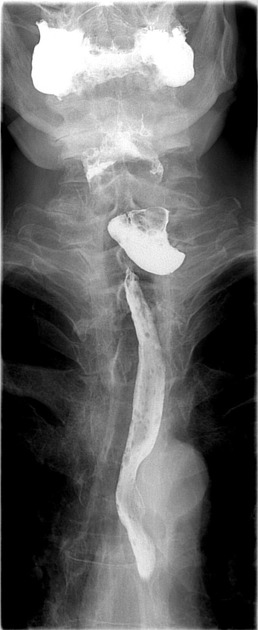
A 70 year old patient presented with history of fever, repeated aspiration and coughing in the night. On examination there is a swelling on left side of neck which produces gurgling sound on compression. Following is the barium swallow study of the patient. What is the most likely diagnosis?
A patient is on follow-up for recurrent abdominal pain. USG reveals an aortic aneurysm of 40 mm. What should be the next immediate step?
A middle aged man complains of upper abdominal pain after a heavy meal. There is tenderness in the upper abdomen and on X-ray, widening of the mediastinum is seen with air in the mediastinum. What is the diagnosis?
A 20 year old boy is brought to the emergency following a RTA (Road Traffic Accident) with respiratory distress and hypotension. He has subcutaneous emphysema and no air entry on the right side. What is the next best step in the management?
A man is brought to the emergency after he fell into a man hole and injured his perineum. He feels the urge to micturate but is unable to pass urine and there is blood at the tip of the meatus with extensive swelling of the penis and scrotum. What is the location of the injury?
Which of the following statements is true regarding retrosternal goiters?