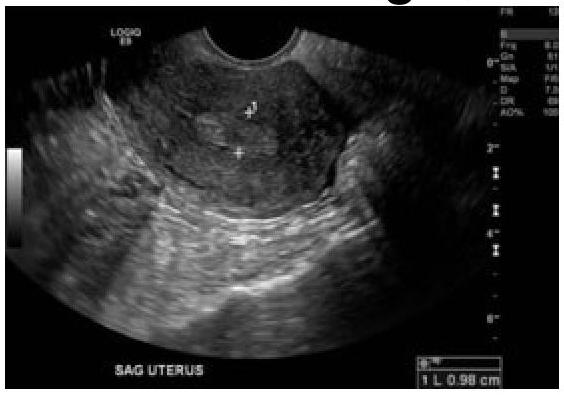
60-year-old female with a history of intermittent bleeding. What is the diagnosis based on the ultrasound image?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
The patient is presenting with pain around the base of the thumb. Which tendons are likely involved?
In which of the following methods of management is the benefit measured in natural units?
Elderly man with a long-standing mole on his face that is increasing in size and showing an irregular border. Diagnosis:
MC location of gastrinoma in MEN-1 syndrome?
Which antibody is not transmitted from mother to baby?
60-year-old female with a history of intermittent bleeding. What is the diagnosis based on the ultrasound image?

A person was given a muscle relaxant that competitively blocks nicotinic receptors. Which of the following drugs is used for reversal of muscle relaxation after surgery?
A 35-year-old female experiences a tingling sensation in her arm after watching TV for long hours with her hands under her head. Which type of nerve fibers is most likely to be affected due to this position?
A patient with depression was given Imipramine for 2 weeks. Relatives noticed increased excitement, colorful clothes, and increased talking. What is the next step in management?
A 68-year-old asymptomatic male is found to have an abdominal aortic aneurysm (AAA) measuring 4.5 cm on routine ultrasound screening. What is the most appropriate management?