Tumour of the uncinate process of the pancreas will compress which artery
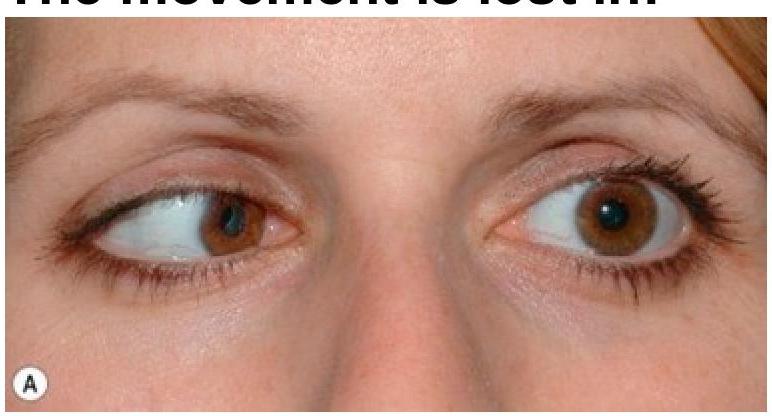
In trochlear palsy, which specific eye movement is lost?
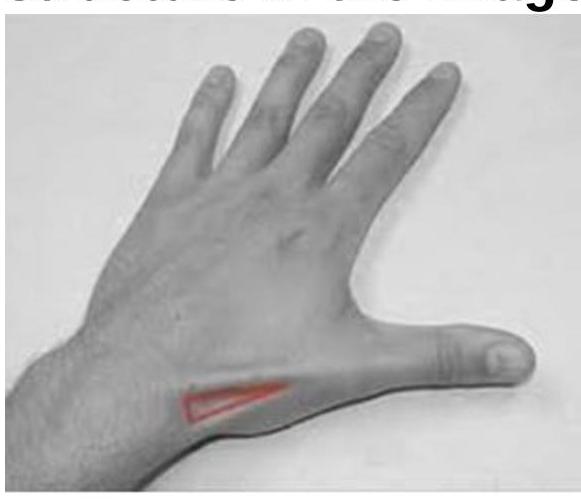
The image shows a highlighted region on the dorsal aspect of the hand (anatomical snuffbox). Which of the following anatomical structures form the boundaries or floor of this region?