Episiotomy incision was extended posteriorly beyond perineal body injuring the structure immediately posterior to it. Which structure has been injured?
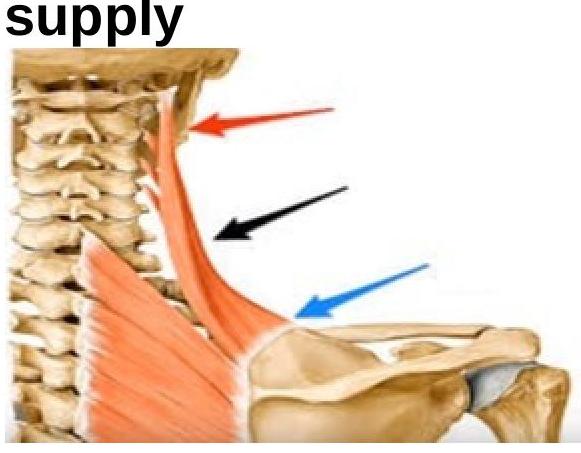
What is the nerve supply of the shown muscle?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Episiotomy incision was extended posteriorly beyond perineal body injuring the structure immediately posterior to it. Which structure has been injured?
What is the nerve supply of the shown muscle?

In a preterm baby with respiratory distress syndrome, which of the following lipids would be deficient?
Patient with clinical signs of DVT had tachycardia and history of bladder cancer. According to modified Well's scoring, the probability of pulmonary embolism would be :
Which of the following is most likely to be acquired by traumatic inoculation?
A 60 years old Female with intermittent bleeding per vagina, endometrial collection, and thickening with anterior bulging of the fundal area on ultrasound. What is the most probable diagnosis?
A 5-year-old child is having acute liver failure. Which one of the following criteria is not included in the King's College criteria?
Anti-glaucoma drug that acts by increasing uveoscleral outflow is
A patient was on lithium therapy for bipolar disorder for 6 months. She fasted for few days due to religious reasons and presented with coarse tremors, abdominal pain, nausea, dizziness & confusion. Which of the following should be done to assess her condition?
A man is brought to the emergency after he fell into a man hole and injured his perineum. He feels the urge to micturate but is unable to pass urine and there is blood at the tip of the meatus with extensive swelling of the penis and scrotum. What is the location of the injury?