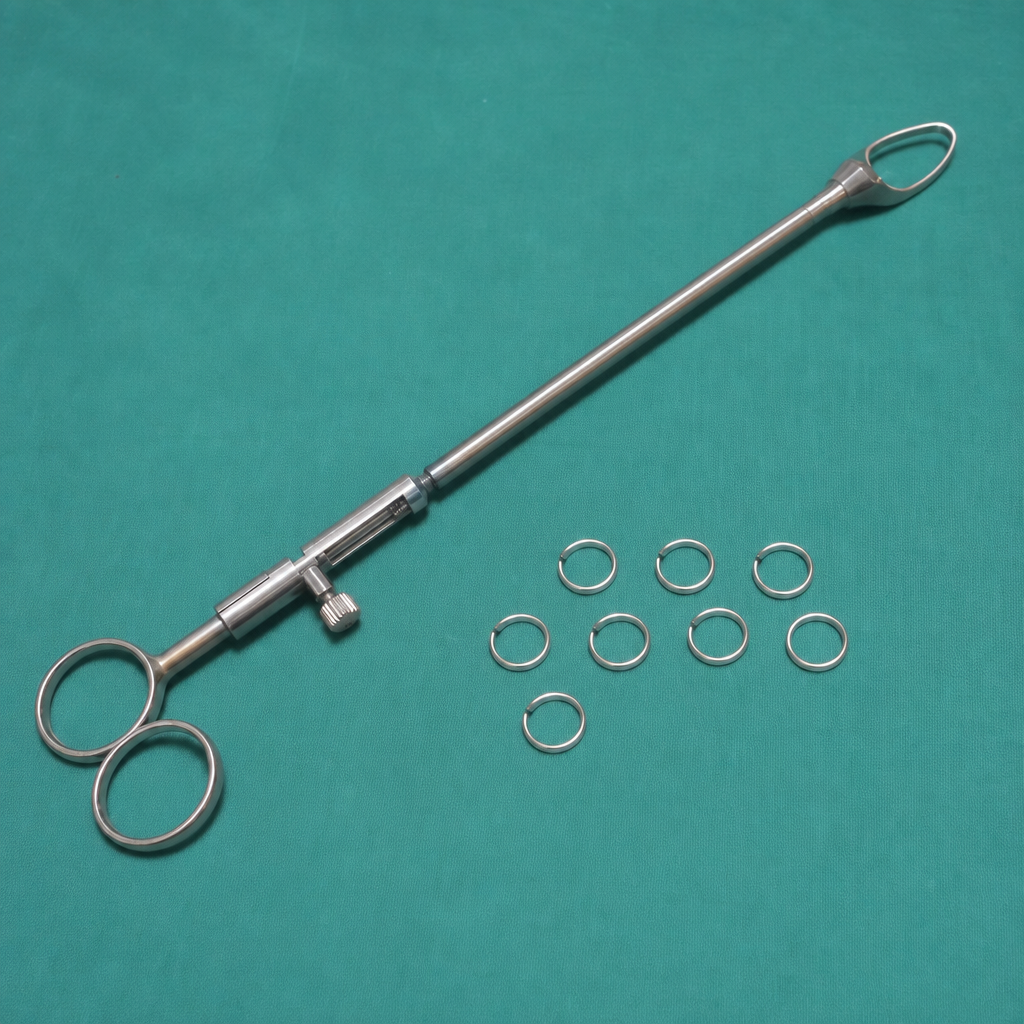
The depicted instrument (Fallopian ring applicator) is used in which procedure?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Female, on maize as a staple diet. History of diarrhoea and lesion in the neck region. This is due to deficiency of which of the following?
Liquid chemical waste is discarded in:
Tuberculous otitis media of the middle ear has all of the following except:-
A 26 year old female after her delivery develops features of headache, nausea, visual complaints, fatigue. What is the most probable diagnosis?
Superantigen is produced by which of the following?
The depicted instrument (Fallopian ring applicator) is used in which procedure?

A 5-year-old unvaccinated child presents to the OPD with fever, red eyes, and a maculopapular rash. What is the most likely complication associated with this condition?
Which of the following drugs act by inhibiting DNA replication?
Radiation Dose Monitoring in Occupational Workers is done by
Which of the following is a FALSE statement regarding radiation?