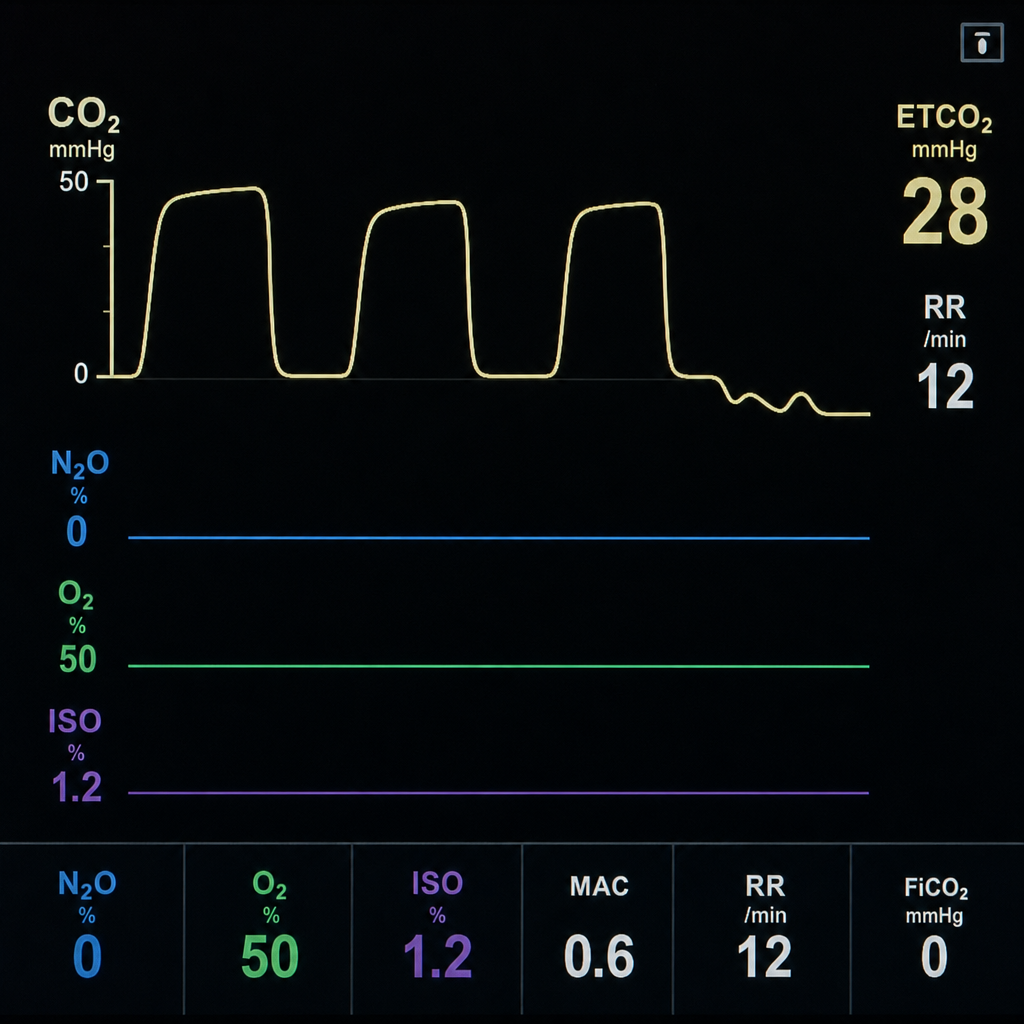
During intraoperative period following capnograph waveform is seen. What does it signify.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
During intraoperative period following capnograph waveform is seen. What does it signify.

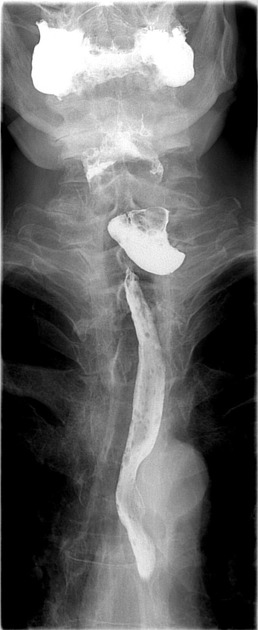
A 70 year old patient presented with history of fever, repeated aspiration and coughing in the night. On examination there is a swelling on left side of neck which produces gurgling sound on compression. Following is the barium swallow study of the patient. What is the most likely diagnosis?
Which of the following is not done in high altitude sickness?
Pulmonary Plethora is seen in -
Which of the following is a Category A bioterrorism agent?
Large, irregular and friable vegetations are seen in?
Which of the following is a cause of Hirschsprung disease in a patient?
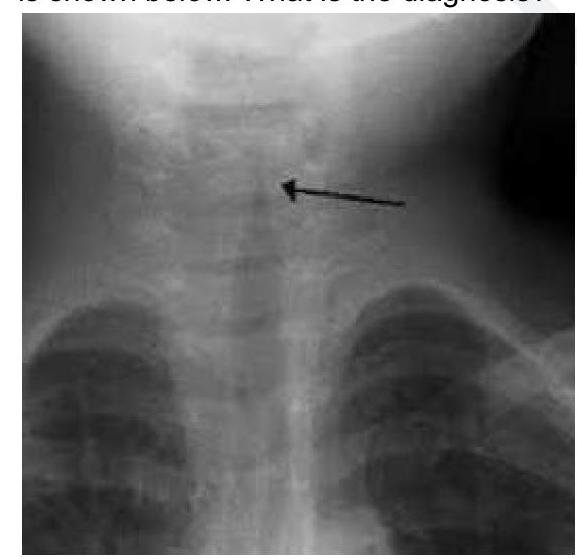
A 2 year child presented with low grade fever and stridor. What is the likely diagnosis?
Which of the following, if normal, would be most significant in making PEM unlikely?
Which one of the following is not a component of THORACOSCORE?