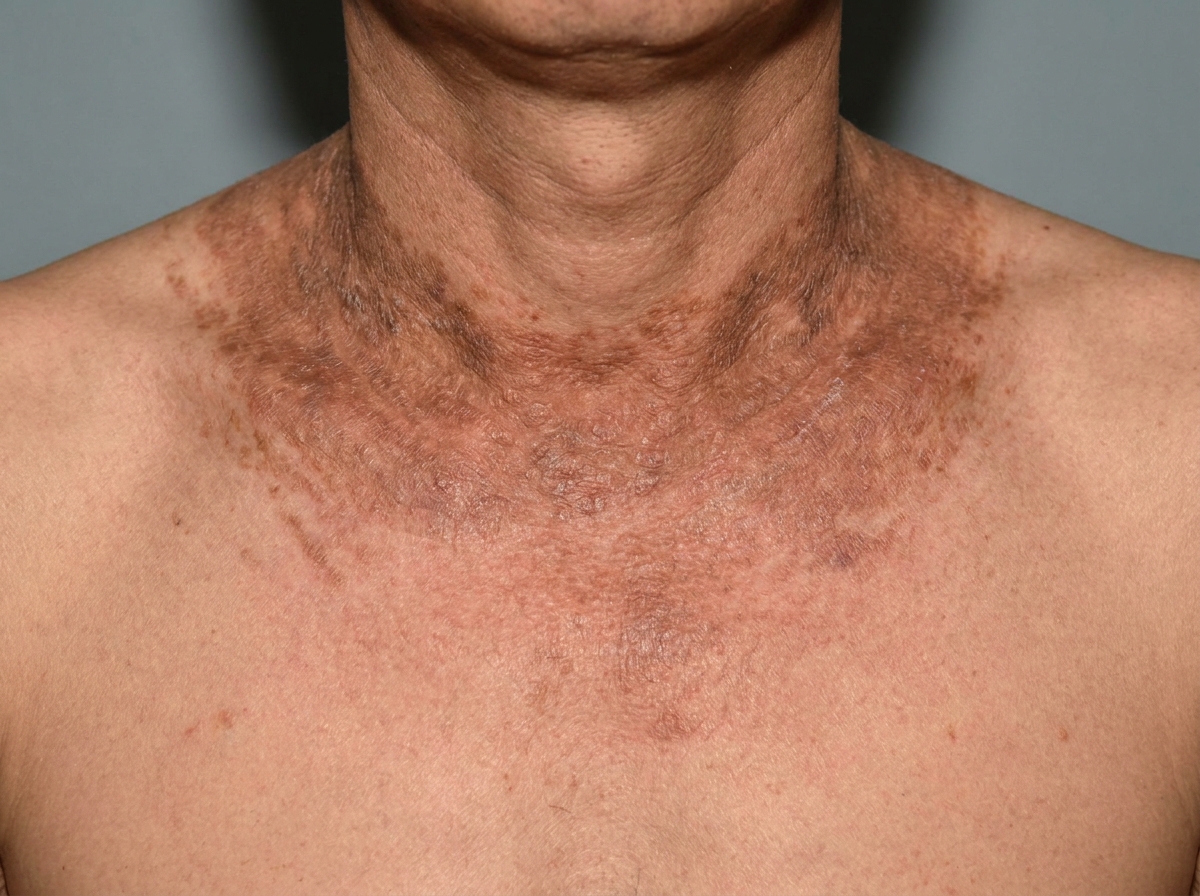
Dermatological manifestation of which of the following diseases?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Dermatological manifestation of which of the following diseases?

Which of the following is true about polyaeritis nodosa?
A patient undergoes bilateral adrenalectomy in view of bilateral pheochromocytoma. A day after surgery patient develops lethargy, fatigue and loss of appetite. On examination BP is 90/ 60 mmHg, pulse rate of 74 beats/min. No evidence of loss of volume. The likely cause is?
Urethritis in males is not caused by:
35 yr old lady attends gynaec OPD with excessive bleeding since 6 months, not controlled with non hormonal drugs. USG and clinical examination reveals no abnormality. Next step is?
What is the diagnosis for a patient with unilateral proptosis with bilateral 6th nerve palsy with chemosis and euthyroid status?
A 2 years old child presents to PHC with fever and cough. He has chest in-drawing and respiratory rate of 38 per minute, weight 11 kg. The next step in management according to IMNCI is:
A term neonate, with a birth weight of 2700 g, who is otherwise well, and is exclusively breastfed, presents for routine evaluation. His total serum bilirubin is found to be 14mg/dl on day 5. What is the management?
A patient of biliary colic presented to hospital. Intern gave an injection and the pain worsened. Which is the most likely injection given?
Which one of the following is not a component of THORACOSCORE?