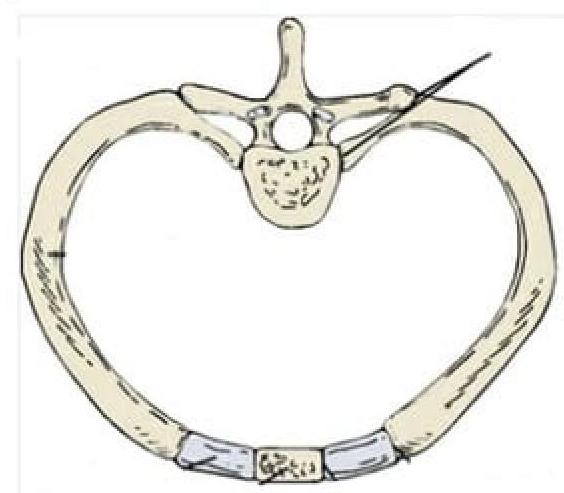
Identify the type of joint in the image provided.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the type of joint in the image provided.

A 13-year-old child visits the OPD with complaints of not attaining menarche, and has a karyotype of 46,XX. On examination, there is clitoromegaly. Which enzyme is likely deficient?
Most common cause of death in SLE in children
60-year-old female with a history of intermittent bleeding. What is the diagnosis based on the ultrasound image?
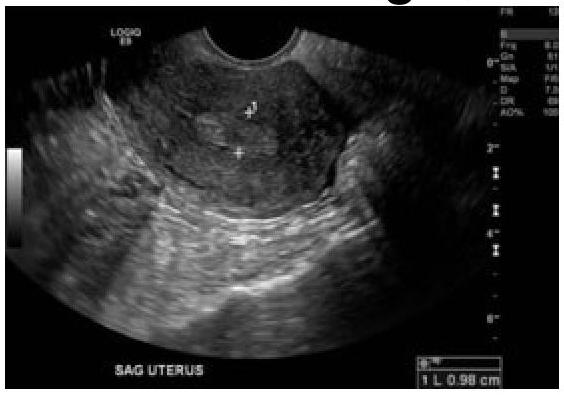
What is the best treatment option for a septate uterus?
HBsAg is based on which principle
What is the most serious complication of measles?
Which of the following is not considered a prokinetic agent?
What is the Drug of Choice (DOC) for Onychomycosis?
Which of the following is referred to as the "Window of the limbic system"?