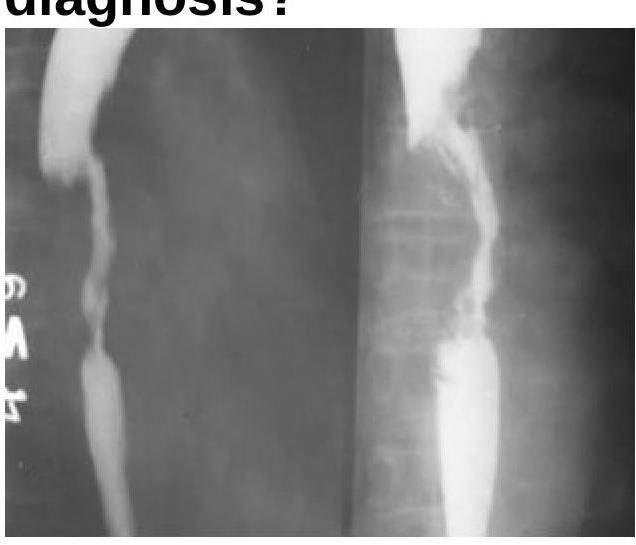
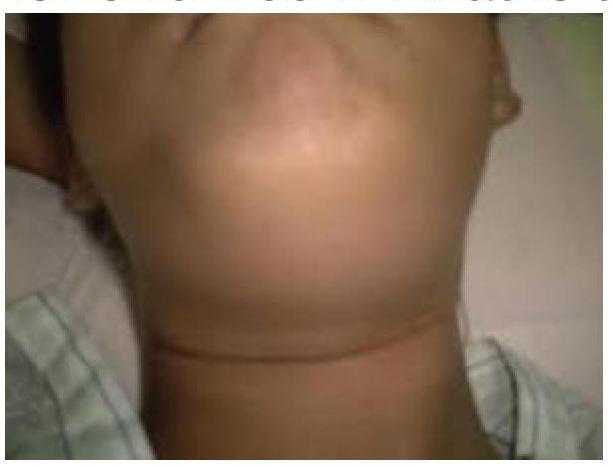
A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?

Relatives of a patient told during postmortem examination that the person had a tattoo - which was now invisible. How to identify?
A body is discovered with burn marks as shown in the image, resembling a 'crocodile skin' pattern. What is the most likely cause?

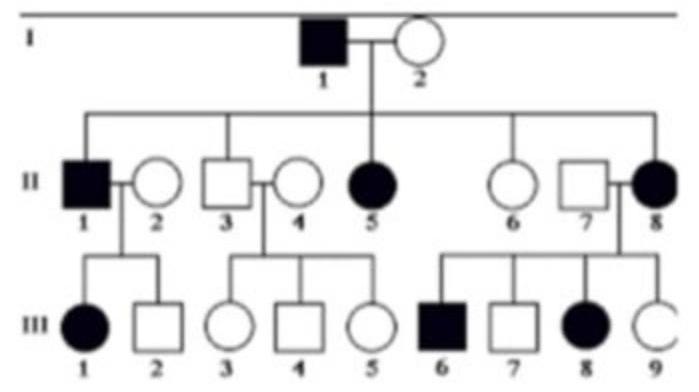
25-year-old man presents for a routine physical examination. The patient is tall and on examination, he was found to have an early diastolic murmur. His family pedigree is given below (image attached). Which of the following is the mode of inheritance by which the disease is likely to be transmitted?
A mother brought her 16-year-old daughter to Gynaecology OPD with a complaint of not attaining menarche. She gives a history of cyclic abdominal pain. On further examination, a midline abdominal swelling is seen. Per rectal examination reveals a bulging mass in the vagina. Which of the following conditions is most likely responsible for these findings?
Which of the following is not considered an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
All-trans retinoic acid is primarily used in the treatment of which of the following tumors?
Which of the following antimicrobials should not be given to a chronic asthmatic patient managed on theophylline therapy?
Identify the radiological sign of Ischemic colitis from the image provided.
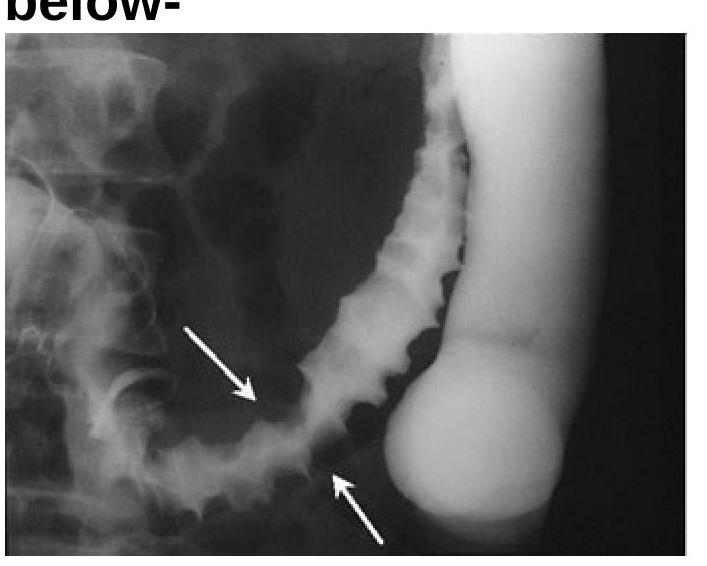
The Barium Swallow examination shows a filling defect in the esophagus. What is the most probable diagnosis?