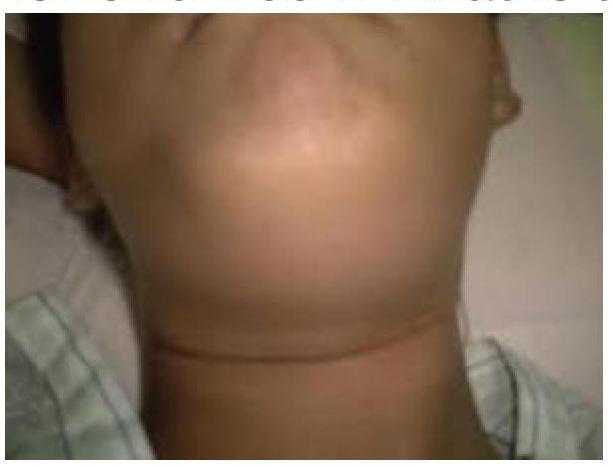
A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which pigment is responsible for the greenish-black color of neonatal stool?
Which of the following is a technique/method based on behavioral sciences
Admission rate bias is?
What is the target population for a Secondary Service Center as per the Vision 2020 initiative in India?
A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?

In the context of civil negligence against a doctor, who bears the burden of proof?
In the context of retinal conditions, what is the primary cause of shifting fluid beneath the retina?
What is the first-line drug for osteoporosis in postmenopausal women?
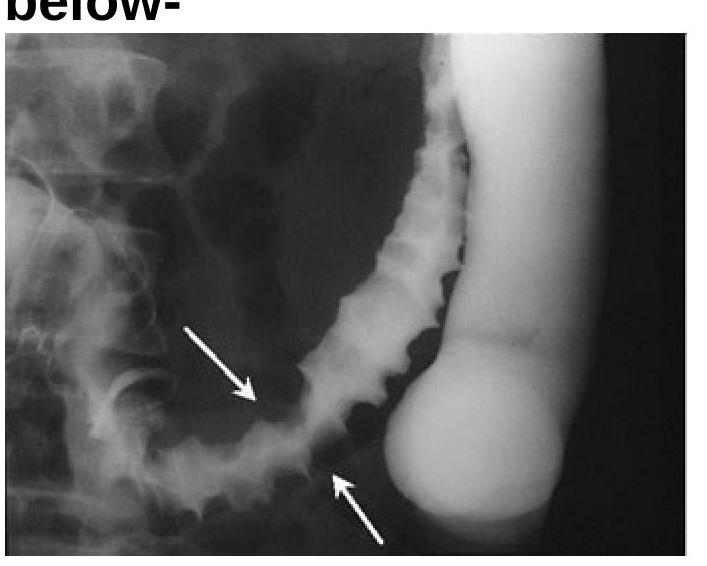
Identify the radiological sign of Ischemic colitis from the image provided.
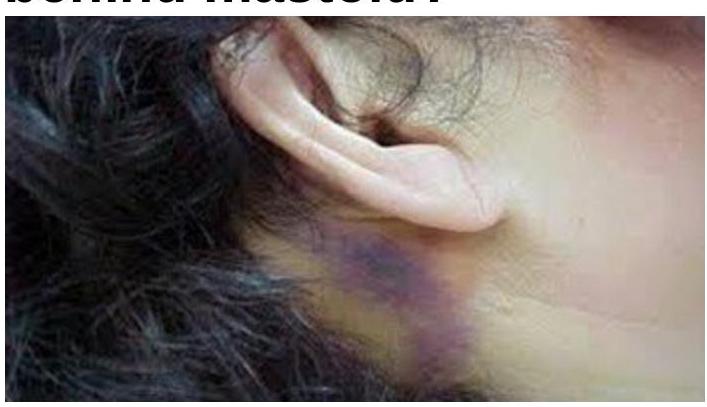
What does a bluish-purple discoloration behind the mastoid indicate?