A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Ochronosis is due to the accumulation of?
What is the appropriate color for containers used to dispose of chemical liquid biomedical waste?
A 30-year-old male presents with a one-week history of severe toothache, swelling in the floor of the mouth, and difficulty swallowing. What is the most likely diagnosis?

What is the cause of loss of pain and temperature sensation on the ipsilateral face and contralateral body due to thrombosis?
Renal tubular acidosis with ABG value pH = 7.24 PO2=80; PaCO2= 36 Na = 131; HCO3 = 14 Cl= 90; BE = -13 Glucose = 135 the above ABG picture suggests –
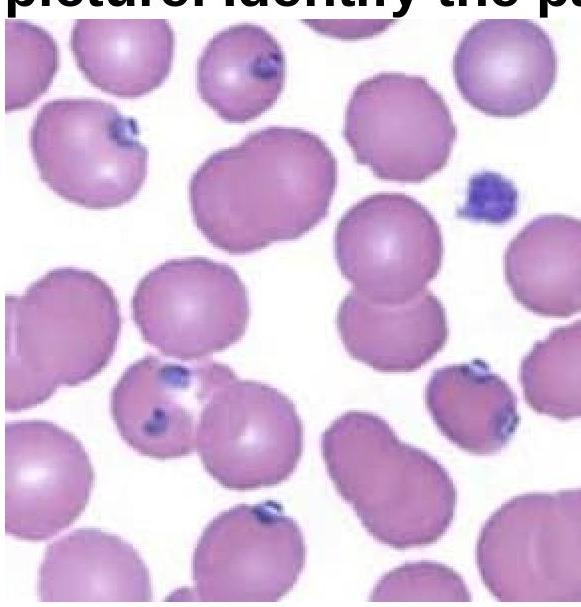
A 15-year-old boy presented with fever and chills for 3 days. On examination, he was found to have delayed skin pinch time and dry oral mucosa. Identify the pathogen involved based on the provided peripheral blood smear image.
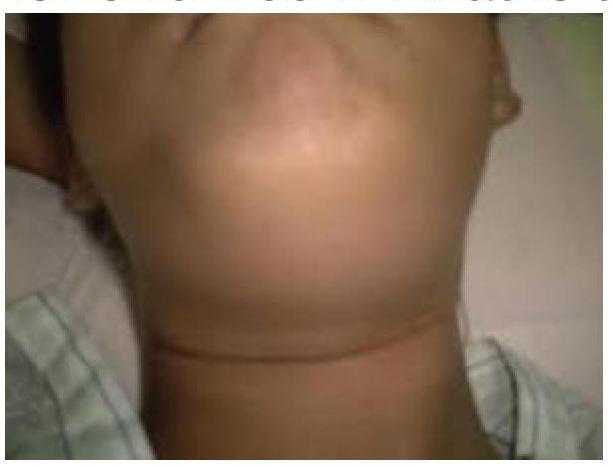
A mother brought her 16-year-old daughter to Gynaecology OPD with a complaint of not attaining menarche. She gives a history of cyclic abdominal pain. On further examination, a midline abdominal swelling is seen. Per rectal examination reveals a bulging mass in the vagina. Which of the following conditions is most likely responsible for these findings?
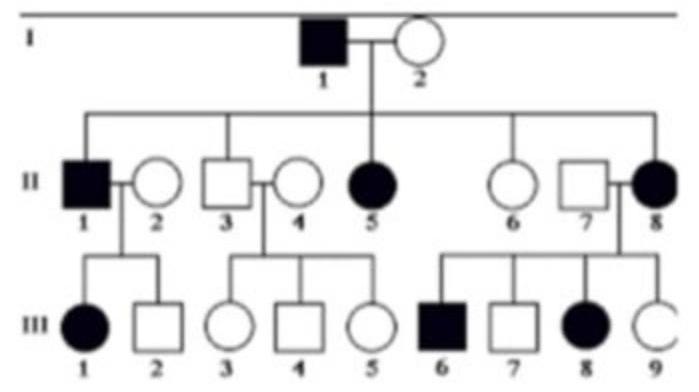
25-year-old man presents for a routine physical examination. The patient is tall and on examination, he was found to have an early diastolic murmur. His family pedigree is given below (image attached). Which of the following is the mode of inheritance by which the disease is likely to be transmitted?
Where does meiosis occur in human females?
Cerebral blood flow is regulated by all of the following except: