NEET-PG 2020 — Obstetrics and Gynecology
29 Previous Year Questions with Answers & Explanations
What is the obstetric score of a 26-year-old woman who is 36 weeks pregnant, has had one previous delivery of twins, and is certain of her dates?
What is the best treatment option for a septate uterus?
A 22-year-old primigravida visits ANC OPD with 20 weeks POG. On examination uterine height reveals a 16-week size. USG shows reduced liquor. What will be the diagnosis?
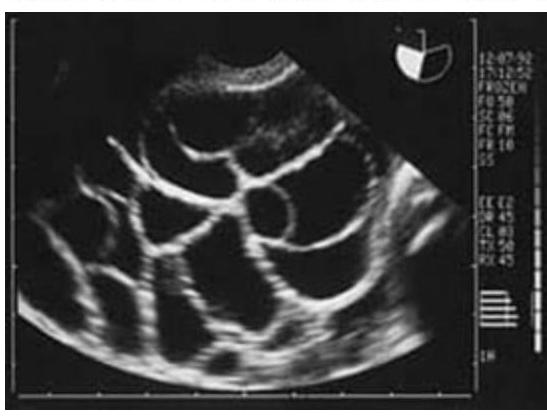
A lady on treatment for infertility developed ascites, abdominal pain, and dyspnea. The ultrasound image is shown below. What is the most likely diagnosis?
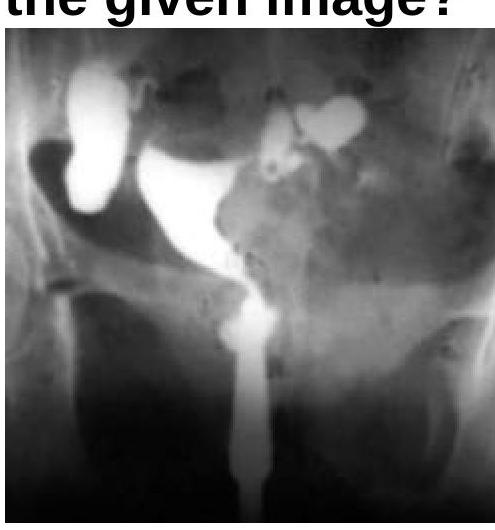
What will be the Hysterosalpingogram (HSG) finding?
A 36-week pregnant lady with previous twin delivery. What is the Obstetric score?
Which distension medium is used for hysteroscopy with bipolar cautery?
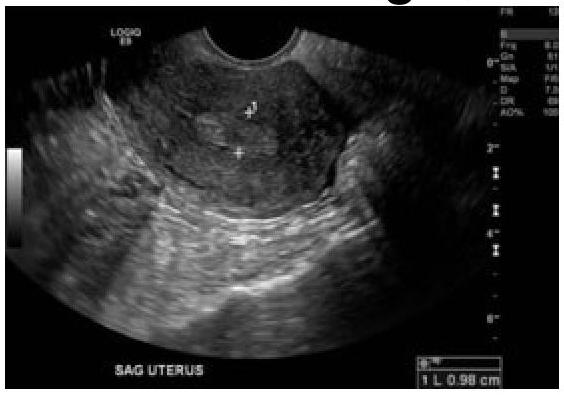
60-year-old female with a history of intermittent bleeding. What is the diagnosis based on the ultrasound image?
A sexually active female presenting with profuse frothy foul-smelling discharge with intense itching. Strawberry cervix revealed on examination. What will be the diagnosis?
What is the use of the instrument shown in the image?

NEET-PG 2020 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 1: What is the obstetric score of a 26-year-old woman who is 36 weeks pregnant, has had one previous delivery of twins, and is certain of her dates?
- A. G2P1L2 (2 live births) (Correct Answer)
- B. G3P2L2 (3 pregnancies, 2 live births)
- C. G2P2L2 (2 pregnancies, 2 live births)
- D. G3P3L2
Explanation: ***G2P1L2 (2 live births)*** - **Gravida (G)** refers to the total number of pregnancies, including the current one. This woman is currently pregnant and has had one previous pregnancy, making her G2. - **Parity (P)** refers to the number of pregnancies that reached viability (>20 weeks gestation or >500g), *regardless of the number of fetuses*. She had one previous delivery (twins) that reached viability, so her P is 1. The current pregnancy is not included in parity until after delivery. - **Live births (L)** refers to the number of live children delivered. Her previous pregnancy resulted in twins, meaning 2 live births. *G3P2L2 (3 pregnancies, 2 live births)* - This option incorrectly counts the number of pregnancies (**G**) as 3. She has had one previous pregnancy and is currently pregnant, totaling 2 pregnancies. - It also incorrectly counts the parity (**P**) as 2. Parity refers to the number of deliveries that reached viability, not the number of fetuses. Her previous delivery was a single event, making P1. *G2P2L2 (2 pregnancies, 2 live births)* - While the Gravida (G2) and Live births (L2) are correct, the Parity (**P**) is incorrectly stated as 2. Parity refers to the number of viable pregnancies delivered, and she has only had one previous delivery. - The number of fetuses (twins) does not increase the parity count for a single delivery event. *G3P3L2 (3 pregnancies, 3 live births)* - This option incorrectly states the number of pregnancies (**G**) as 3 and the parity (**P**) as 3. - The woman has only had one previous pregnancy and is currently pregnant, for a total of G2 and P1.
Question 2: What is the best treatment option for a septate uterus?
- A. Tompkins Metroplasty
- B. Jones metroplasty
- C. Strassmann metroplasty
- D. Transcervical hysteroscopic resection of the septum (Correct Answer)
Explanation: ***Transcervical hysteroscopic resection of the septum*** - This procedure involves using a **hysteroscope** to visualize and resect the **fibrous or muscular septum** that divides the uterine cavity, restoring a normal uterine shape. - It is considered the gold standard due to its **minimally invasive nature**, effectiveness in improving reproductive outcomes, and lower risk of complications compared to abdominal approaches. *Tompkins Metroplasty* - This is an **abdominal surgical procedure** primarily used for the repair of a **bicornuate uterus**, not typically for a septate uterus. - It involves resecting the uterine fundus to create a single uterine cavity, which is more invasive than hysteroscopic septum resection. *Jones metroplasty* - This procedure is also an **abdominal approach** used for the surgical correction of a **bicornuate uterus**, not a septate uterus. - It involves excising the septal portion and approximating the uterine walls. *Strassmann metroplasty* - This is another **abdominal surgical technique** that is primarily indicated for the repair of a **bicornuate or didelphys uterus**, where a large defect needs to be corrected. - It involves reconstructing the uterus through a fundal incision, which is significantly more invasive than hysteroscopic septal resection for a septate uterus.
Question 3: A 22-year-old primigravida visits ANC OPD with 20 weeks POG. On examination uterine height reveals a 16-week size. USG shows reduced liquor. What will be the diagnosis?
- A. Bilateral renal agenesis (Correct Answer)
- B. Bartter’s syndrome
- C. Liddle syndrome
- D. Fetal anemia
Explanation: ***Renal agenesis*** - **Bilateral renal agenesis** leads to **oligohydramnios** because the fetal kidneys are the primary producers of amniotic fluid after 16 weeks of gestation. - The reduced amniotic fluid (liquor) is consistent with the decreased uterine size (16-week size at 20 weeks POG) and is a hallmark of this condition, often resulting in **Potter sequence**. *Bartter’s syndrome* - This is a rare, inherited renal tubulopathy characterized by significant electrolyte disturbances (hypokalemia, metabolic alkalosis, hypercalciuria) due to impaired ion transport. - While it affects kidney function, it does not typically cause severe **oligohydramnios** or **renal agenesis** and would not explain the small uterine size in this scenario. *Liddle syndrome* - This is a rare genetic disorder characterized by early-onset hypertension, hypokalemia, and metabolic alkalosis, due to constitutive activation of the epithelial sodium channel (ENaC) in the collecting ducts. - It does not involve structural kidney abnormalities or significantly impact amniotic fluid volume during pregnancy to cause the described findings. *Fetal anemia* - Fetal anemia can lead to complications such as **hydrops fetalis**, which would typically cause **polyhydramnios** or a uterine size larger than expected due to fluid accumulation, not oligohydramnios or a smaller uterine size. - Reduced liquor and a small uterine size are not characteristic presentations of fetal anemia.
Question 4: A lady on treatment for infertility developed ascites, abdominal pain, and dyspnea. The ultrasound image is shown below. What is the most likely diagnosis?
- A. PCOS
- B. OHSS (Correct Answer)
- C. Theca lutein cyst
- D. Mucinous cystadenomas
Explanation: ***OHSS*** - The clinical presentation of a woman undergoing infertility treatment who develops **ascites**, **abdominal pain**, and **dyspnea** is classic for **Ovarian Hyperstimulation Syndrome (OHSS)**. The ultrasound image showing massively enlarged, multicystic ovaries with numerous follicles further confirms this diagnosis. - OHSS is an iatrogenic complication of **ovarian stimulation**, where ovaries become hyperstimulated, leading to **capillary permeability** and fluid shifts, resulting in ascites and potentially pleural effusions causing dyspnea. *PCOS* - While Polycystic Ovarian Syndrome (PCOS) involves multiple small follicles (usually 12 or more per ovary, each 2-9 mm in diameter), it typically does not present with acute symptoms like **ascites** and **dyspnea** unless severe OHSS occurs after ovulation induction in a woman with PCOS. - The ovaries in PCOS are generally smaller or normal size compared to the massively enlarged ovaries seen in the image, and the presence of significant ascites and dyspnea is not a direct feature of PCOS itself. *Theca lutein cyst* - **Theca lutein cysts** are usually **bilateral**, **multiloculated ovarian cysts** that result from exaggerated stimulation by **human chorionic gonadotropin (hCG)**, often seen in conditions like **gestational trophoblastic disease** or **multiple gestations**. - While they can be large and multicystic, the presentation with acute ascites and dyspnea in the context of infertility treatment points more specifically to OHSS. *Mucinous cystadenomas* - **Mucinous cystadenomas** are benign **epithelial ovarian tumors** that can grow very large and be multiloculated, but they are not typically associated with infertility treatment or the acute systemic symptoms of **ascites** and **dyspnea** via capillary leak syndrome. - Their presence would be coincidental rather than a direct complication of infertility therapy, and their fluid is usually thick and mucinous, enclosed within the cyst wall rather than causing diffuse fluid extravasation.
Question 5: What will be the Hysterosalpingogram (HSG) finding?
- A. Hydrosalpinx (Correct Answer)
- B. Cornual block
- C. Normal findings
- D. Bicornuate uterus
Explanation: ***Hydrosalpinx*** - The image, likely a hysterosalpingogram (HSG), shows a **dilated and fluid-filled fallopian tube** with no spillage of contrast into the peritoneal cavity, which is characteristic of hydrosalpinx. - The **contrast media fills the tubal lumen** but is unable to egress, indicating distal tubal obstruction and fluid accumulation. *Cornual block* - A cornual block would present as **obstruction at the uterine ostium** of the fallopian tube, preventing contrast from entering the tubal lumen. - In this image, contrast has clearly entered and dilated the fallopian tube, ruling out a cornual block. *Normal findings* - Normal HSG findings would show **patent fallopian tubes** with free spill of contrast into the peritoneal cavity. - The visible **dilation** and **lack of spill** in the image are distinctly abnormal. *Bicornuate uterus* - A bicornuate uterus is a **congenital uterine anomaly** characterized by two separate uterine horns. - While the uterus appears somewhat irregular, the dominant feature is the dilated fallopian tube, which is not a hallmark of a bicornuate uterus.
Question 6: A 36-week pregnant lady with previous twin delivery. What is the Obstetric score?
- A. G2P1 (Correct Answer)
- B. G2P2
- C. G3P2
- D. G3P3
Explanation: ***G2P1*** - **Gravida (G)** refers to the total number of pregnancies, including the current one, so the current pregnancy (1) plus the previous twin delivery (1) equals **G2**. - **Parity (P)** refers to the number of times a woman has given birth to a fetus (or fetuses) beyond 20 weeks gestation, irrespective of whether the baby was born alive or is now living. A **twin delivery counts as one parity event** because it was one pregnancy that resulted in a delivery. *G2P2* - This option incorrectly counts the twin delivery as two separate parity events, whereas **parity is counted per pregnancy event** resulting in live birth or stillbirth beyond 20 weeks. - While G2 is correct (current pregnancy + previous pregnancy), P2 incorrectly implies two separate delivery events. *G3P2* - This option correctly identifies the parity as P2, but incorrectly states the gravida as G3. - **Gravida is 2** (current pregnancy + previous twin pregnancy), not 3. *G3P3* - This option is incorrect for both gravida and parity. - The patient has had **two pregnancies** (G2) and **one delivery event** (P1).
Question 7: Which distension medium is used for hysteroscopy with bipolar cautery?
- A. NS (Correct Answer)
- B. Glycine
- C. Carbon Dioxide
- D. Dextran 70
Explanation: ***NS*** - **Normal Saline (NS)** is an **electrolyte-containing solution** (0.9% NaCl) and is thus safe to use with **bipolar electrosurgery** because it does not conduct current across the tissue but only between the two poles of the instrument. - Its isotonicity minimizes fluid shifts and its clear nature allows for good visualization. *Glycine* - **Glycine** is a **non-electrolyte solution** that is used with **monopolar electrosurgery**, as it does not conduct electrical current to the patient but only through the active electrode. - Using it with bipolar devices is unnecessary and can lead to complications such as **dilutional hyponatremia** and **hyperammonemia** if significant intravascular absorption occurs. *Carbon Dioxide* - **Carbon dioxide** is used as a distension medium for **diagnostic hysteroscopy** because of its lack of risk for fluid overload and clear visualization. - It is **contraindicated with electrosurgery** because of the risk of **gas embolism** and its potential for impaired visualization with significant bleeding. *Dextran 70* - **Dextran 70** is a **high-viscosity, non-electrolyte solution** primarily used for diagnostic hysteroscopy when blood or mucus obscures the view. - It is **contraindicated for electrosurgery** due to its non-conductive nature and the risk of **anaphylactic reactions** and **pulmonary edema** from volume expansion.
Question 8: 60-year-old female with a history of intermittent bleeding. What is the diagnosis based on the ultrasound image?
- A. Endometrial polyp (Correct Answer)
- B. Ca endometrium
- C. Submucosal fibroid
- D. Endometrial hyperplasia
Explanation: ***Endometrial polyp*** - The ultrasound image shows a well-defined, **echogenic focal lesion within the endometrial cavity**, which is characteristic of an endometrial polyp. - In a 60-year-old female with intermittent bleeding, a polyp is a common cause of **postmenopausal bleeding** and is often identified as an intracavitary mass on ultrasound. - Endometrial polyps appear as **focal, hyperechoic or isoechoic masses** with a smooth contour projecting into the endometrial cavity. *Ca endometrium* - **Endometrial carcinoma** typically appears as diffuse endometrial thickening (>4-5 mm in postmenopausal women), irregular endometrial-myometrial interface, or heterogeneous endometrial echoes, often with evidence of myometrial invasion. - While bleeding is a cardinal symptom of endometrial carcinoma, the distinct **focal, well-circumscribed nature** of the lesion on ultrasound is less typical for carcinoma, which tends to be more diffuse and irregular. *Submucosal fibroid* - A **submucosal fibroid** (leiomyoma) is a benign smooth muscle tumor originating from the myometrium that protrudes into the endometrial cavity. - While it can appear as an intracavitary mass and cause abnormal bleeding, fibroids often have a more **heterogeneous or hypoechoic appearance** with posterior acoustic shadowing, compared to the isoechoic to hyperechoic appearance of a polyp. - The feeding vessel sign (blood flow at the base) is more characteristic of polyps than fibroids. *Endometrial hyperplasia* - **Endometrial hyperplasia** presents as **diffuse, uniform endometrial thickening** rather than a focal intracavitary mass. - It typically shows homogeneous increased echogenicity of the entire endometrium without a discrete, well-defined lesion as seen with a polyp. - While it can cause postmenopausal bleeding, the focal nature of the lesion in this case makes hyperplasia less likely.
Question 9: A sexually active female presenting with profuse frothy foul-smelling discharge with intense itching. Strawberry cervix revealed on examination. What will be the diagnosis?
- A. Trichomonas vaginalis (Correct Answer)
- B. Bacterial vaginosis
- C. Candidiasis
- D. None of the options
Explanation: **Trichomonas vaginalis** - The classic presentation of **profuse, frothy, foul-smelling vaginal discharge** with **intense itching** and the presence of a **strawberry cervix** are highly characteristic of a *Trichomonas vaginalis* infection. - *Trichomonas vaginalis* is a **motile protozoan** and a common sexually transmitted infection. *Bacterial vaginosis* - While bacterial vaginosis (BV) causes a **foul-smelling discharge** (often described as "fishy"), it is typically **thin and grayish-white**, not frothy, and does not cause a strawberry cervix. - BV is caused by an **overgrowth of anaerobic bacteria** and a decrease in lactobacilli, leading to an elevated vaginal pH. *Candidiasis* - Candidiasis (yeast infection) presents with a **thick, white, "cottage cheese-like" discharge** and intense itching, but the discharge is usually odorless and it does not cause a frothy discharge or strawberry cervix. - It is caused by an **overgrowth of *Candida* species**, primarily *Candida albicans*, and is not typically sexually transmitted. *None of the options* - Given the classic constellation of symptoms and definitive signs, a specific diagnosis can be made, making this option incorrect.
Question 10: What is the use of the instrument shown in the image?
- A. Laparoscopic sterilization (Correct Answer)
- B. Surgical removal of ectopic pregnancy
- C. Induction of abortion
- D. Creating pneumoperitoneum for laparoscopic procedures
Explanation: ***Laparoscopic sterilization*** - The image depicts a **laparoscopic clip applicator**, specifically designed for placing clips on structures like the **fallopian tubes** during laparoscopic sterilization procedures. - This instrument is used to permanently occlude the fallopian tubes, preventing the passage of eggs and sperm for effective **contraception**. *Surgical removal of ectopic pregnancy* - While an ectopic pregnancy can be removed laparoscopically, the instrument shown is a **clip applicator**, not typically used for dissecting or excising tissue in such a procedure. - Surgical removal of an ectopic pregnancy often involves **laparoscopic salpingostomy** or **salpingectomy**, which require cutting, grasping, and coagulating instruments. *Induction of abortion* - **Abortion induction** is typically performed using medical methods (medications) or surgical procedures like **dilation and curettage (D&C)** or **manual vacuum aspiration (MVA)**, none of which involve the specific instrument shown. - This instrument is designed for **occlusion** rather than tissue removal related to abortion. *Creating pneumoperitoneum for laparoscopic procedures* - **Pneumoperitoneum** is created using a **Veress needle** to insufflate carbon dioxide into the abdominal cavity, providing a working space for laparoscopic instruments. - The instrument shown is a **clip applicator**, not a needle for gas insufflation.