NEET-PG 2020 — Microbiology
12 Previous Year Questions with Answers & Explanations
Which interleukin is primarily responsible for inducing IgE production from B cells?
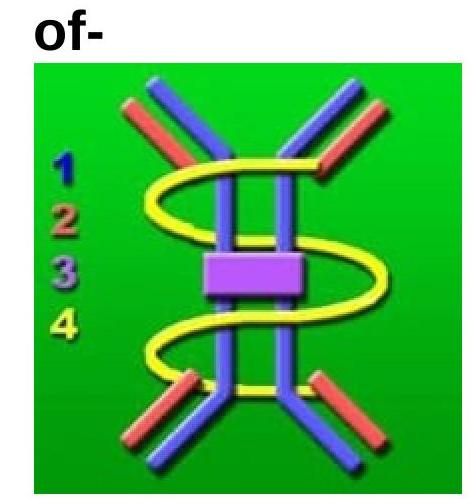
The image of an immunoglobulin is shown below. Which type of immunoglobulin is it?
Identify the parasite shown in the image.
Which of the following cell components produced by Neisseria gonorrhoeae is responsible for attachment to host cells?
Which of the following does not possess superantigen properties?
Fungal infection which is acquired by traumatic inoculation is?
A 15-year-old boy presented with fever and chills for 3 days. On examination, he was found to have delayed skin pinch time and dry oral mucosa. Identify the pathogen involved based on the provided peripheral blood smear image.
Superantigen is produced by which of the following?
A 29 year old male was brought to ED with complaints of nausea, vomiting and abdominal cramps 3-4 hours after eating meat at dinner. What is the likely cause of this condition?
A 12 year old boy presents with vomiting within 3 hours of consumption of food at a party. What is the likely causative organism responsible for the symptoms?
NEET-PG 2020 - Microbiology NEET-PG Practice Questions and MCQs
Question 1: Which interleukin is primarily responsible for inducing IgE production from B cells?
- A. IL-1 and IL-3
- B. IL-3
- C. IL-1
- D. IL-4 (Correct Answer)
Explanation: ***IL-4*** - **IL-4** is the primary cytokine responsible for promoting B cell differentiation into **plasma cells** that produce **IgE antibodies**. - It plays a crucial role in the development of **allergic reactions** by stimulating IgE class switching. *IL-1* - **IL-1** is a pro-inflammatory cytokine primarily involved in the **innate immune response**, fever, and acute phase reactions. - It does not directly induce IgE production but can modulate immune responses in a broader context. *IL-3* - **IL-3** is a cytokine that primarily supports the growth and differentiation of **hematopoietic stem cells** in the bone marrow. - It is crucial for the development of various blood cell lineages but is not directly involved in IgE class switching. *IL-1 and IL-3* - While both **IL-1** and **IL-3** have important roles in immunity and hematopoiesis, neither directly induces **IgE production** from B cells. - **IL-4** is the specific and most significant interleukin for this function.
Question 2: The image of an immunoglobulin is shown below. Which type of immunoglobulin is it?
- A. Immunoglobulin A (IgA) (Correct Answer)
- B. Immunoglobulin G (IgG)
- C. Immunoglobulin M (IgM)
- D. Immunoglobulin E (IgE)
Explanation: ***Immunoglobulin A (IgA)*** - The image depicts two Y-shaped immunoglobulin monomers linked by a central purple component, which represents the **J-chain**, and enveloped by a yellow structure, which represents the **secretory component**. This **dimeric** structure with a secretory component is characteristic of secretory IgA. - **Secretory IgA** is primarily found in mucosal secretions such as saliva, tears, breast milk, and gastrointestinal fluids, where it plays a crucial role in **mucosal immunity** by preventing pathogen adhesion. *Immunoglobulin G (IgG)* - IgG exists as a **monomer** (single Y-shaped unit) in its functional form. - It is the most abundant immunoglobulin in serum and plays a major role in **secondary immune responses** and can cross the placenta. *Immunoglobulin M (IgM)* - In serum, IgM typically exists as a **pentamer**, meaning five Y-shaped units are joined together by a J-chain, forming a star-like structure. - It is the first antibody produced in a **primary immune response** and is effective in complement activation. *Immunoglobulin E (IgE)* - IgE exists as a **monomer** and is primarily associated with **allergic reactions** and defense against parasites. - It binds to receptors on mast cells and basophils, triggering immune responses upon allergen exposure.
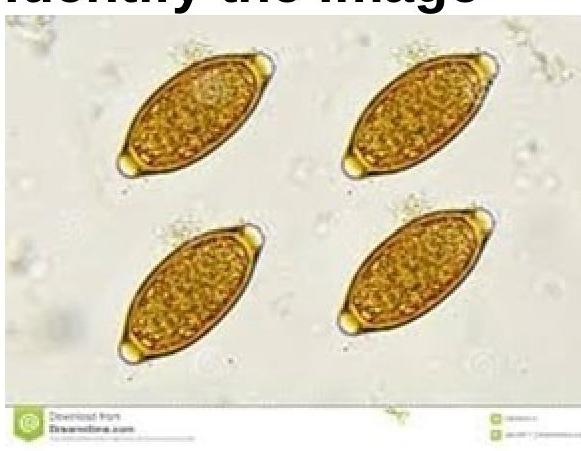
Question 3: Identify the parasite shown in the image.
- A. Trichuris trichiura (Correct Answer)
- B. Ancylostoma duodenale
- C. Strongyloides stercoralis
- D. Paragonimus westermani
Explanation: ***Trichuris trichiura*** - The image displays characteristic **lemon-shaped** or **barrel-shaped eggs** with distinctive **polar plugs** at each end, which are pathognomonic for *Trichuris trichiura* (whipworm) eggs. - These eggs are thick-shelled and typically measure 50-55 µm by 20-25 µm, containing an undeveloped larva when passed in feces. *Ancylostoma duodenale* - Eggs of *Ancylostoma duodenale* (Old World hookworm) are **oval-shaped** with blunt ends, and a **thin shell**. - They typically contain a **segmented ovum** or an early-stage larva, lacking the polar plugs seen in the image. *Paragonimus westermani* - *Paragonimus westermani* (lung fluke) eggs are generally **oval-shaped** with a **flattened operculum** at one end, which is not visible in the image. - They are larger than *Trichuris* eggs, often measuring around 80-120 µm by 45-70 µm, and are often coughed up in sputum or passed in feces. *Strongyloides stercoralis* - *Strongyloides stercoralis* primarily produces **larvae** (rhabditiform or filariform) in stool samples rather than eggs. - If eggs are seen (rarely, in cases of severe diarrhea), they are small, thin-shelled, and typically contain a developed larva, unlike the eggs shown.
Question 4: Which of the following cell components produced by Neisseria gonorrhoeae is responsible for attachment to host cells?
- A. Lipooligosaccharide
- B. Pili (fimbriae) (Correct Answer)
- C. IgA1 protease
- D. Outer membrane porin protein
Explanation: ***Pili (fimbriae)*** - **Pili** are hair-like appendages on the surface of *Neisseria gonorrhoeae* that facilitate initial attachment to **eukaryotic host cells**, particularly epithelial cells in the genitourinary tract. - This attachment is crucial for **colonization** and preventing the bacteria from being washed away by bodily fluids. *Lipooligosaccharide* - **Lipooligosaccharide (LOS)** is a major component of the outer membrane of *Neisseria gonorrhoeae* that contributes to **virulence** through its endotoxin activity, causing inflammation and tissue damage. - While it's important for pathogenicity, its primary role isn't direct attachment but rather the **immune response modulation** and tissue invasion. *IgA1 protease* - **IgA1 protease** is an enzyme produced by *Neisseria gonorrhoeae* that cleaves **IgA1 antibodies**, which are found on mucosal surfaces. - This enzyme helps the bacteria **evade the host immune response** by destroying protective antibodies, not directly mediating cell attachment. *Outer membrane porin protein* - **Outer membrane porin proteins (Porins)** form channels in the outer membrane of *Neisseria gonorrhoeae*, allowing the passage of small molecules. - While important for bacterial metabolism and survival, porins are not the primary structures responsible for **initial host cell attachment**.
Question 5: Which of the following does not possess superantigen properties?
- A. Staphylococcal enterotoxins
- B. Vibrio cholerae (Correct Answer)
- C. Streptococcal pyrogenic exotoxins
- D. None of these
Explanation: ***Vibrio cholerae*** - This bacterium is primarily known for producing **cholera toxin**, which acts on the **adenylate cyclase** pathway to cause severe watery diarrhea. - While it produces powerful toxins, these do not function as **superantigens**, meaning they do not directly bind to MHC class II and T-cell receptors outside the antigen-binding groove. *Streptococcal pyrogenic exotoxins* - These toxins, produced by **Streptococcus pyogenes**, are well-known **superantigens** that cause symptoms such as **scarlet fever** and **streptococcal toxic shock syndrome**. - They bind directly to MHC class II molecules and T-cell receptors, leading to widespread T-cell activation and massive cytokine release. *Staphylococcal enterotoxins* - Produced by **Staphylococcus aureus**, these toxins are a classic example of **superantigens**, causing symptoms such as **food poisoning** and **toxic shock syndrome**. - They bypass conventional antigen presentation, nonspecifically activating a large proportion of T cells and inducing a massive inflammatory response. *None of these* - This option is incorrect because *Vibrio cholerae* stands out as the organism among the choices that does not produce superantigens. - Both streptococcal pyrogenic exotoxins and staphylococcal enterotoxins are well-established superantigens.
Question 6: Fungal infection which is acquired by traumatic inoculation is?
- A. Sporothrix (Correct Answer)
- B. Coccidioides
- C. Paracoccidioides
- D. Blastomyces
Explanation: ***Sporothrix*** - **Sporotrichosis** is characteristically acquired through **traumatic inoculation** of the fungus, often from contact with soil, thorns, or decaying vegetation. - The organism causes **cutaneous lymphatic disease**, presenting as nodular lesions along lymphatic drainage paths. *Blastomyces* - **Blastomycosis** is typically acquired by inhaling airborne fungal spores, usually from **soil rich in organic matter** or decaying wood. - It primarily affects the **lungs** and can disseminate to the skin, bones, and other organs, but is not primarily associated with traumatic inoculation. *Coccidioides* - **Coccidioidomycosis** (Valley Fever) is acquired by inhaling **arthroconidia** present in dust or soil in endemic areas. - It is a **pulmonary infection** that can disseminate to other body sites, and its entry is almost exclusively respiratory, not traumatic. *Paracoccidioides* - **Paracoccidioidomycosis** is acquired by inhaling airborne fungal propagules, typically found in **soil in Latin America**. - It primarily causes **chronic pulmonary disease** and can spread to mucous membranes, skin, and lymph nodes, with no known association with traumatic inoculation.
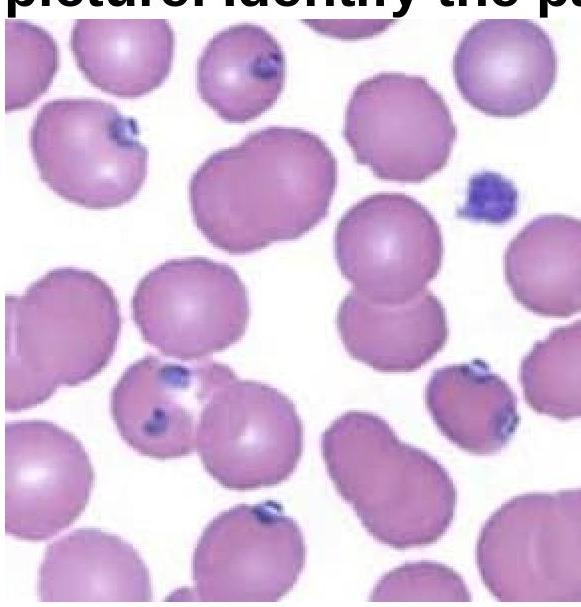
Question 7: A 15-year-old boy presented with fever and chills for 3 days. On examination, he was found to have delayed skin pinch time and dry oral mucosa. Identify the pathogen involved based on the provided peripheral blood smear image.
- A. Babesia
- B. Plasmodium vivax (Correct Answer)
- C. Plasmodium falciparum
- D. Salmonella typhi
Explanation: ***Plasmodium vivax*** - The image shows **enlarged red blood cells** infected with various stages of *Plasmodium vivax*, including trophozoites and schizonts displaying **ameboid forms**. - The presence of **Schüffner's dots**, though not distinctly visible in this specific resolution, is characteristic of *P. vivax* infection. - *P. vivax* preferentially infects **reticulocytes** and young red blood cells, leading to the characteristic RBC enlargement. *Babesia* - *Babesia* infection typically presents with **ring forms** in red blood cells that lack pigment and often form **tetrads** (Maltese cross appearance), which are not seen here. - While it can cause fever and chills, the morphology of the parasites in the image is inconsistent with *Babesia*. *Plasmodium falciparum* - *P. falciparum* characteristically presents with **multiple small ring forms** in a single red blood cell and **crescent-shaped gametocytes**. - It infects red blood cells of all ages, does not typically enlarge the red blood cells, and early trophozoites (*ring forms*) are the most common stage seen in peripheral blood, which differs from the image. *Salmonella typhi* - *Salmonella typhi* is a bacterium that causes **typhoid fever** and is a systemic infection. - It does not infect red blood cells or present with intraerythrocytic parasites on a peripheral blood smear; diagnosis is typically made by **blood culture**.
Question 8: Superantigen is produced by which of the following?
- A. Clostridium perfringens
- B. Vibrio cholerae
- C. Staphylococcus epidermidis
- D. Streptococcus pyogenes (Correct Answer)
Explanation: ***Streptococcus pyogenes*** - *Streptococcus pyogenes* produces **superantigens** such as **streptococcal pyrogenic exotoxins (SPE-A, SPE-B, SPE-C)**. - These superantigens cause massive non-specific T-cell activation, leading to **toxic shock syndrome** and **scarlet fever**. - Superantigens bypass normal antigen processing by directly binding MHC class II molecules to T-cell receptors. *Clostridium perfringens* - *Clostridium perfringens* primarily produces **alpha-toxin** (phospholipase C) and other toxins causing **gas gangrene** and **food poisoning**. - It does not produce superantigens. *Vibrio cholerae* - *Vibrio cholerae* produces **cholera toxin**, an **enterotoxin** that causes massive fluid secretion in the intestine, leading to profuse watery diarrhea. - Cholera toxin is not a superantigen; it acts by activating adenylate cyclase through ADP-ribosylation. *Staphylococcus epidermidis* - *Staphylococcus epidermidis* is a common skin commensal that can cause infections related to **medical devices** and **biofilm formation**. - Unlike *Staphylococcus aureus* (which produces TSST-1 and enterotoxins), *S. epidermidis* does not produce superantigens.
Question 9: A 29 year old male was brought to ED with complaints of nausea, vomiting and abdominal cramps 3-4 hours after eating meat at dinner. What is the likely cause of this condition?
- A. Clostridium perfringens
- B. Clostridium botulinum
- C. Staphylococcus aureus (Correct Answer)
- D. Salmonella Enteritidis
Explanation: ***Staphylococcus aureus*** - The rapid onset of symptoms (3-4 hours) after eating meat, characterized by **nausea**, **vomiting**, and **abdominal cramps**, is highly suggestive of preformed toxin-mediated food poisoning, with **Staphylococcus aureus** being a common culprit. - *S. aureus* produces heat-stable enterotoxins that, when ingested, cause prompt gastrointestinal symptoms due to their direct irritant effect on the gut. *Clostridium perfringens* - This bacterium typically causes food poisoning with an incubation period of **8-16 hours** and symptoms primarily include **abdominal cramps** and **diarrhea**, with vomiting being less common. - Symptoms arise from toxins produced *in vivo* after spore ingestion, not preformed toxins, which leads to a longer incubation time. *Clostridium botulinum* - While *Clostridium botulinum* produces a potent neurotoxin, its food poisoning primarily manifests as **neurological symptoms** (e.g., flaccid paralysis, diplopia, dysphagia), not acute gastrointestinal upset like vomiting and cramps. - The incubation period is typically **12-36 hours**, longer than the reported 3-4 hours, and it is usually associated with improperly canned foods. *Salmonella Enteritidis* - *Salmonella* infections usually have a longer incubation period of **6 hours to 6 days**, and while they can cause nausea, vomiting, cramps, and diarrhea, the rapid onset in this case makes *S. aureus* more likely. - Infection typically leads to **inflammatory gastroenteritis**, sometimes with fever, which is not mentioned as a prominent symptom here.
Question 10: A 12 year old boy presents with vomiting within 3 hours of consumption of food at a party. What is the likely causative organism responsible for the symptoms?
- A. Staphylococcus aureus (Correct Answer)
- B. Clostridium perfringens
- C. Clostridium botulinum
- D. Salmonella
Explanation: ***Staphylococcus aureus*** - **Vomiting occurring within 1-6 hours of food consumption** is highly characteristic of preformed toxin ingestion, commonly associated with *S. aureus*. - *S. aureus* produces **heat-stable enterotoxins** that cause rapid onset nausea, vomiting, and abdominal cramps. *Clostridium perfringens* - This bacterium typically causes symptoms like **abdominal cramps and diarrhea**, with vomiting being less common. - The onset of illness from *C. perfringens* is usually **8-16 hours** after consumption, which is longer than the 3-hour window in this case. *Clostridium botulinum* - *C. botulinum* causes **botulism**, a neuroparalytic illness, which may include nausea and vomiting in its early stages but is primarily characterized by **flaccid paralysis**. - Symptoms usually appear **12-36 hours** after exposure, which is much longer than the presentation described. *Salmonella* - **Salmonellosis** typically has an incubation period of **6-72 hours**, with symptoms including diarrhea, fever, and abdominal cramps; vomiting may occur but is not as immediate or predominant as with *S. aureus* toxin. - The illness is caused by bacterial colonization and invasion, not preformed toxins, leading to a longer onset compared to the 3-hour presentation.