Patient presented with diarrhoea, poor appetite and malabsorption. His duodenal biopsy was taken which showed crypt hyperplasia, villi atrophy and infiltration of CD8+ T cells in the epithelium. What is the likely diagnosis of the patient?
A patient posted for Lap Cholecystectomy had drug eluting stent placed two years back. Patient has no symptoms since then. Which of the following set of investigation should be done in this patient?
In comparison to a normal healthy person, in the evening time, which of these will have an elevated ACTH as well as elevated Cortisol?
A person was brought to emergency department and was diagnosed with Supra ventricular tachycardia and suddenly he became unstable. What is the next line of management?
A lesion was seen on the face of a 42 year old patient as shown below. Which of the following would be ideal management for this condition?
On esophageal manometry, spastic contractions in the esophageal body with a distal contractile integral (DCI) >8000 mmHg*s*cm are diagnostic of:
Which is not seen in heart failure?
A 30-year-old female complaints of fatigue and is unable to gain weight. On examination, her body felt warm. Which of the following investigation can be helpful in reaching the diagnosis?
A boy after playing football complaining fatigue and abdominal pain. He also had a history of hand swelling in past. On ultrasonography, he has shrunken spleen. What is the likely diagnosis of this patient?
Frontal gyrus lesion leads to?
NEET-PG 2020 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 51: Patient presented with diarrhoea, poor appetite and malabsorption. His duodenal biopsy was taken which showed crypt hyperplasia, villi atrophy and infiltration of CD8+ T cells in the epithelium. What is the likely diagnosis of the patient?
- A. Celiac disease (Correct Answer)
- B. Whipple disease
- C. Environmental enteropathy
- D. Pancreatitis
Explanation: ***Celiac disease*** - The combination of **diarrhoea**, **malabsorption**, **villi atrophy**, **crypt hyperplasia**, and **CD8+ T-cell infiltration** in the duodenal epithelium is pathognomonic for celiac disease [1]. - This condition is triggered by **gluten ingestion**, leading to an immune-mediated enteropathy [1], [3]. *Whipple disease* - Characterized by **malabsorption**, fever, arthralgia, and neurological symptoms [2]. - Histologically, it shows **foamy macrophages** containing PAS-positive material (Tropheryma whipplei) in the lamina propria, not primarily CD8+ T-cell infiltration [2]. *Environmental enteropathy* - Also known as tropical enteropathy, it causes **villi atrophy** and malabsorption, particularly in individuals living in areas with poor sanitation. - However, the prominent feature is often a diffuse inflammatory infiltrate, and specific **CD8+ T-cell infiltration** in the epithelium is not as specific as in celiac disease. *Pancreatitis* - Presents with **abdominal pain**, nausea, and vomiting, and can lead to malabsorption due to pancreatic enzyme insufficiency. - Histology of the duodenum would typically be normal, as the pathology primarily involves the **pancreas**, not the duodenal mucosa itself.
Question 52: A patient posted for Lap Cholecystectomy had drug eluting stent placed two years back. Patient has no symptoms since then. Which of the following set of investigation should be done in this patient?
- A. Coronary angiography, Thallium scan
- B. ECG, CBC, Coronary angiography
- C. ECG, CBC, Stress echocardiography (Correct Answer)
- D. ECG, CBC, Stress echocardiography, coronary angiography
Explanation: **ECG, CBC, Stress echocardiography** - A patient with a **drug-eluting stent (DES)** placed two years prior, who is now asymptomatic, typically requires a **non-invasive cardiac assessment** before surgery. [1] - **Stress echocardiography** is an appropriate investigation to assess for inducible ischemia in an asymptomatic patient with a history of DES, especially when determining readiness for non-cardiac surgery. [1] *Coronary angiography, Thallium scan* - **Coronary angiography** is an invasive procedure and is generally not indicated for asymptomatic patients two years post-DES unless there are new symptoms or high-risk findings on non-invasive tests. [2] - A **Thallium scan** (myocardial perfusion scintigraphy) is a valid stress test, but **stress echocardiography** provides similar information regarding ischemia and ventricular function without radiation exposure. [1] *ECG, CBC, Coronary angiography* - While **ECG** and **CBC** are standard preoperative tests, **coronary angiography** is an invasive procedure and is not the first-line investigation for an asymptomatic patient two years post-DES without other indications. [2] - The patient's asymptomatic status suggests that invasive testing is not immediately warranted for surgical clearance. *ECG, CBC, Stress echocardiography, coronary angiography* - Performing both **stress echocardiography** and **coronary angiography** in an asymptomatic patient two years after DES placement is **redundant** and subjects the patient to an unnecessary invasive procedure. [1], [2] - The results of a non-invasive stress test like stress echocardiography would guide the need for any further invasive intervention.
Question 53: In comparison to a normal healthy person, in the evening time, which of these will have an elevated ACTH as well as elevated Cortisol?
- A. Addison's disease
- B. Cushing's disease (Correct Answer)
- C. Transient state after exercise (evening time)
- D. Normal healthy person (evening time)
Explanation: **_Cushing's disease_** * In **Cushing's disease**, there is an **ACTH-producing pituitary adenoma** that leads to excessive ACTH secretion, which in turn stimulates the adrenal glands to produce high levels of cortisol. * This results in **chronically elevated cortisol levels** throughout the day, including the evening, and an inappropriately elevated ACTH due to increased production from the pituitary. *Addison's disease* * **Addison's disease** is characterized by **primary adrenal insufficiency**, meaning the adrenal glands cannot produce sufficient cortisol despite adequate ACTH stimulation. * While ACTH would be significantly **elevated** due to a lack of negative feedback from cortisol, the **cortisol levels would be low** or normal in response to the adrenal gland dysfunction. *Transient state after exercise (evening time)* * During and immediately after **intense exercise**, both ACTH and cortisol levels can transiently increase as part of the body's stress response. * However, these elevations are typically **transient** and would not represent a sustained, pathologically elevated state in the evening in the same way as Cushing's disease, and levels would usually normalize relatively quickly. *Normal healthy person (evening time)* * In a normal healthy person, ACTH and cortisol levels exhibit a **diurnal rhythm**, with the highest levels in the morning and the lowest levels in the late evening/night. * Therefore, in the evening, both **ACTH and cortisol levels would naturally be low** as part of the physiological circadian rhythm, not elevated.
Question 54: A person was brought to emergency department and was diagnosed with Supra ventricular tachycardia and suddenly he became unstable. What is the next line of management?
- A. Intravenous ibutilide
- B. Intravenous Diltiazem
- C. DC Cardioversion (Correct Answer)
- D. Intravenous Flecainide
Explanation: ***DC Cardioversion*** - For **unstable supraventricular tachycardia (SVT)**, immediate **direct current (DC) cardioversion** is the definitive treatment to restore sinus rhythm. - Instability in SVT includes symptoms like hypotension, altered mental status, signs of shock, ischemic chest discomfort, or acute heart failure. *Intravenous ibutilide* - **Ibutilide** is an antiarrhythmic drug used for pharmacological cardioversion of recent-onset atrial fibrillation or flutter, but not typically for unstable SVT. - While it can convert certain supraventricular arrhythmias, it is generally reserved for **stable patients** and takes longer to act than immediate electrical cardioversion. *Intravenous Diltiazem* - **Diltiazem** is a calcium channel blocker used to control ventricular rate in **stable SVT**, atrial fibrillation, or flutter [1]. - It is contraindicated in unstable patients as it can further depress cardiac contractility and worsen hypotension [2]. *Intravenous Flecainide* - **Flecainide** is a class Ic antiarrhythmic drug used to maintain sinus rhythm in patients with supraventricular arrhythmias, including SVT. - It also takes time to act and is used in **stable patients** without structural heart disease, not in emergency unstable situations where immediate rhythm conversion is required.
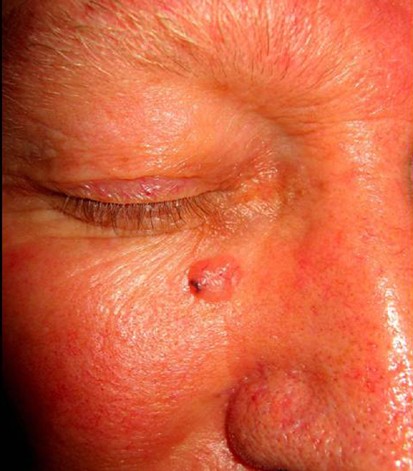
Question 55: A lesion was seen on the face of a 42 year old patient as shown below. Which of the following would be ideal management for this condition?
- A. Topical retinoids
- B. Oral steroids
- C. Start on MDT for leprosy
- D. Start on ATT (Correct Answer)
Explanation: ***Start on ATT*** - The presented image shows a **gummy lesion** on the face, which is characteristic of **tuberculosis cutis colliquativa**, a form of cutaneous tuberculosis. - **Anti-tubercular therapy (ATT)** is the primary and most effective treatment for all forms of tuberculosis, including cutaneous manifestations. *Topical retinoids* - Topical retinoids are primarily used for **acne vulgaris** and certain **disorders of keratinization** and are not indicated for infectious granulomatous conditions. - They work by **regulating cell growth and differentiation**, which is not the mechanism required to treat tuberculosis. *Oral steroids* - Oral steroids are **immunosuppressive** and generally contraindicated in active infections like tuberculosis, as they can worsen the disease. - While they might be used short-term in some inflammatory skin conditions, they would **not address the underlying tuberculous infection**. *Start on MDT for leprosy* - **Multi-drug therapy (MDT)** is the standard treatment for leprosy, which also presents with skin lesions and nerve involvement. - However, the image shows a **single, nodular, ulcerated lesion** more typical of cutaneous tuberculosis rather than the varied forms of leprosy (macular, papular, nodular lesions, or nerve thickening).
Question 56: On esophageal manometry, spastic contractions in the esophageal body with a distal contractile integral (DCI) >8000 mmHg*s*cm are diagnostic of:
- A. Jackhammer esophagus
- B. Type II achalasia
- C. Type III achalasia (Correct Answer)
- D. Type I achalasia
Explanation: ***Type III achalasia*** - This diagnosis is characterized by the presence of **spastic contractions** in the esophageal body, specifically with a **distal contractile integral (DCI) greater than 8000 mmHg*s*cm**, alongside the classic features of achalasia (impaired LES relaxation and absent peristalsis) [1]. - The elevated DCI reflects the **premature and simultaneous contractions** that are hallmark of this subtype, distinguishing it from other motility disorders [1]. *Jackhammer esophagus* - While it also involves very strong esophageal contractions (**high DCI**), jackhammer esophagus (also known as hypercontractile esophagus) does **not present with impaired LES relaxation or absent peristalsis** as seen in achalasia. - The defining feature of jackhammer esophagus is **multiple rapid swallows** (MRS) that induce simultaneous contractions, often with very high vigor. *Type II achalasia* - This type of achalasia is defined by **pan-esophageal pressurization** in more than 20% of swallows, along with impaired LES relaxation and absent peristalsis. - Unlike Type III, it does **not show the spastic hypercontractile activity** in the esophageal body revealed by a very high DCI. *Type I achalasia* - This is the classic form of achalasia characterized by **absent esophageal peristalsis** and **impaired lower esophageal sphincter (LES) relaxation**, without significant esophageal pressurization or spastic contractions [1]. - It represents the most common subtype and lacks the **high DCI spastic activity** seen in Type III achalasia.
Question 57: Which is not seen in heart failure?
- A. Cardiomegaly
- B. Kerley B lines
- C. Kerley A Lines
- D. Oligemia (Correct Answer)
Explanation: ***Oligemia*** - **Oligemia** refers to a reduced blood volume or total blood flow to a region, which is typically not observed in **heart failure**. - In **heart failure**, the body often experiences **fluid overload** and **pulmonary congestion**, leading to increased blood volume in the lungs, not reduced [1]. *Cardiomegaly* - **Cardiomegaly**, or an enlarged heart, is a common finding in **heart failure** as the heart muscle remodels and dilates to compensate for impaired pumping function [1], [3]. - This can be seen on a chest X-ray as an **increased cardiothoracic ratio** [1], [2]. *Kerley B lines* - **Kerley B lines** are thin, horizontal lines visible on a chest X-ray, typically found at the lung periphery. - They indicate **interstitial edema** due to increased pulmonary venous pressure, a characteristic sign of **pulmonary congestion** in **heart failure** [1]. *Kerley A Lines* - **Kerley A lines** are longer, less common lines seen radiating from the hila towards the upper lobes. - These lines represent **distended anastomotic channels** between pulmonary and systemic venous systems, also indicative of **pulmonary edema** and **heart failure** [1], [4].
Question 58: A 30-year-old female complaints of fatigue and is unable to gain weight. On examination, her body felt warm. Which of the following investigation can be helpful in reaching the diagnosis?
- A. Elevated TSH with normal thyroid hormone levels
- B. Elevated TSH with low thyroid hormone levels
- C. Normal TSH with abnormal thyroid hormone levels
- D. Suppressed TSH with elevated thyroid hormone levels (Correct Answer)
Explanation: Suppressed TSH with elevated thyroid hormone levels - The patient's symptoms of **fatigue** (despite being warm) and **difficulty gaining weight**, coupled with her body feeling **warm**, are classic signs of **hyperthyroidism**. [1] - In hyperthyroidism, the thyroid gland produces **excessive thyroid hormones (T3 and T4)**, which in turn **suppresses TSH** production from the pituitary gland through negative feedback. [2] *Elevated TSH with normal thyroid hormone levels* - This pattern is characteristic of **subclinical hypothyroidism**, where the thyroid gland is beginning to fail, leading to increased TSH to maintain normal thyroid hormone levels. [3] - The patient's symptoms of feeling warm and difficulty gaining weight are inconsistent with hypothyroidism. [1] *Elevated TSH with low thyroid hormone levels* - This indicates **primary hypothyroidism**, where the thyroid gland is underactive and produces insufficient thyroid hormones, leading to a compensatory rise in TSH. [2] - Hypothyroidism typically presents with **weight gain**, **cold intolerance**, and fatigue, which contradict the patient's presentation. [1] *Normal TSH with abnormal thyroid hormone levels* - This scenario usually suggests **central hypothyroidism** (pituitary or hypothalamic dysfunction affecting TSH production) or **thyroid hormone resistance**. [3] - While possible in some rare cases, it does not fit the typical clinical picture of hyperthyroidism presented by the patient's symptoms.
Question 59: A boy after playing football complaining fatigue and abdominal pain. He also had a history of hand swelling in past. On ultrasonography, he has shrunken spleen. What is the likely diagnosis of this patient?
- A. Acute pancreatitis
- B. Sickle cell anemia (Correct Answer)
- C. Iron deficiency anemia
- D. Intermittent porphyria
Explanation: ### Sickle cell anemia - This patient's history of **hand swelling** (dactylitis), current **fatigue**, and **abdominal pain** are classic symptoms of sickle cell crises in **sickle cell anemia**. - The finding of a **shrunken spleen** on ultrasonography is consistent with **autosplenectomy**, a common complication of sickle cell disease due to repeated infarctions [1]. *Acute pancreatitis* - While acute pancreatitis can cause **severe abdominal pain**, it typically presents with elevated amylase/lipase, and does not explain the history of **hand swelling** or **shrunken spleen**. - There is no specific connection between playing football and developing acute pancreatitis in this context. *Iron deficiency anemia* - **Iron deficiency anemia** can cause **fatigue**, but it does not typically cause **abdominal pain**, **hand swelling**, or **autosplenectomy**. - A definitive diagnosis would require iron studies, which are not mentioned here. *Intermittent porphyria* - **Intermittent porphyria** can cause **abdominal pain** and neurological symptoms, but it does not manifest with **hand swelling** or **splenic atrophy**. - Its clinical presentation is distinctly different from the symptoms described.
Question 60: Frontal gyrus lesion leads to?
- A. Nominal aphasia
- B. Akinetic mutism
- C. Wernicke's aphasia
- D. Broca's aphasia (Correct Answer)
Explanation: ***Broca's aphasia*** - A lesion in the **frontal gyrus**, specifically **Broca's area** (Brodmann areas 44 and 45), leads to Broca's aphasia [1]. - This condition is characterized by **non-fluent speech**, difficulty with articulation, and telegraphic sentences, while comprehension remains relatively intact [1]. *Nominal aphasia* - This is also known as **anomic aphasia**, characterized primarily by difficulty with **word finding** (naming objects). - It results from lesions in various cortical areas, but typically not isolated to Broca's area in the frontal gyrus. *Akinetic mutism* - This condition involves a state of **unresponsiveness** where the patient is awake but does not move or speak. - It usually results from lesions in the **cingulate gyrus**, basal ganglia, or medial frontal lobes, often bilateral, not typically a solitary frontal gyrus lesion. *Wernicke's aphasia* - Wernicke's aphasia results from damage to **Wernicke's area**, located in the **posterior superior temporal gyrus** [1]. - It is characterized by **fluent but nonsensical speech** with impaired comprehension [1].