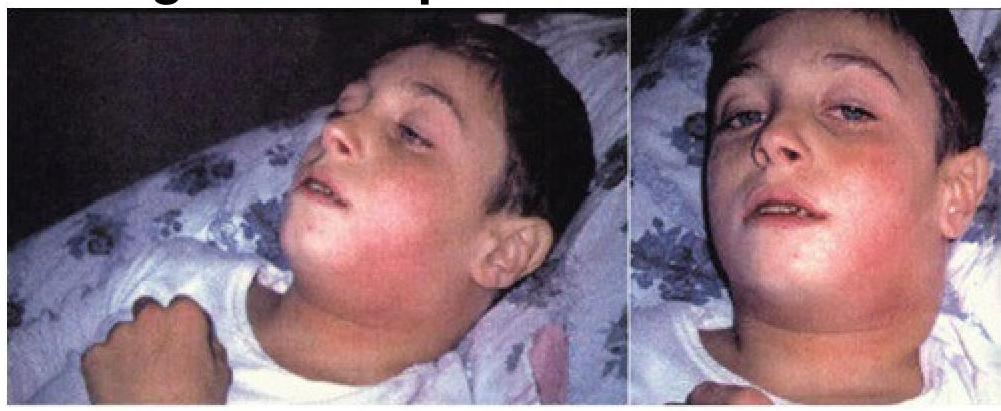
A patient with the following feature shown in the image. The patient reports having another 3-year-old sibling at home, who is fully immunized as per the immunization schedule. What is the best measure to prevent diphtheria in the sibling of the child with diphtheria?
Mission Indradhanush is for:
The difference between the incidence in the exposed and non-exposed group is best given by:
In a study of 200 patients, CA-125 testing was performed. Among the 100 patients who tested positive, 60 had ovarian cancer confirmed by histopathology. Among the 100 patients who tested negative, 20 had ovarian cancer confirmed by histopathology. What is the negative predictive value of this test?
Which of the following is an example of prospective screening?
What is the appropriate color for containers used to dispose of chemical liquid biomedical waste?
What is the target population for a Secondary Service Center as per the Vision 2020 initiative in India?
Admission rate bias is?
Nosocomial infections are defined as infections that develop after how many hours of hospital admission?
Which of the following is a technique/method based on behavioral sciences