NEET-PG 2020 — Anesthesiology
3 Previous Year Questions with Answers & Explanations
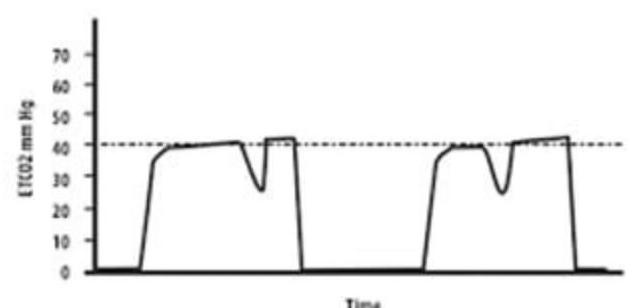
What does the image of the Capnograph depict?
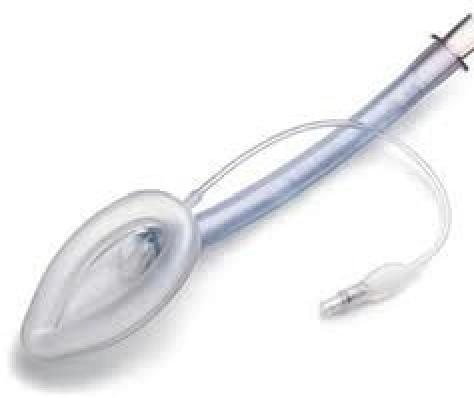
Identify the airway device shown in the image.
A patient scheduled for elective inguinal hernia surgery has a history of myocardial infarction (MI) and underwent coronary artery bypass grafting (CABG). What should be included in the preoperative assessment?
NEET-PG 2020 - Anesthesiology NEET-PG Practice Questions and MCQs
Question 1: What does the image of the Capnograph depict?
- A. Capnograph during inspiration
- B. Capnograph showing inspiration with cardiac oscillations
- C. Capnograph during expiration
- D. Capnograph indicating spontaneous respiration (Correct Answer)
Explanation: ***Capnograph indicating spontaneous respiration*** - The characteristic dip in the **EtCO2 waveform** during the plateau phase (phaselll) is indicative of a breath taken by the individual which is a classic finding of **spontaneous respiration**. This dip is because when a patient takes a breath in, fresh gas with no CO2 is pulled into the sampling line momentarily decreasing the measured CO2. - This pattern is often referred to as a "**curare cleft**" or "**respiratory indentation**," and it signifies incomplete paralysis or return of spontaneous breathing. *Capnograph during inspiration* - During normal inspiration, there is no CO2 in the inhaled air, so the capnograph reading would theoretically drop to **zero** or near-zero, not exhibit a waveform with a plateau. - The baseline of the capnograph reflects inspiration, which should be flat (zero CO2). *Capnograph showing inspiration with cardiac oscillations* - Cardiac oscillations typically appear as **small rhythmic fluctuations** on the baseline or the expiratory plateau, synchronized with the heartbeat. - These oscillations are usually much smaller and do not present as distinct, sharp dips within the expiratory plateau as seen in the image. *Capnograph during expiration* - During a normal expiration, the capnograph waveform rises from a baseline of zero (phase I, **dead space ventilation**) to a plateau (phase III, **alveolar gas emptying**) with a peak value, before returning to baseline during inspiration. - While the image shows expiration with a plateau, the key feature of the dip during the plateau is more specific to spontaneous respiration than just general expiration.
Question 2: Identify the airway device shown in the image.
- A. Nasopharyngeal Airway
- B. Cuffed Endotracheal Tube
- C. Guedel Airway
- D. Laryngeal Mask Airway (Correct Answer)
Explanation: ***Laryngeal Mask Airway*** - The image clearly displays a **Laryngeal Mask Airway (LMA)**, characterized by its inflatable, elliptical cuff designed to seal around the laryngeal inlet. - This supraglottic device is used for airway management in anesthesia and emergencies when endotracheal intubation is not required or feasible. *Nasopharyngeal Airway* - A **nasopharyngeal airway** is a soft, flexible tube inserted through the nose into the posterior pharynx. - It does not have an inflatable cuff or the broad, mask-like structure seen in the image. *Cuffed Endotracheal Tube* - A **cuffed endotracheal tube (ETT)** is a long, narrow tube inserted directly into the trachea, featuring a balloon cuff near the distal end for tracheal sealing. - The device in the image has a much broader, mask-like structure designed to sit above the larynx, not within the trachea. *Guedel Airway* - A **Guedel airway** (or oropharyngeal airway) is a rigid, curved device inserted into the mouth to prevent the tongue from obstructing the airway. - It is typically made of plastic and lacks any inflatable components or the sophisticated design of the device shown.
Question 3: A patient scheduled for elective inguinal hernia surgery has a history of myocardial infarction (MI) and underwent coronary artery bypass grafting (CABG). What should be included in the preoperative assessment?
- A. History + c/e + routine labs + V/Q scan
- B. History + c/e + routine labs
- C. History + c/e + routine labs + stress test (Correct Answer)
- D. History + c/e + routine labs + angiography to assess graft patency
Explanation: ***History + c/e + routine labs + stress test*** - A **stress test** is crucial in patients with a history of MI and CABG to assess **myocardial ischemia** and functional capacity, guiding perioperative management. - This evaluation helps determine the patient's **cardiac risk** for non-cardiac surgery and the need for further cardiac optimization. *History + c/e + routine labs + angiography to assess graft patency* - **Coronary angiography** is an invasive procedure and is generally not indicated as a routine preoperative assessment unless there are new, significant cardiac symptoms or signs of **graft dysfunction**. - Assessing graft patency through angiography carries risks and would only be justified if there were strong clinical indications suggesting acute or severe **cardiac ischemia**. *History + c/e + routine labs* - While critical for any preoperative assessment, **routine history, physical examination, and basic laboratory tests** are insufficient for a patient with a significant cardiac history like MI and CABG. - This approach would **underestimate the cardiac risk** and might miss undetected ischemia, leading to adverse perioperative cardiac events. *History + c/e + routine labs + V/Q scan* - A **ventilation-perfusion (V/Q) scan** is primarily used to diagnose **pulmonary embolism** or assess regional lung function. - It does not provide information about myocardial ischemia or cardiac functional capacity, making it **irrelevant** for assessing cardiac risk in this clinical scenario.