Which of the following statements about undescended testis is true?
A 45-year-old male is diagnosed with carcinoma of the penis. Which lymph nodes should the surgeon primarily consider for potential metastasis?
A 45-year-old male presenting with penile cancer extending up to the glans penis is treated with which of the following surgical options?
A young male presents with a testicular mass on the right side. The AFP is elevated while the HCG is normal. The most appropriate next step is
All of the following are true about Nissen Fundoplication except which of the following?
Which of the following statements about hypernephroma is true?
In which of the following surgeries is monopolar cautery preferred over bipolar cautery?
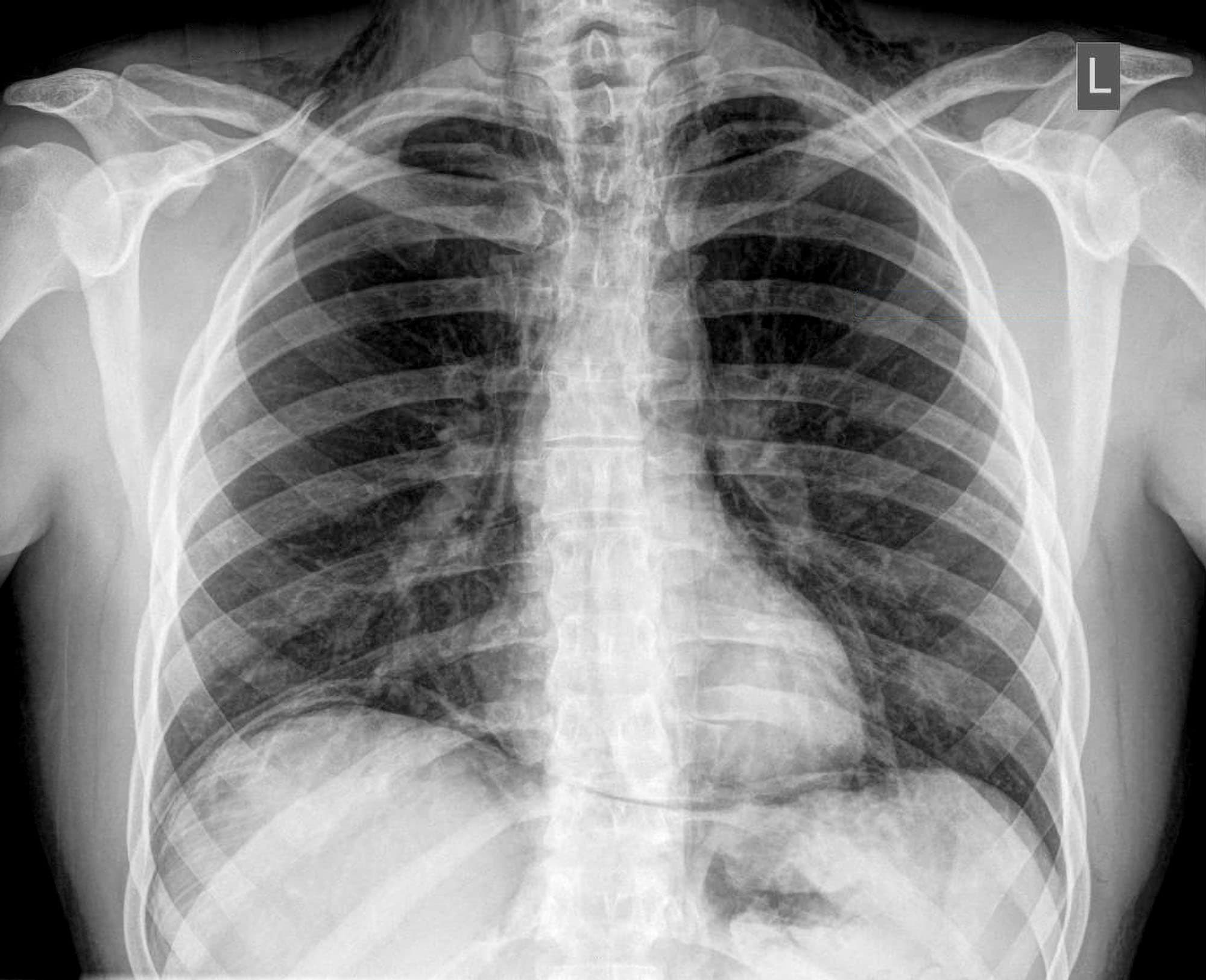
A patient presents with abdominal pain. On physical examination there was abdominal guarding and tenderness. A plain erect chest X-ray reveals air under diaphragm. Probable diagnosis is
What is the most common site of injury in an underwater blast?
Not true about gas gangrene: