Which of the following precancerous conditions, if treated, has the highest likelihood of not leading to cancer?
Most common antigen involved in erythroblastosis fetalis is:
Which of the following conditions is most commonly associated with malodorous vaginal discharge?
Hydrocephalus is best detected antenatally by :
What condition is diagnosed using the Amsel criteria?
Which of the following describes the points marked in the diagram of pelvic measurements?
Which of the following is not considered an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
NEET-PG 2015 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 61: Which of the following precancerous conditions, if treated, has the highest likelihood of not leading to cancer?
- A. Cervical intraepithelial Neoplasia (Correct Answer)
- B. Ductal carcinoma in situ of breast
- C. Lobular carcinoma in situ of breast
- D. Vaginal intraepithelial neoplasia
Explanation: ***Cervical intraepithelial neoplasia (CIN)*** - CIN has a high success rate with treatment (e.g., **cryotherapy**, **LEEP**), often completely eradicating the dysplastic cells and preventing progression to **invasive cervical cancer**. - The effectiveness of screening via **Pap smears** allows for early detection and intervention, significantly reducing cancer risk. *Ductal carcinoma in situ (DCIS) of breast* - While treatable, DCIS carries a higher risk of recurrence and progression to **invasive breast cancer** in the same or contralateral breast compared to CIN. - Treatment often involves **lumpectomy** with or without radiation, and sometimes **total mastectomy**, reflecting its more serious potential. *Lobular carcinoma in situ (LCIS) of breast* - LCIS is largely considered a **risk indicator** for future invasive cancer in either breast, rather than a direct precursor that inevitably progresses. - Management often involves **close surveillance** or **chemoprevention**, as surgical excision does not prevent cancer development in other areas of the breast. *Vaginal intraepithelial neoplasia (VAIN)* - While treatable, VAIN is less common and often coexists with or follows **cervical or vulvar neoplasia**, indicating a broader field defect due to **HPV**. - Recurrence rates post-treatment can be significant, and patients often require long-term follow-up due to the continued risk of progression.
Question 62: Most common antigen involved in erythroblastosis fetalis is:
- A. C antigen in Rh group
- B. E antigen in Rh group
- C. Duffy antigen
- D. D antigen in Rh group (Correct Answer)
Explanation: ***D antigen in Rh group*** - The **D antigen** is the most immunogenic of the Rh antigens and is responsible for the vast majority of cases of **erythroblastosis fetalis** (hemolytic disease of the fetus and newborn). - When an **Rh-negative mother** is exposed to Rh-positive fetal blood (usually during previous pregnancies or transfusions), she can form antibodies against the D antigen, which can then cross the placenta in subsequent pregnancies and attack Rh-positive fetal red blood cells. *C antigen in Rh group* - While the **C antigen** is part of the Rh blood group system, antibodies to it are much less common and typically cause less severe hemolytic disease compared to anti-D antibodies. - The C antigen is less immunogenic than the D antigen, meaning it is less likely to provoke an immune response in an Rh-negative individual. *E antigen in Rh group* - Similar to the C antigen, the **E antigen** is another Rh antigen, but antibodies against it (anti-E) are also less frequently implicated in severe erythroblastosis fetalis than anti-D. - Antibodies to E can cause hemolytic disease, but their clinical significance is usually milder than that of anti-D. *Duffy antigen* - The **Duffy antigen system** is separate from the Rh system and is known for its role in resistance to certain malarial parasites (e.g., *Plasmodium vivax*). - Although antibodies to Duffy antigens (anti-Fya, anti-Fyb) can cause **hemolytic disease of the fetus/newborn**, they are a far less common cause of erythroblastosis fetalis than antibodies to the Rh D antigen.
Question 63: Which of the following conditions is most commonly associated with malodorous vaginal discharge?
- A. Bacterial vaginosis (Correct Answer)
- B. Chlamydia trachomatis
- C. Trichomonas vaginalis
- D. Neisseria gonorrhoeae
Explanation: ***Bacterial vaginosis*** - This condition is characterized by a "fishy" or **malodorous vaginal discharge**, particularly noticeable after intercourse due to the release of amines. - It results from an imbalance in the vaginal flora, with an overgrowth of anaerobic bacteria and a decrease in protective lactobacilli. *Chlamydia trachomatis* - Often presents with **asymptomatic cervicitis** or mild watery discharge; **malodorous discharge** is not a common or prominent symptom. - While it can cause pelvic pain or dysuria, it's not typically associated with the characteristic smell of bacterial vaginosis. *Trichomonas vaginalis* - Can cause a **frothy, yellow-green discharge** that may be malodorous, but the "fishy" odor is more classically associated with bacterial vaginosis. - Other common symptoms include intense itching, burning, and dyspareunia. *Neisseria gonorrhoeae* - Causes cervicitis, which can lead to a **purulent or mucopurulent vaginal discharge**, but it does not typically produce the distinctive malodor seen in bacterial vaginosis. - Infection can also manifest as dysuria, pelvic pain, or be asymptomatic.
Question 64: Hydrocephalus is best detected antenatally by :
- A. X-ray abdomen
- B. Amniocentesis
- C. Clinical examination
- D. Ultrasonography (Correct Answer)
Explanation: ***Ultrasonography*** - **Antenatal ultrasonography** is the primary and most effective method for detecting fetal hydrocephalus. - It allows direct visualization of **ventricular dilation**, the key diagnostic finding in hydrocephalus (lateral ventricles >10mm at atrium level). - USG is **safe, non-invasive**, and can be performed repeatedly without radiation exposure. - It also helps identify associated anomalies and determine the cause of hydrocephalus. *X-ray abdomen* - **X-rays** expose the fetus to **ionizing radiation**, posing risks and violating ALARA (As Low As Reasonably Achievable) principles. - They provide limited detail of **soft tissue structures** like brain ventricles, making them unsuitable for diagnosing hydrocephalus. - X-rays are not used for antenatal diagnosis of fetal brain abnormalities. *Amniocentesis* - **Amniocentesis** is primarily used for **chromosomal analysis** and genetic testing, not for direct visualization of brain anomalies. - While some genetic conditions can lead to hydrocephalus, amniocentesis doesn't directly detect the hydrocephalus itself. - It cannot visualize structural fetal abnormalities. *Clinical examination* - **Antenatal clinical examination** of the mother cannot directly assess fetal brain abnormalities. - It may suggest fetal issues if there is an abnormally large uterine size or polyhydramnios, but it **lacks the specificity and sensitivity** to diagnose hydrocephalus. - Clinical examination alone is inadequate for detecting structural fetal anomalies.
Question 65: What condition is diagnosed using the Amsel criteria?
- A. Bacterial vaginosis (Correct Answer)
- B. Antiphospholipid antibody syndrome
- C. Ovarian ectopic pregnancy
- D. HELLP Syndrome
Explanation: ***Bacterial vaginosis*** - The **Amsel criteria** are specifically used for the clinical diagnosis of **bacterial vaginosis (BV)**. - The criteria include the presence of at least three of four findings: **homogeneous discharge**, **vaginal pH >4.5**, **positive whiff test**, and **clue cells** on microscopy. *Antiphospholipid antibody syndrome* - This syndrome is diagnosed based on **clinical criteria** (thrombosis, pregnancy morbidity) and the presence of persistent **antiphospholipid antibodies** (lupus anticoagulant, anti-cardiolipin, anti-β2-glycoprotein I antibodies). - It does not involve the use of the Amsel criteria. *Ovarian ectopic pregnancy* - Diagnosed primarily through **ultrasound imaging** showing a gestational sac or fetal heartbeat within the ovary, often accompanied by clinical symptoms like abdominal pain and vaginal bleeding. - This condition is not related to vaginal infections or the Amsel criteria. *HELLP Syndrome* - **HELLP syndrome** (Hemolysis, Elevated Liver enzymes, Low Platelets) is a severe obstetric complication usually occurring in pregnancy, diagnosed by **laboratory findings** of these specific abnormalities. - It is a systemic condition, not a vaginal infection, and does not use the Amsel criteria for diagnosis.
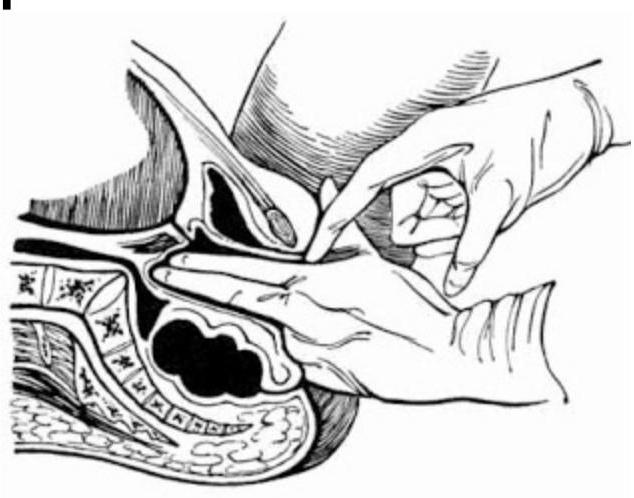
Question 66: Which of the following describes the points marked in the diagram of pelvic measurements?
- A. Diagonal conjugate (Correct Answer)
- B. Obstetric conjugate measurement
- C. True conjugate measurement
- D. Oblique conjugate measurement
Explanation: ***Diagonal conjugate*** - The image depicts a **bimanual examination** where one hand is inserted vaginally to measure the distance from the **lower border of the pubic symphysis** to the **sacral promontory**. - This measurement directly corresponds to the **diagonal conjugate**, which is a clinically estimated measurement of the pelvic inlet. *Obstetric conjugate measurement* - The **obstetric conjugate** is the smallest anteroposterior diameter through which the fetal head must pass. - It extends from the **middle of the sacral promontory** to the **innermost aspect of the pubic symphysis** and cannot be measured directly by clinical examination. *True conjugate measurement* - The **true conjugate**, also known as the anatomical conjugate, extends from the **sacral promontory** to the **upper border of the pubic symphysis**. - Like the obstetric conjugate, it is not directly palpable and must be estimated from the diagonal conjugate (true conjugate = diagonal conjugate - 1.5 to 2 cm). *Oblique conjugate measurement* - The **oblique conjugate** measures the distance between the sacroiliac joint on one side to the iliopectineal eminence on the opposite side. - This measurement is not typically assessed during a routine pelvic examination as depicted and is more relevant for identifying asymmetric pelvic deformities.
Question 67: Which of the following is not considered an absolute contraindication for the use of an Intra Uterine Contraceptive Device (IUD)?
- A. Undiagnosed vaginal bleeding
- B. Pregnancy
- C. Pelvic inflammatory disease
- D. Uterine malformation (Correct Answer)
Explanation: ***Uterine malformation*** - While a uterine malformation can make IUD insertion more difficult or reduce its effectiveness, it is often considered a **relative contraindication**, depending on the specific anomaly and the patient's desire for contraception. - In certain cases, an IUD might still be a viable option, but it requires careful consideration and specialized insertion techniques. *Pregnancy* - The presence of an existing pregnancy is an **absolute contraindication** for IUD insertion, as it can lead to complications such as miscarriage or ectopic pregnancy. - An IUD is a contraceptive device, and inserting it when a woman is already pregnant directly contradicts its purpose and poses significant risks. *Undiagnosed vaginal bleeding* - This is an **absolute contraindication** because it could be a symptom of a serious underlying condition, such as cervical cancer, endometrial cancer, or ectopic pregnancy. - Inserting an IUD before diagnosing the cause of the bleeding could delay treatment of a potentially life-threatening condition and exacerbate the bleeding. *Pelvic inflammatory disease* - Current or recent (within the last 3 months) **pelvic inflammatory disease (PID)** is an **absolute contraindication** due to the increased risk of worsening infection. - IUD insertion can introduce bacteria from the vagina into the uterus, potentially exacerbating an existing infection or causing a new one.