Identify the type of joint in the image provided.
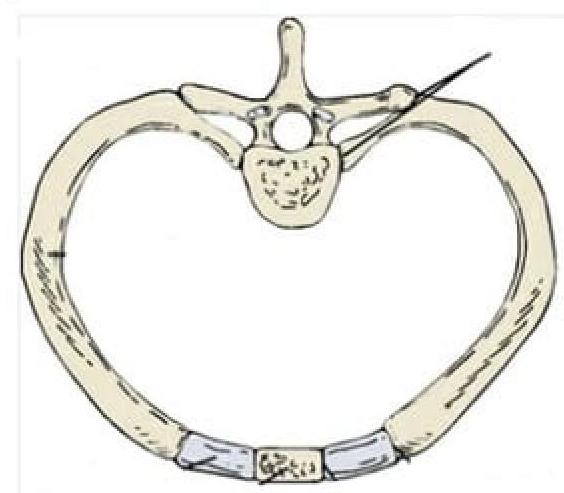
Identify the marked structure in the image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
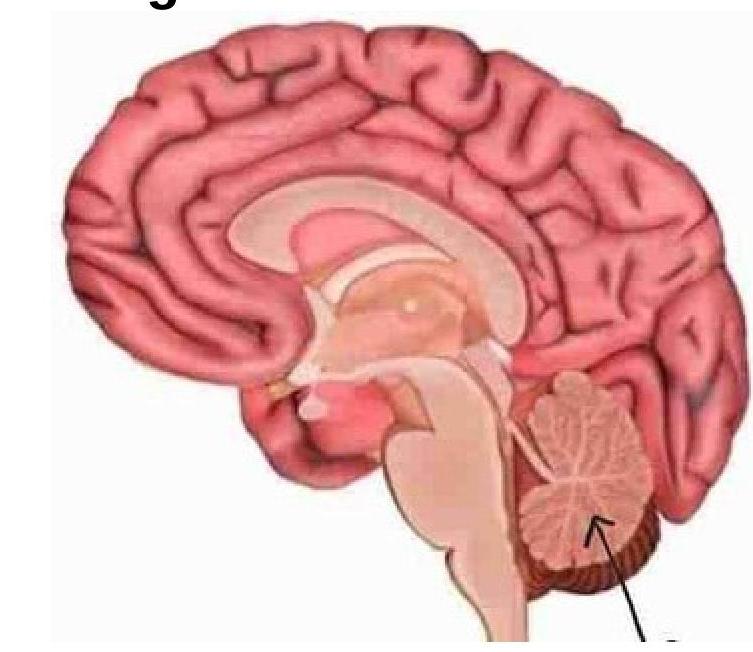
Identify the type of joint in the image provided.

Identify the marked structure in the image.

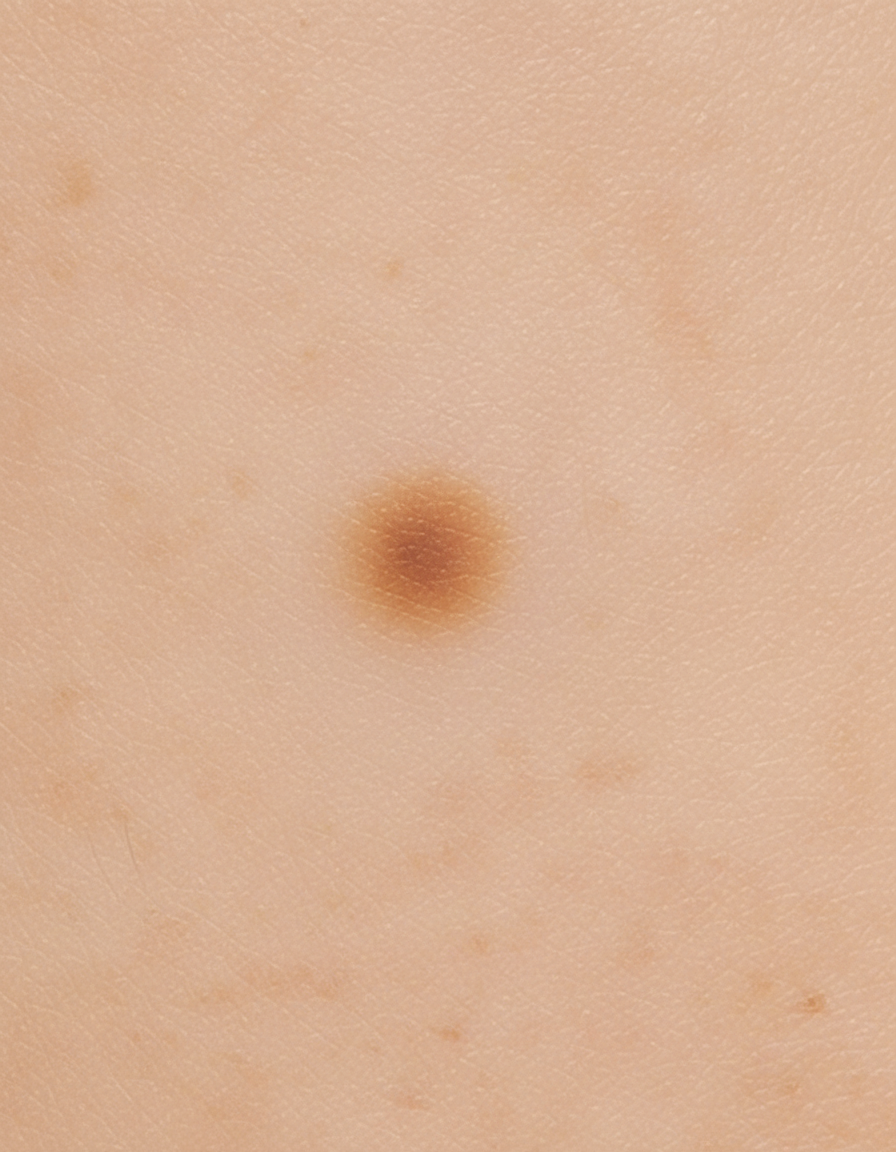
Identify the type of skin lesion shown in the image.
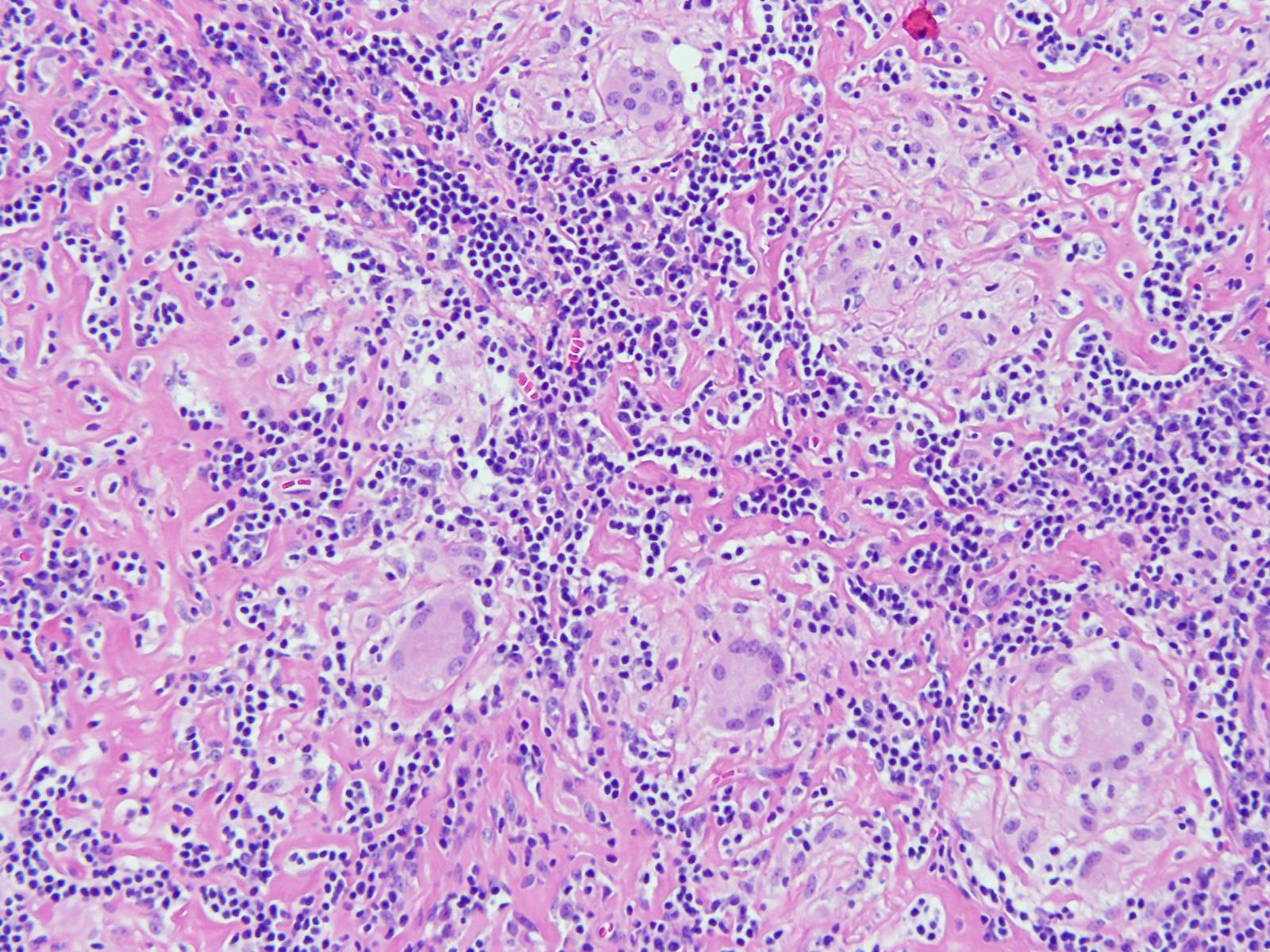
An 11-year-old boy presented with a cough for 15 days. On examination, he was found to have cervical lymphadenopathy. Lymph node biopsy showed the following findings. What could be the diagnosis?
Which of the following is a known risk factor for cholangiocarcinoma?
A 6-year-old boy presents with fever and chills, cough, rapid breathing, difficulty breathing, and chest pain. A culture from a respiratory sample shows Gram-positive bacteria. What is the most likely organism causing this infection?
HBsAg is based on which principle
In which type of lung carcinoma is the p53 mutation most commonly observed?
Identify the condition in the image below?
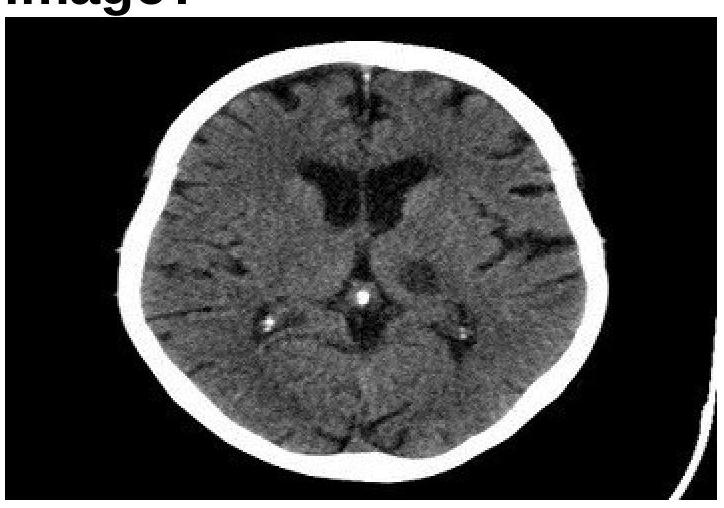
A 40-year-old male with a head injury presents with a GCS of 8, BP of 90/60, and HR of 120. A CT scan shows an epidural hematoma. What are the immediate management priorities?