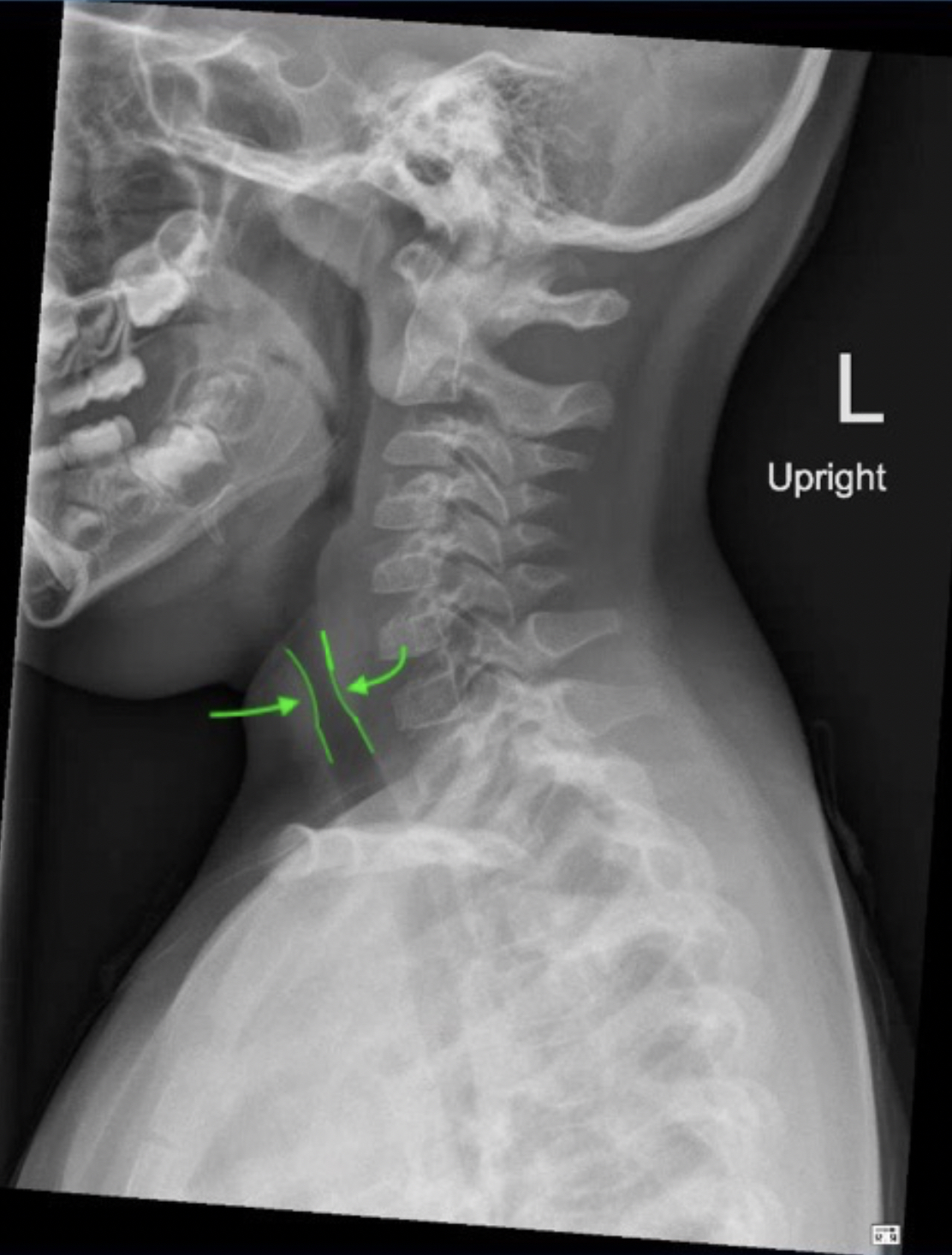
A 4-year-old boy presents with low-grade fever, inspiratory stridor, and barking cough for the past 5 days. Examination reveals a hoarse voice, a moderately inflamed pharynx, and a slightly increased respiratory rate. His chest x-ray showed subglottic narrowing appearing like a steeple. Which among the following is not indicated in the treatment of this condition?