Gastroenterology & Hepatology

On this page
Anatomical Foundations and Disease Burden in Gastroenterology
A 52-year-old man presents with intermittent epigastric burning that worsens after meals and when lying flat. This quintessential presentation of affects approximately 25% of the UK population at some point, making it one of the most common reasons for primary care consultations. Understanding the anatomical basis of gastroenterological conditions-from the oesophagogastric junction to the hepatic lobule-provides the foundation for recognising when functional disorders like cross into organic pathology requiring urgent intervention.
-
Key anatomical landmarks with clinical significance:
- Lower oesophageal sphincter (LES): normally 3-4 cm high-pressure zone; failure allows acid reflux
- Gastric mucosa: parietal cells secrete HCl (pH 1-2); disruption leads to ulceration
- Ileocaecal valve: bacterial load increases from 10³ CFU/mL (small bowel) to 10¹² CFU/mL (colon)
- Portal venous system: drains GI tract at 1000-1200 mL/min; pressure >12 mmHg defines portal hypertension
-
Epidemiological burden requiring memorisation:
- GORD: 25% lifetime prevalence; 10-15% develop Barrett's oesophagus
- IBS: 10-20% UK prevalence; female:male ratio 2:1
- IBD: 620 per 100,000 prevalence; peak onset 15-30 years
- Cirrhosis: 16 per 100,000 mortality; alcohol accounts for 60% of UK cases
📌 Mnemonic for ALARM features: Anaemia, Loss of weight, Anorexia, Recent onset/progressive, Melaena/haematemesis
| Condition | UK Incidence (per 100,000/year) | Key Risk Factor | 5-Year Mortality |
|---|---|---|---|
| GORD | 470 | Obesity (OR 2.5) | <1% (uncomplicated) |
| IBS | 200-300 | Post-infectious | 0% (no excess) |
| Crohn's | 8-10 | Smoking (RR 2.0) | 5-10% |
| Cirrhosis | 15 | Alcohol >50 U/week | 50-70% (decompensated) |
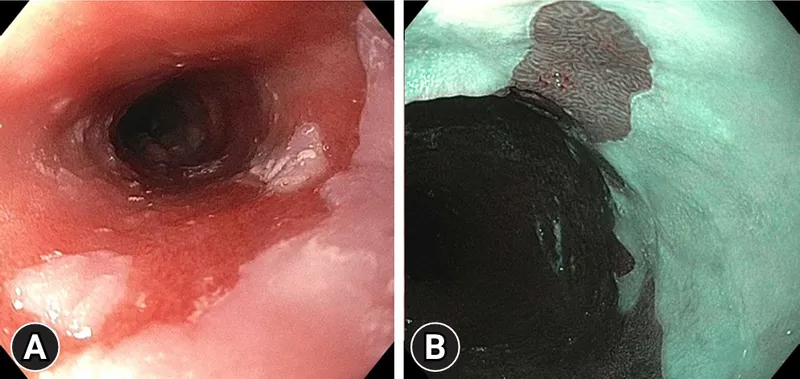
Anatomical Foundations and Disease Burden in Gastroenterology
Pathophysiological Mechanisms Driving GI and Hepatic Disease
The inflammatory cascade in exemplifies how dysregulated immune responses transform physiological inflammation into chronic tissue destruction. In Crohn's disease, impaired NOD2 function disrupts bacterial recognition, triggering excessive Th1/Th17 responses that produce transmural inflammation with non-caseating granulomas. This contrasts with ulcerative colitis, where mucosal-limited Th2 responses cause continuous inflammation from the rectum proximally. Understanding these mechanisms explains why anti-TNF agents work in both conditions but why surgical cure is possible only in UC.
-
Hepatic fibrogenesis in :
- Hepatic stellate cells activated by TGF-β, PDGF, and oxidative stress
- Collagen deposition (types I and III) replaces normal architecture
- Portal hypertension develops when HVPG >10 mmHg (normal 3-5 mmHg)
- Sinusoidal remodelling reduces hepatic blood flow by 30-50%
-
Pancreatic autodigestion in :
- Premature trypsinogen activation within acinar cells (normally occurs in duodenum)
- Trypsin activates elastase, phospholipase A2, and complement cascade
- Capillary leak syndrome develops within 24-48 hours in severe cases
- Calcium sequestration causes hypocalcaemia (<2.0 mmol/L predicts severity)
| Mechanism | Key Mediator | Clinical Consequence | Therapeutic Target |
|---|---|---|---|
| IBD inflammation | TNF-α, IL-12/23 | Transmural ulceration | Infliximab, ustekinumab |
| Portal hypertension | Nitric oxide, endothelin | Varices, ascites | Beta-blockers, TIPS |
| Pancreatic necrosis | Elastase, phospholipase | Retroperitoneal fat necrosis | Supportive only |
Pathophysiological Mechanisms Driving GI and Hepatic Disease
Clinical Presentation and Diagnostic Strategies
A 38-year-old woman with sudden-onset haematemesis and melaena represents , where immediate risk stratification determines survival. The Glasgow-Blatchford Score (GBS) calculated at presentation guides disposition: GBS 0 allows outpatient management (99% safe), while GBS ≥12 predicts need for intervention (>50% requiring endoscopic therapy). Simultaneously, a 45-year-old with chronic epigastric pain and weight loss requires urgent endoscopy to exclude malignancy, as per NICE CG184 guidance for with alarm features.
-
Upper GI bleeding assessment (NICE CG141):
- Immediate full blood count, coagulation, cross-match 2-4 units
- Glasgow-Blatchford Score: Hb, BP, pulse, melaena, syncope, comorbidity
- Rockall Score post-endoscopy predicts rebleeding risk
- Endoscopy within 24 hours for most; immediate if suspected variceal bleed
-
Red flags requiring urgent investigation (<2 weeks):
- Dysphagia at any age (oesophageal cancer until proven otherwise)
- Weight loss >5% in 6 months with GI symptoms
- Persistent vomiting with weight loss
- Age ≥55 years with new-onset dyspepsia lasting >4 weeks
-
Acute pancreatitis diagnosis requires 2 of 3 criteria:
- Characteristic abdominal pain (sudden, severe, epigastric radiating to back)
- Serum amylase or lipase >3× upper limit normal (lipase more specific)
- Imaging findings (CT shows pancreatic oedema, necrosis, fluid collections)
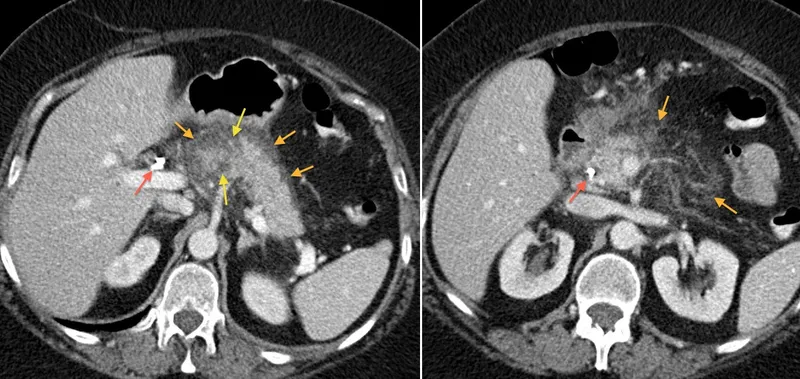
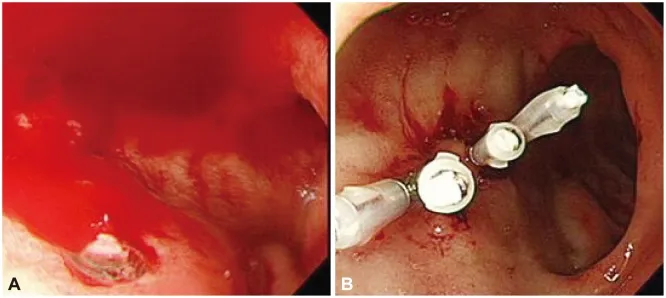
Clinical Presentation and Diagnostic Strategies
Distinguishing Functional from Inflammatory Bowel Disease
The diagnostic challenge separating from hinges on recognising that both cause abdominal pain, diarrhoea, and bloating-yet their management and prognosis differ fundamentally. IBS, affecting 10-20% of the population, represents visceral hypersensitivity and altered motility without structural pathology. Conversely, IBD demonstrates endoscopic ulceration, histological inflammation, and elevated biomarkers. Missing IBD risks delayed treatment and complications; over-investigating IBS drives healthcare costs and patient anxiety.
-
Key discriminating clinical features:
- IBS: Pain relieved by defaecation, symptoms >6 months, normal inflammatory markers
- IBD: Nocturnal diarrhoea, blood in stool, weight loss, raised CRP/ESR
- Faecal calprotectin: <50 μg/g excludes IBD (NPV 99%); >250 μg/g warrants colonoscopy
-
Rome IV criteria for IBS diagnosis (requires all):
- Recurrent abdominal pain ≥1 day/week in last 3 months
- Associated with ≥2 of: related to defaecation, change in stool frequency, change in stool form
- Symptoms onset ≥6 months before diagnosis
⭐ Clinical Pearl: Normal faecal calprotectin in a patient <45 years without alarm features makes IBD extremely unlikely-avoid unnecessary colonoscopy.
| Feature | IBS | IBD (Crohn's/UC) |
|---|---|---|
| Blood PR | Absent (or with constipation only) | Present, mixed with stool |
| Nocturnal symptoms | Rare | Common |
| Weight loss | Absent | Present (>5% body weight) |
| CRP | Normal (<5 mg/L) | Elevated (often >20 mg/L) |
| Faecal calprotectin | <50 μg/g | >250 μg/g |
| Endoscopy | Normal mucosa | Ulceration, friability |
Distinguishing Functional from Inflammatory Bowel Disease
Evidence-Based Management and Escalation Thresholds
Managing follows a treat-to-target strategy, with mucosal healing as the therapeutic endpoint reducing long-term complications by 50%. NICE NG129 recommends starting moderate-to-severe Crohn's with corticosteroids (prednisolone 40 mg daily, taper over 8 weeks) plus azathioprine 2-2.5 mg/kg for maintenance. Failure to achieve remission by 12 weeks mandates biologics: infliximab 5 mg/kg at weeks 0, 2, 6, then 8-weekly. For , endoscopic haemostasis (adrenaline injection plus thermal coagulation) achieves initial control in 90% of cases, but rebleeding occurs in 10-20%-requiring repeat endoscopy or interventional radiology.
-
Variceal bleeding management in :
- Terlipressin 2 mg IV every 4 hours (reduces portal pressure by 25-30%)
- Prophylactic antibiotics: ceftriaxone 1 g IV daily for 7 days (reduces mortality by 30%)
- Endoscopic variceal band ligation within 12 hours
- Transjugular intrahepatic portosystemic shunt (TIPS) if rebleeding despite 2 endoscopies
-
Escalation criteria requiring specialist input:
- IBD: Failure to respond to corticosteroids after 2 weeks (steroid-refractory disease)
- Cirrhosis: Any variceal bleed, ascites, encephalopathy, or jaundice
- Pancreatitis: Persistent organ failure >48 hours, infected necrosis
| Drug | Dose | Monitoring | Key Adverse Effect |
|---|---|---|---|
| Azathioprine | 2-2.5 mg/kg PO daily | FBC, LFTs every 3 months | Myelosuppression (check TPMT) |
| Infliximab | 5 mg/kg IV (0,2,6 weeks then 8-weekly) | Pre-treatment TB screening | Infusion reactions, infection |
| Propranolol | 40-80 mg BD PO | HR target 55-60 bpm | Bronchospasm (avoid in asthma) |
Evidence-Based Management and Escalation Thresholds
Complex Cases and Special Populations
The 68-year-old with compensated cirrhosis and new-onset ascites represents a critical transition point in -median survival drops from 12 years (compensated) to 2 years (first decompensation). Management requires balancing diuresis (spironolactone 100 mg plus furosemide 40 mg daily) against renal impairment, while screening for hepatocellular carcinoma (6-monthly ultrasound and AFP) and varices (endoscopy at diagnosis, then 3-yearly if none found). Pregnancy in IBD demands careful medication review: aminosalicylates and azathioprine are safe, but methotrexate is absolutely contraindicated (major teratogen).
-
Acute pancreatitis severity stratification:
- Modified Glasgow Score ≥3 predicts severe disease (mortality 15-20%)
- CT severity index (Balthazar score) at 72-96 hours guides prognosis
- Infected necrosis (gas on CT, positive aspirate culture) requires necrosectomy
-
Special population considerations:
- Pregnancy: Continue mesalazine, azathioprine; avoid methotrexate, high-dose corticosteroids
- Elderly: Reduce azathioprine dose if eGFR <30; avoid NSAIDs in cirrhosis
- Renal impairment: Adjust mesalazine dose; avoid nephrotoxic drugs in hepatorenal syndrome
| Complication | Presentation | Immediate Management | Prognostic Impact |
|---|---|---|---|
| Infected pancreatic necrosis | Fever, rising CRP after initial improvement | IV meropenem, consider necrosectomy | 30% mortality |
| Hepatorenal syndrome | Rising creatinine, oliguria, no response to fluids | Terlipressin + albumin, consider TIPS | 90% mortality untreated |
| Toxic megacolon | Colon >6 cm, fever, tachycardia | IV hydrocortisone, surgical review | 20% mortality |
Complex Cases and Special Populations
High Yield Summary
Key Take-Aways:
- GORD affects 25% of population; Barrett's oesophagus develops in 10-15%, requiring surveillance endoscopy every 2-5 years
- Faecal calprotectin <50 μg/g excludes IBD with 99% NPV-avoid colonoscopy in young patients with typical IBS and normal calprotectin
- Glasgow-Blatchford Score 0 safely allows discharge in upper GI bleeding; score ≥12 predicts need for intervention
- Portal hypertension defined as HVPG >12 mmHg; variceal bleeding requires terlipressin + antibiotics + band ligation within 12 hours
- Acute pancreatitis requires 2 of 3: characteristic pain, amylase/lipase >3× ULN, imaging findings; Modified Glasgow ≥3 predicts severe disease
Essential Gastroenterology & Hepatology Numbers:
| Parameter | Threshold | Clinical Significance |
|---|---|---|
| Faecal calprotectin | <50 μg/g | Excludes IBD (NPV 99%) |
| Portal pressure (HVPG) | >12 mmHg | Varices develop |
| Amylase/lipase | >3× ULN | Diagnostic for pancreatitis |
| Glasgow-Blatchford Score | 0 | Safe for discharge in UGIB |
| CRP in IBD flare | >20 mg/L | Suggests active inflammation |
Key Principles/Pearls:
- Never discharge a patient with new-onset dysphagia without urgent endoscopy-oesophageal cancer presents late
- In variceal bleeding, prophylactic antibiotics (ceftriaxone) reduce mortality by 30%-always give alongside terlipressin
- IBS is a positive diagnosis using Rome IV criteria, not a diagnosis of exclusion-but always check faecal calprotectin first
- Infected pancreatic necrosis rarely occurs before 7-10 days-early fever suggests another source
Quick Reference:
| Condition | First-Line Investigation | First-Line Treatment | Escalation Trigger |
|---|---|---|---|
| GORD | PPI trial 4-8 weeks | Lansoprazole 30mg daily | Alarm features, failed PPI trial |
| UGIB | Glasgow-Blatchford Score, endoscopy | Resuscitation, endoscopic therapy | Rebleeding after 2 endoscopies |
| IBS | Faecal calprotectin | Dietary modification, antispasmodics | Alarm features, abnormal calprotectin |
| IBD | Colonoscopy + biopsy | Corticosteroids ± azathioprine | Steroid-refractory at 2 weeks |
| Cirrhosis | Ultrasound + AFP 6-monthly | Treat underlying cause, varices screening | Any decompensation event |
| Acute pancreatitis | Amylase/lipase, CT at 72-96h | Fluid resuscitation, analgesia | Modified Glasgow ≥3, organ failure |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app










