🚧 Pathophysiology - Bile Duct Blockade
- A progressive, idiopathic, fibro-obliterative process that destroys the extrahepatic (and often intrahepatic) bile ducts during early infancy.
- The exact cause is unknown, but potential triggers include perinatal viral infections (Reovirus, CMV), an abnormal immune response, or genetic predisposition.
- Obstruction of bile flow leads to cholestasis, causing direct hepatocyte injury from retained toxic bile acids.
- This triggers a cascade of inflammation, progressive fibrosis, and ultimately, biliary cirrhosis and end-stage liver disease if untreated.
⭐ The process is time-sensitive. Fibrosis progresses rapidly, making the liver unsuitable for a Kasai portoenterostomy if diagnosis is delayed past 90-120 days of life.
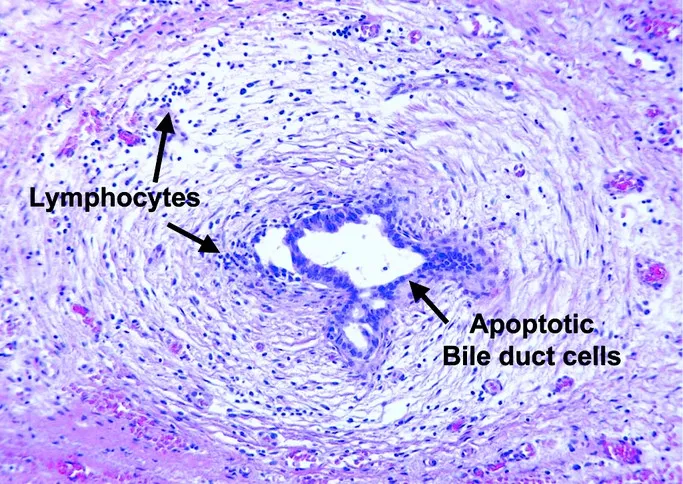
👶 Jaundice That Lingers
Presents in a previously healthy-appearing infant, typically between 2-8 weeks of age.
- Persistent Jaundice: The cardinal sign. Jaundice develops or persists beyond the typical 2-3 weeks of physiologic jaundice.
- Stool & Urine Changes:
- Acholic Stools: Progressively pale, clay-colored stools due to biliary obstruction.
- Dark Urine: Tea-colored from renal excretion of conjugated bilirubin.
- Lab Hallmark: Conjugated (direct) hyperbilirubinemia (Direct Bili >1 mg/dL or >20% of total).
- Physical Exam: Firm, progressive hepatomegaly.

⭐ Critical Pearl: Infants often appear well and gain weight initially, which can falsely reassure caregivers and delay the crucial diagnosis past the optimal window for the Kasai procedure.
🔬 Diagnosis - Catching the Culprit
-
Initial Labs:
- ↑ Direct (conjugated) bilirubin is the hallmark.
- ↑ Gamma-glutamyl transpeptidase ($GGT$) is highly characteristic.
- ↑ AST/ALT.
-
Imaging Pathway:
- 1st Line (Ultrasound): Screens for other causes. May show absent/small gallbladder or the "triangular cord sign" (fibrous remnant of extrahepatic duct).
- 2nd Line (HIDA Scan): Hepatobiliary scintigraphy. After 5 days of phenobarbital pre-treatment to stimulate bile flow, shows hepatic uptake but no excretion of tracer into the small bowel.
- Gold Standard (Intraoperative Cholangiogram): Definitive diagnosis. Dye is injected directly into the gallbladder/biliary tree during surgery, confirming blockage before proceeding with Kasai.
⭐ Failure of radiotracer to appear in the intestine on a HIDA scan, even after phenobarbital stimulation, is the most reliable non-invasive finding pointing to biliary atresia over other causes of neonatal cholestasis.
🔪 The Kasai Fix: Hepatoportoenterostomy
-
Procedure: A hepatoportoenterostomy (Roux-en-Y anastomosis).
- The fibrotic, atretic extrahepatic biliary tree is excised.
- A loop of jejunum is anastomosed to the liver capsule at the porta hepatis.
- This allows bile to drain directly from microscopic intrahepatic ductules into the small intestine.
-
Timing is Critical:
- Best outcomes if performed before 60 days of age.
- Success rates decline sharply after 90 days due to irreversible cirrhosis.
⭐ The Kasai procedure is palliative, not curative. It aims to restore bile flow to delay the need for liver transplantation. Many patients ultimately require a transplant.
- Post-op Management:
- Prophylactic antibiotics (e.g., trimethoprim-sulfamethoxazole) to prevent ascending cholangitis.
- Supplementation: Fat-soluble vitamins (A, D, E, K) and medium-chain triglycerides (MCTs).
⚡ Biggest Takeaways
- Presents in neonates (2-8 weeks) with jaundice, dark urine, and pale/acholic stools.
- Key lab finding is conjugated (direct) hyperbilirubinemia.
- Pathophysiology: Progressive inflammatory obliteration of extrahepatic bile ducts.
- Gold standard diagnosis is intraoperative cholangiogram.
- Treatment is the Kasai procedure (hepatoportoenterostomy), best performed <60 days of age.
- Despite surgery, most patients develop cholangitis and eventually need a liver transplant.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

