Thyroid Hormone Synthesis - The Iodine Job
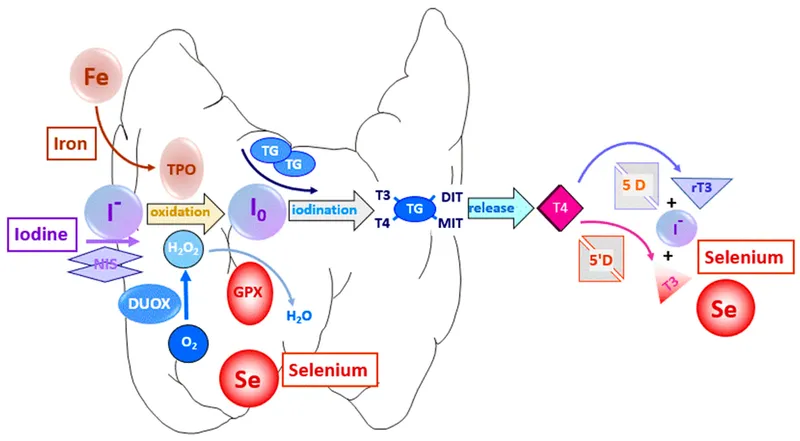
- Iodide Trapping: Dietary iodide is actively transported into follicular cells via the Na+/I- symporter (NIS).
- Key Enzyme: Thyroid peroxidase (TPO) on the apical membrane manages:
- Oxidation: Iodide (I⁻) to iodine (I₂).
- Organification: Iodine added to thyroglobulin (TG) to form MIT & DIT.
- Coupling: MIT + DIT → T₃; DIT + DIT → T₄.
⭐ Wolff-Chaikoff Effect: Excess iodide temporarily inhibits TPO, ↓ hormone synthesis. This is a protective autoregulatory effect. "Escape" from this effect occurs via downregulation of the NIS.
- Drug Targets:
- Perchlorate, Thiocyanate: Inhibit NIS.
- Propylthiouracil (PTU), Methimazole: Inhibit TPO.
Bloodstream Convoy - The Great Carrier Heist
- Transport: >99% of T3/T4 is protein-bound in blood; only free hormone is active.
- Thyroxine-Binding Globulin (TBG): Binds most T4 & T3. Levels ↑ in pregnancy (estrogen), ↓ in liver failure, nephrotic syndrome.
- Other carriers: Albumin, Transthyretin.
- Action:
- T4 is a prohormone, converted to T3 (more potent) in peripheral tissues by 5'-deiodinase.
- T3 acts via nuclear receptors to regulate gene transcription.
⭐ High-Yield: Drugs like salicylates and phenytoin can displace thyroid hormone from TBG, transiently increasing free hormone levels.
Peripheral Action - T4's Big Makeover
- Prohormone to Active Form: Thyroxine ($T_4$) is the main circulating hormone, but Triiodothyronine ($T_3$) is 3-4x more potent. $T_4$ functions as a prohormone, converted to $T_3$ in target tissues.
- Key Enzyme: Deiodinase:
- 5'-deiodinase (Types I & II) converts $T_4 \rightarrow T_3$ (activation). Found in liver, kidney, brain, pituitary.
- 5-deiodinase (Type III) converts $T_4 \rightarrow$ reverse $T_3$ ($rT_3$, inactive) and $T_3 \rightarrow T_2$ (inactivation).
- Cellular Action:
- $T_3$ enters the cell and binds to high-affinity nuclear receptors (TRα, TRβ).
- This hormone-receptor complex acts as a transcription factor, binding to Thyroid Response Elements (TREs) on DNA to alter gene expression and metabolic rate.
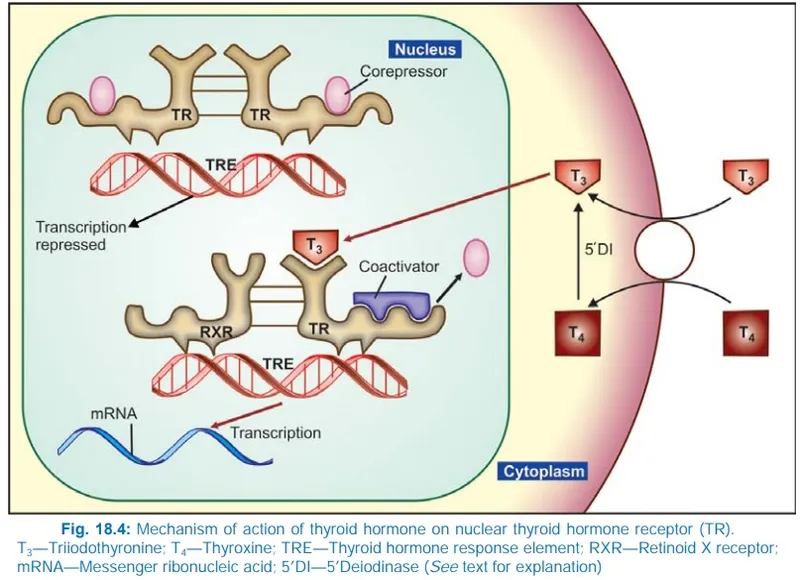
⭐ High-Yield Fact: Drugs like propylthiouracil (PTU), propranolol, amiodarone, and corticosteroids can ↓ the peripheral conversion of $T_4$ to $T_3$. This is a key mechanism for rapidly controlling symptoms in thyroid storm.
HPT Axis - The Control Tower
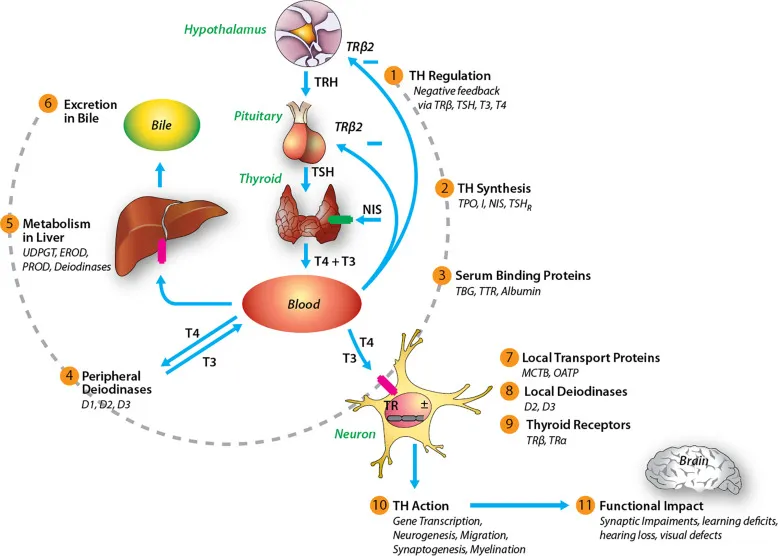
- Hypothalamus: Releases Thyrotropin-Releasing Hormone (TRH) in a pulsatile fashion.
- Anterior Pituitary: TRH stimulates thyrotrophs to release Thyroid-Stimulating Hormone (TSH).
- Thyroid Gland: TSH acts on follicular cells (via Gs pathway) to synthesize and release T4 and T3.
- Negative Feedback: Free T3/T4 inhibit TRH and TSH secretion, maintaining hormonal balance.
⭐ Inhibition: TSH release is also inhibited by somatostatin, dopamine, and high levels of glucocorticoids. This is a key regulatory point outside of direct thyroid feedback.
High‑Yield Points - ⚡ Biggest Takeaways
- Most thyroid hormone circulates bound to thyroxine-binding globulin (TBG); only the free hormone is active.
- Peripheral conversion of T4 to T3 by 5'-deiodinase is a key activation step; T3 is more potent.
- Thyroid hormones act via intracellular nuclear receptors, directly influencing gene transcription and protein synthesis.
- They are critical for regulating basal metabolic rate (BMR) and CNS maturation.
- They upregulate β-adrenergic receptors, increasing sensitivity to catecholamines.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

