Insulin Synthesis - The Body's Sugar Boss
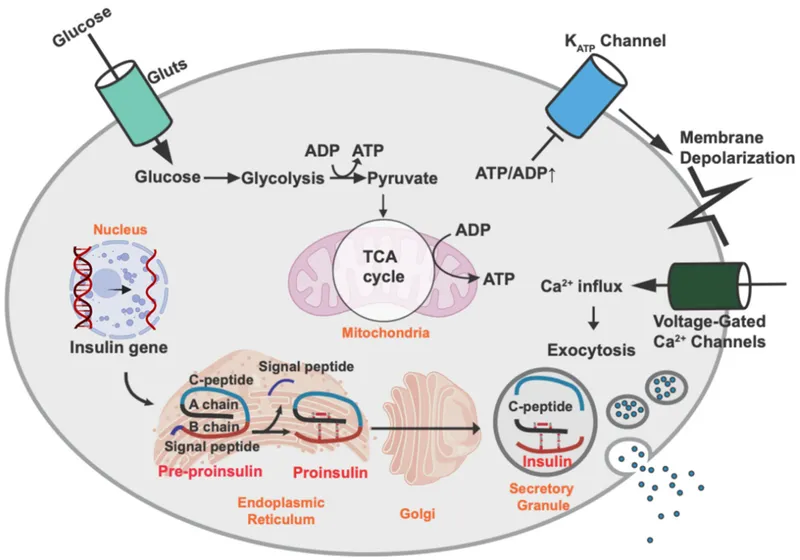
- Origin: Synthesized in pancreatic β-cells, encoded by the INS gene on chromosome 11.
- Process: Follows the secretory pathway from preproinsulin (RER) to proinsulin (Golgi), finally cleaved into active insulin and C-peptide.
- Storage: Held in secretory granules with zinc, awaiting a glucose signal for release.
⭐ C-peptide is the most accurate measure of endogenous insulin production. It has a longer half-life (
30 min) than insulin (5 min), making it a more stable clinical marker.
Insulin Kinetics - The Insulin Lineup
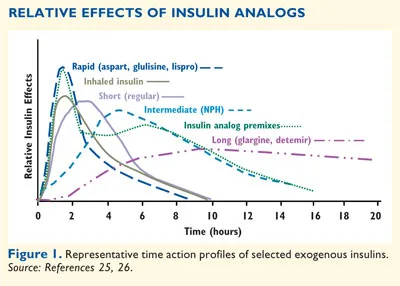
- Rapid-Acting: Lispro, Aspart, Glulisine. 📌 Mnemonic: No LAG.
- Onset: 15 min
- Peak: 1-2 hr
- Duration: 3-5 hr
- Short-Acting: Regular (Humulin R, Novolin R).
- Onset: 30-60 min
- Peak: 2-4 hr
- Duration: 6-8 hr
- Intermediate-Acting: NPH (Humulin N, Novolin N).
- Onset: 1-2 hr
- Peak: 4-12 hr
- Duration: 12-18 hr
- Long-Acting: Detemir, Glargine, Degludec.
- Onset: 1-2 hr
- Peak: Flat (no true peak)
- Duration: >24 hr (Glargine, Degludec), 16-24 hr (Detemir)
⭐ IV regular insulin is standard for hyperglycemic emergencies like DKA, while rapid-acting (Lispro/Aspart) can also be used IV.
Clinical Use & Complications - The Balancing Act
-
Therapeutic Uses:
- Type 1 & advanced Type 2 DM
- Gestational Diabetes
- DKA/HHS emergencies
- Hyperkalemia (with glucose to prevent hypoglycemia)
-
Major Complications:
- Hypoglycemia: Most common/dangerous.
- Autonomic symptoms (tachycardia, sweating) precede neuroglycopenic ones (confusion, coma).
- Treat: Glucose (oral/IV), glucagon (IM).
- Weight Gain: Due to anabolic effects.
- Lipodystrophy: Atrophy/hypertrophy at injection sites; prevented by site rotation.
- Hypokalemia: Especially with IV insulin; drives K⁺ into cells.
- Hypoglycemia: Most common/dangerous.
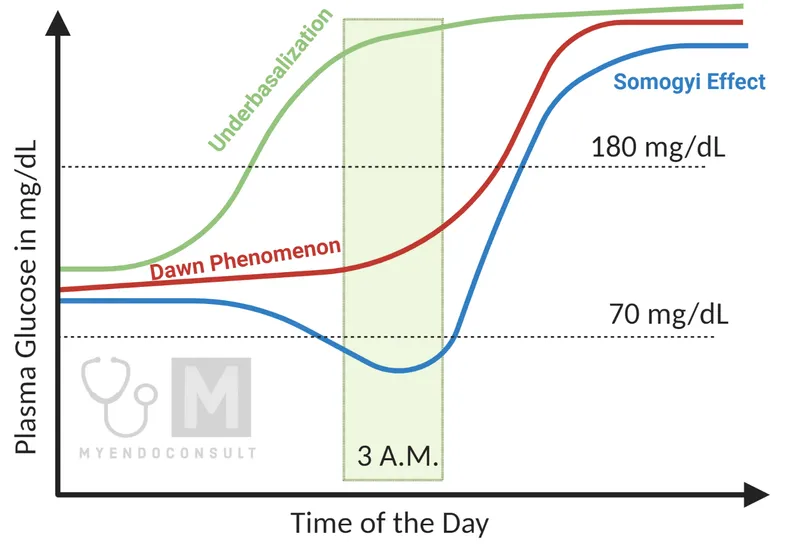
⭐ Exam Favorite: Differentiating morning hyperglycemia. Check glucose at 3 AM.
- Somogyi Effect: Low 3 AM glucose. Caused by nocturnal hypoglycemia → counter-regulatory surge. Fix: Decrease evening insulin.
- Dawn Phenomenon: Normal/High 3 AM glucose. Caused by morning cortisol/GH surge. Fix: Increase evening insulin.
High‑Yield Points - ⚡ Biggest Takeaways
- Rapid-acting insulins (Lispro, Aspart, Glulisine) are crucial for postprandial glucose control.
- Regular insulin is the only preparation for IV use, making it essential in Diabetic Ketoacidosis (DKA).
- NPH, an intermediate-acting insulin, has a cloudy appearance and exhibits more variable absorption.
- Long-acting, peakless insulins (Glargine, Detemir, Degludec) provide basal glycemic control.
- The most common and dangerous adverse effect across all insulin types is hypoglycemia.
- When mixing, always draw up clear (Regular/Rapid) before cloudy (NPH).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

