Mechanism of Inotropy - The Heart's Power-Up
- Primary Driver: ↑ intracellular Calcium ($Ca^{2+}$) is the final common pathway for inotropy.
- Key Pathway: Sympathetic stimulation of β1 receptors activates the cAMP-PKA pathway.
- PKA phosphorylates L-type $Ca^{2+}$ channels → ↑ $Ca^{2+}$ influx.
- PKA also enhances sarcoplasmic reticulum (SR) $Ca^{2+}$ release.
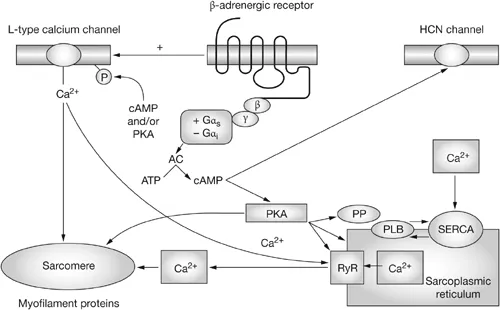
⭐ Digoxin's Unique Mechanism: Unlike sympathomimetics, Digoxin inhibits the Na⁺/K⁺-ATPase pump. This leads to ↑ intracellular Na⁺, which then reduces Ca²⁺ efflux via the Na⁺/Ca²⁺ exchanger, ultimately increasing intracellular $Ca^{2+}$ and contractility.
Cardiac Glycosides - Digoxin's Digital Grip
- Mechanism: Directly inhibits the Na⁺/K⁺ ATPase pump in myocardial cells.
- This increases intracellular Na⁺, reversing the Na⁺/Ca²⁺ exchanger.
- Result: ↑ intracellular Ca²⁺ → ↑ contractility (positive inotropy).
- Also stimulates the vagus nerve → ↓ AV nodal conduction & ↓ heart rate.
-
Clinical Use:
- Heart Failure (HFrEF): For symptomatic control; no survival benefit.
- Atrial Fibrillation: Rate control by slowing AV conduction.
-
Toxicity & Adverse Effects (Narrow Therapeutic Index):
- Cardiac: Any arrhythmia, classically scooped "hockey-stick" ST segments on ECG.
- GI/CNS: Nausea, vomiting, confusion, xanthopsia (yellow vision).
- Antidote: Digoxin immune Fab.
⭐ Hypokalemia is a key precipitant of digoxin toxicity because it reduces competition for binding sites on the Na⁺/K⁺ ATPase.
Beta-Adrenergic Agonists - The Beta Boosters
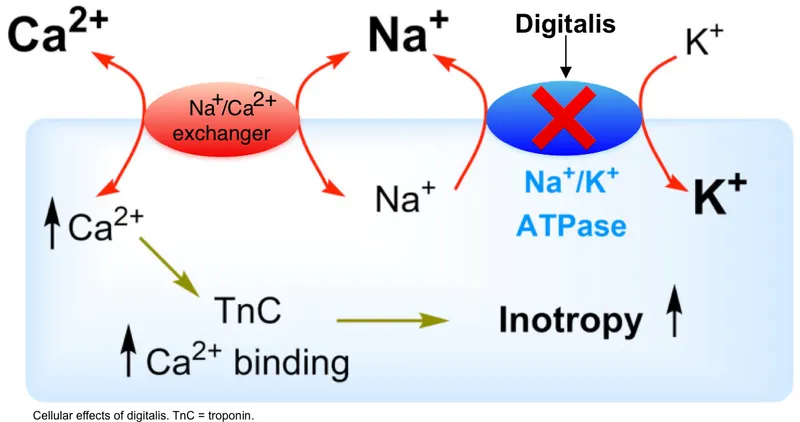
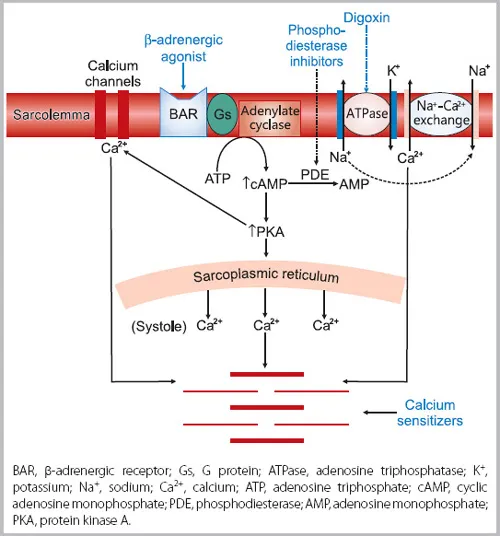
- Mechanism: Stimulate β-receptors → ↑ adenylyl cyclase → ↑ cAMP → ↑ intracellular Ca²⁺ → ↑ myocardial contractility & heart rate.
- Agents & Actions:
- Dobutamine: Primarily β₁ agonist. ↑ Contractility >> ↑ Heart Rate. Used in acute decompensated heart failure & cardiogenic shock.
- Dopamine: Dose-dependent effects.
- Low: D₁ receptors → Renal vasodilation.
- Med: β₁ receptors → ↑ Contractility, ↑ HR.
- High: α₁ receptors → Vasoconstriction.
- Isoproterenol: Non-selective β₁/β₂ agonist. ↑ HR & contractility, but potent vasodilation (↓ SVR).
- Adverse Effects: Tachyarrhythmias, angina, headache.
⭐ In cardiogenic shock, dobutamine is a primary choice. However, if the patient is severely hypotensive (e.g., SBP < 70 mmHg), dopamine or norepinephrine are preferred for their potent vasoconstrictor effects.
PDE-3 Inhibitors - cAMP's Lifeguards
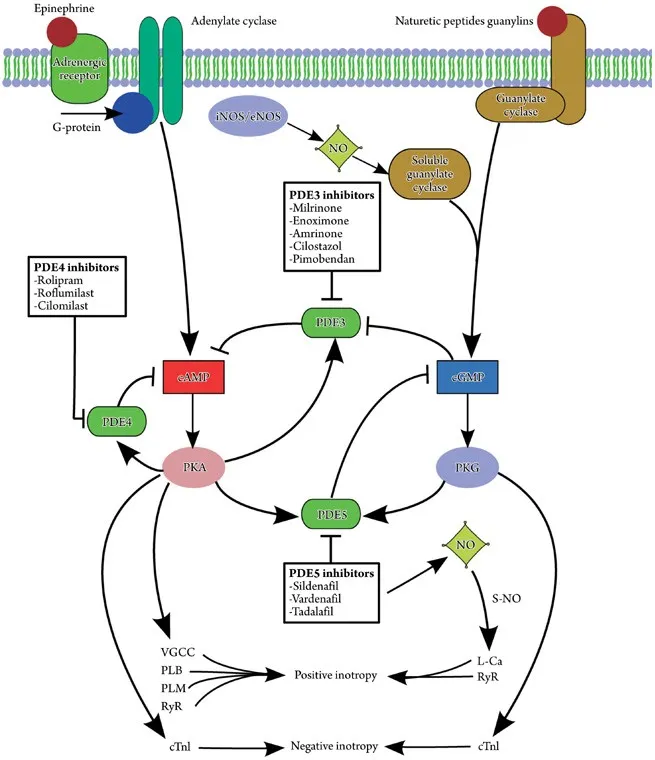
- Drugs: Milrinone, Inamrinone.
- Mechanism: Selective PDE-3 inhibition prevents cAMP breakdown in cardiac and vascular smooth muscle.
- Heart: ↑ cAMP → PKA activation → ↑ Ca²⁺ influx → ↑ contractility (inotropy) & heart rate.
- Vessels: ↑ cAMP → smooth muscle relaxation → significant vasodilation (↓ preload & afterload).
- Use: Short-term management of acute decompensated heart failure.
- Adverse Effects: Ventricular arrhythmias, hypotension, thrombocytopenia.
⭐ Reserved for severe, refractory heart failure as long-term use is associated with increased mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Digoxin inhibits the Na+/K+ ATPase, increasing intracellular Ca2+ and contractility; toxicity presents with xanthopsia and hyperkalemia.
- Beta-agonists (Dobutamine) and PDE-3 inhibitors (Milrinone) increase cAMP, boosting contractility in acute heart failure.
- Both are used for acute decompensated HF but increase myocardial O2 demand and risk of arrhythmias.
- The final common pathway for inotropy is elevated intracellular calcium.
- Treat digoxin toxicity with DigiFab (antibody fragments).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

