Mechanisms & Hemodynamics - Pipe-Opening Principles
- Primary Action: Directly relax arteriolar smooth muscle, leading to vasodilation.
- Hemodynamic Effect: Marked ↓ in Systemic Vascular Resistance (SVR) and afterload.
- Minimal effect on venous capacitance; preload is largely unaffected.
- Compensatory Response: Baroreceptor-mediated stimulation of the sympathetic nervous system.
- Results in reflex tachycardia, ↑ contractility, and ↑ renin release.
⭐ Exam Favorite: The profound reflex sympathetic activation often necessitates co-administration with a beta-blocker to manage the resulting tachycardia and increased myocardial oxygen demand.
Arterial Vasodilators - The 'Artery-Only' Agents
-
Hydralazine
- Mechanism: ↑ cGMP → smooth muscle relaxation. Primarily dilates arterioles, reducing afterload.
- Metabolism: Acetylation in the liver. Status (slow vs. fast acetylator) affects drug levels and risk of toxicity.
- Use: Severe HTN, hypertensive emergencies (incl. pregnancy), co-administered with nitrates for heart failure.
- Adverse Effects: Reflex tachycardia, fluid retention/edema, headache, angina. Drug-induced lupus-like syndrome.
-
Minoxidil
- Mechanism: Opens ATP-sensitive K+ channels ($K_{ATP}$) in vascular smooth muscle → hyperpolarization & relaxation.
- Use: Severe, treatment-refractory hypertension.
- Adverse Effects: More potent than hydralazine. Causes significant reflex tachycardia and fluid retention. 📌 Hypertrichosis (hirsutism) - exploited for topical use (Rogaine) in alopecia.
⭐ High-Yield: Hydralazine-induced lupus is more common in patients who are slow acetylators and is associated with anti-histone antibodies.
Mixed Vasodilators - The Emergency Responders
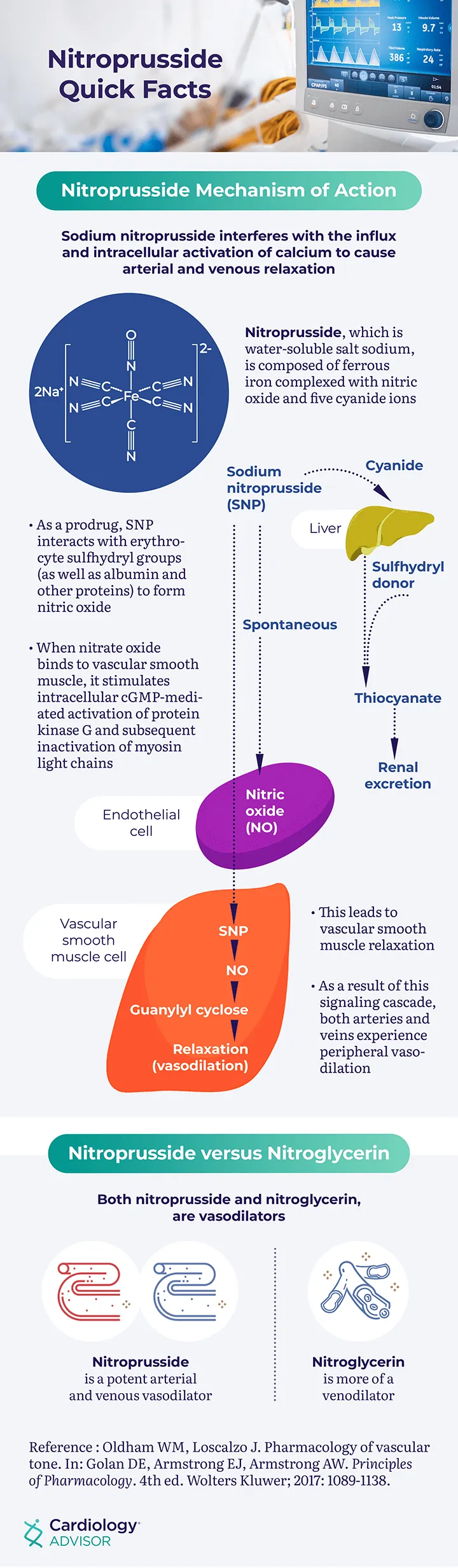
- Sodium Nitroprusside
- MOA: Directly releases Nitric Oxide (NO) → ↑ cGMP → potent vasodilation of both arterioles and venules.
- Hemodynamic Effects: ↓↓ Preload (venous pooling) & ↓↓ Afterload (reduced SVR).
- Maintains stroke volume; ↑ heart rate (reflex tachycardia).
- Use: Hypertensive emergencies (e.g., malignant hypertension, aortic dissection). Administered via continuous IV infusion.
- Metabolism & Toxicity:
- Metabolized to cyanide and NO.
- ⚠️ Cyanide Toxicity: Risk ↑ with renal impairment or prolonged (>24-48 hrs) / high-dose infusions. Presents with altered mental status, seizures, lactic acidosis.
- Antidotes: Sodium thiosulfate (provides sulfur groups), hydroxocobalamin (binds cyanide), sodium nitrite (induces methemoglobinemia).
- 📌 Mnemonic: NitroPrusside → NO Provider.
⭐ Exam Favorite: Nitroprusside can cause coronary steal syndrome by dilating coronary arterioles, potentially shunting blood away from ischemic areas.
High‑Yield Points - ⚡ Biggest Takeaways
- Hydralazine and Minoxidil are primarily arteriolar vasodilators, causing a significant decrease in afterload.
- The profound drop in blood pressure triggers reflex tachycardia and fluid retention, necessitating co-administration with β-blockers and diuretics.
- Remember drug-induced lupus for Hydralazine and hypertrichosis for Minoxidil.
- Sodium nitroprusside dilates both arteries and veins for hypertensive emergencies but carries a risk of cyanide toxicity.
- Fenoldopam, a D1 agonist, uniquely increases renal blood flow, making it ideal for hypertensive crises with renal insufficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

