Mechanism of Action - Cellular Sabotage
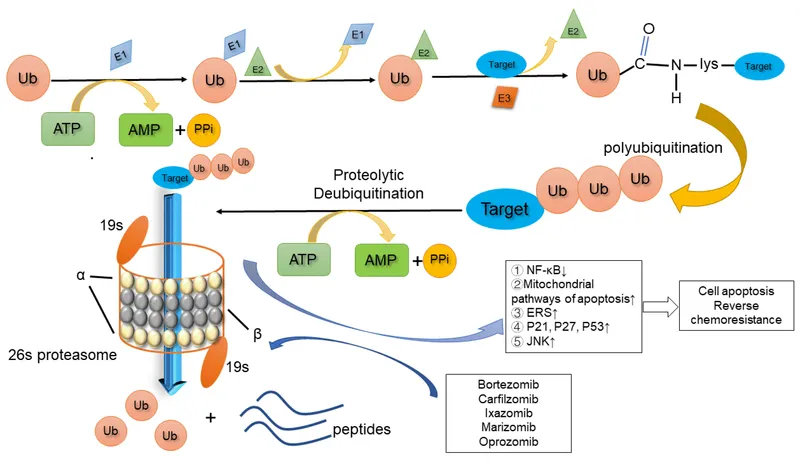
- Proteasome inhibitors (e.g., Bortezomib) reversibly block the 26S proteasome, preventing the breakdown of ubiquitinated proteins.
- This disruption leads to the accumulation of regulatory proteins, triggering programmed cell death (apoptosis).
- Key Consequence: Prevents degradation of IκB.
- Accumulated IκB sequesters and inhibits NF-κB, a key pro-survival transcription factor.
- This blockade halts the transcription of genes that promote cell growth and survival.
⭐ In multiple myeloma, cells are highly dependent on NF-κB signaling. Inhibiting the proteasome is thus a highly effective therapeutic strategy.
The 'Zomibs' - Key Proteasome Players
-
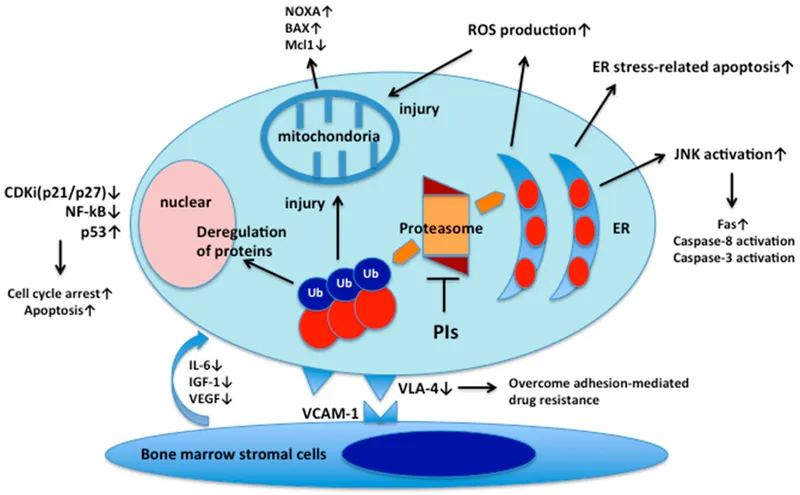
Mechanism: Inhibit the 26S proteasome, a key cellular machine for protein degradation. This disrupts cell cycle regulation and promotes apoptosis by preventing the breakdown of pro-apoptotic proteins.
- Leads to accumulation of ubiquitinated proteins, causing proteotoxic stress.
- In multiple myeloma, it crucially inhibits NF-κB by stabilizing its inhibitor, IκB.
-
Indications: Multiple Myeloma, Mantle Cell Lymphoma.
-
Agents & Key Features:
- Bortezomib: The first-in-class, reversible inhibitor. Administered IV or SC.
- Carfilzomib: An irreversible inhibitor. Often used in relapsed/refractory cases.
- Ixazomib: The first oral proteasome inhibitor, offering convenience.
- Toxicity Profile:
- Peripheral Neuropathy: Most common with Bortezomib.
- Thrombocytopenia: Common across the class.
- Cardiotoxicity: A notable risk with Carfilzomib.
⭐ High-Yield: Patients on proteasome inhibitors are at an increased risk for Herpes Zoster reactivation. Prophylactic antiviral therapy (e.g., acyclovir) is standard of care.
Adverse Effects - The Downside of Disruption
- Peripheral Neuropathy: A major dose-limiting toxicity, especially with bortezomib. Presents as a painful sensory neuropathy. Less frequent with second-generation agents like carfilzomib.
- Myelosuppression: Primarily cyclical thrombocytopenia. Platelet counts nadir around day 11 and typically recover before the next cycle. Anemia and neutropenia also occur.
- Cardiotoxicity: Can manifest as or worsen heart failure, particularly with carfilzomib. Requires baseline and ongoing cardiac monitoring.
- Constitutional & GI: Fatigue, pyrexia, nausea, and diarrhea are common.
⭐ A key distinguishing adverse effect is the risk of Herpes Zoster (shingles) reactivation due to suppression of VZV-specific T-cells. Prophylactic antiviral therapy (e.g., acyclovir) is standard practice.
High‑Yield Points - ⚡ Biggest Takeaways
- Proteasome inhibitors (e.g., Bortezomib) block the 26S proteasome, causing accumulation of ubiquitinated intracellular proteins.
- This buildup of toxic proteins triggers apoptosis and cell cycle arrest, proving particularly effective against malignant plasma cells.
- The primary clinical use is for Multiple Myeloma.
- Key toxicities include painful peripheral neuropathy and thrombocytopenia.
- Prophylaxis for herpes zoster reactivation is essential due to immunosuppression.
- Identify this class by the "-zomib" suffix.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

