Self-Tolerance - Friend or Foe?
-
Definition: The immune system's ability to distinguish self from non-self, preventing attacks on its own tissues. Failure leads to autoimmunity.
-
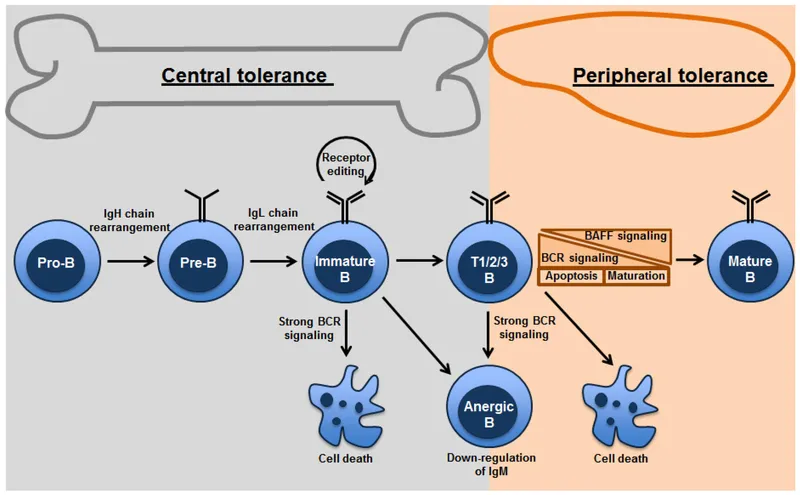
Central Tolerance: Occurs in primary lymphoid organs.
- T-Cells (Thymus): Negative selection eliminates self-reactive T-cells. The AIRE gene is crucial for expressing tissue-specific antigens.
- B-Cells (Bone Marrow): Receptor editing or apoptosis of self-reactive B-cells.
-
Peripheral Tolerance: A backup system for escaped self-reactive lymphocytes.
- Anergy: Functional inactivation without cell death.
- Suppression: By regulatory T-cells (Tregs) expressing FOXP3.
- Activation-Induced Cell Death (AICD): Fas-FasL pathway.
⭐ Mutations in the AIRE gene cause Autoimmune Polyendocrinopathy-Candidiasis-Ectodermal Dystrophy (APECED), also known as APS-1.

Tolerance Breakdown - The System Glitches
-
Central Tolerance Failure: Defective negative selection in primary lymphoid organs.
- AIRE gene mutations → Autoimmune Polyendocrinopathy-Candidiasis-Ectodermal Dystrophy (APECED).
-
Peripheral Tolerance Failure: Mature lymphocytes misbehave in secondary tissues.
- T-Regulatory Cell Defects: FOXP3 mutations → IPEX syndrome (Immune dysregulation, Polyendocrinopathy, Enteropathy, X-linked).
- Molecular Mimicry: Foreign antigen resembles self-antigen. E.g., Rheumatic fever post-Strep infection.
- Epitope Spreading: Immune response broadens from initial to other self-antigens.
- Cryptic Antigens: Self-antigens, previously hidden, are exposed by tissue damage or inflammation.
⭐ HLA Association: Many autoimmune diseases are linked to specific HLA subtypes, like HLA-B27 with ankylosing spondylitis.
Damage Mechanisms - Friendly Fire Frenzy
-
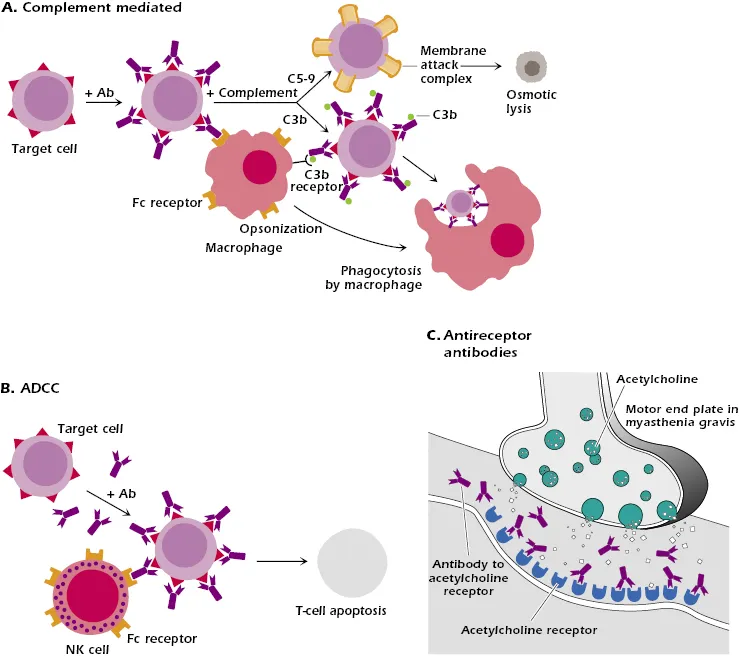
Type II: Antibody-Mediated (Cytotoxic)
- IgG/IgM bind to self-antigens on cell surfaces or in the extracellular matrix.
- Triggers destruction via:
- Opsonization: Coating for phagocytosis.
- Complement Activation: Leads to MAC formation & cell lysis.
- ADCC: NK cells kill antibody-coated targets.
-
Type III: Immune Complex-Mediated
- Antigen-antibody complexes form and deposit in tissues (e.g., vessels, kidneys, joints).
- Activates complement (C3a, C5a), attracting neutrophils that release damaging enzymes.
-
Type IV: T-Cell-Mediated
- CD4+ T-cells: Secrete cytokines (e.g., IFN-γ) that activate macrophages, leading to chronic inflammation and tissue injury.
- CD8+ T-cells: Directly kill host cells expressing self-antigens.
⭐ Receptor-Blocking/Stimulating Antibodies: A key Type II variant where antibodies don't cause cell death but alter function. E.g., anti-AChR in Myasthenia Gravis (blocks) or anti-TSHR in Graves' disease (stimulates).
High-Yield Points - ⚡ Biggest Takeaways
- Autoimmunity represents a loss of self-tolerance, leading the immune system to attack host tissues.
- Genetic susceptibility is strongly linked to specific HLA subtypes (e.g., HLA-B27, HLA-DR3/DR4).
- Environmental factors, like infections or UV light, often trigger disease in predisposed individuals.
- Key mechanisms include molecular mimicry, where microbial antigens resemble self-antigens.
- Failure of peripheral tolerance, involving dysfunctional T-regulatory (Treg) cells, is a central defect.
- Tissue damage is mediated by Type II, III, and IV hypersensitivity reactions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

