Initial Prenatal Visit - The Grand Welcome
- Comprehensive History & Physical:
- History: Detailed medical, surgical, OB/GYN (GPs), and genetic history.
- Physical Exam: Baseline weight, BMI, blood pressure, and a full pelvic exam including a Pap test if due.
- Dating the Pregnancy:
- Based on Last Menstrual Period (LMP).
- 1st-trimester ultrasound is the most accurate method; Crown-Rump Length (CRL) measurement is key. Supersedes LMP if discrepancy is >7 days.
- Initial Lab Workup (Prenatal Panel):
- Blood Tests: CBC, Blood type, Rh(D) status & antibody screen, RPR (syphilis), HBsAg (Hep B), HIV screen.
- Immunity Status: Rubella and Varicella titers.
- Infection Screen: Urine culture, Gonorrhea & Chlamydia NAAT.
⭐ A fetal heart rate is typically first detectable by Doppler ultrasound around 10-12 weeks of gestation.
First Trimester - Foundation & Formation
- Frequency: Every 4 weeks.
- Aneuploidy Screening (11-14 weeks):
-
- Combined Test: Serum PAPP-A & β-hCG + Nuchal Translucency (NT) ultrasound.
-
- NIPT/cffDNA: Non-invasive prenatal testing using cell-free fetal DNA; high sensitivity/specificity, especially for high-risk patients.
-
- Diagnostic Testing (Confirmatory):
-
- Chorionic Villus Sampling (CVS): Performed at 10-13 weeks if screening is positive or for high-risk cases.
-
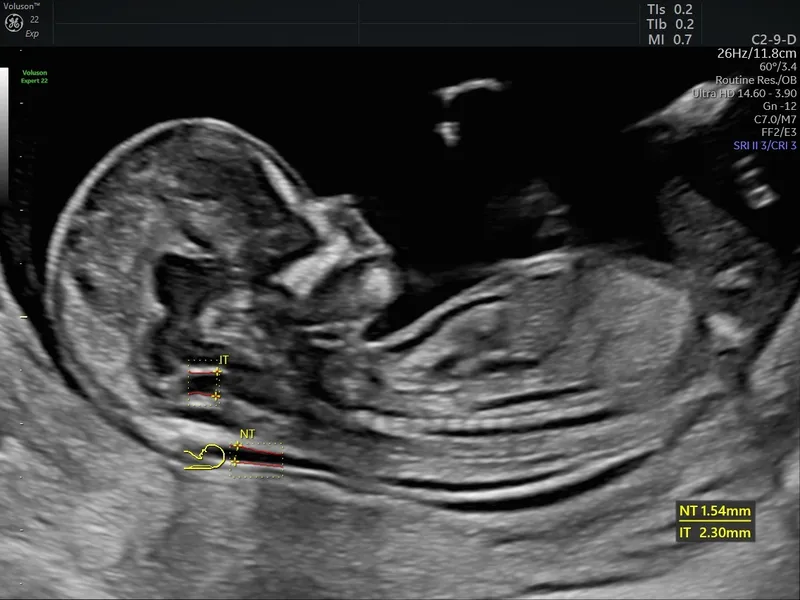
⭐ Nuchal translucency (NT) is a key marker; an increased NT measurement is associated with a higher risk for aneuploidies like Trisomy 21.
Second Trimester - Anatomy & Sweetness
- Visits: Every 4 weeks until 28 weeks.
- Assessments: Monitor fetal heart tones & measure fundal height (pubic symphysis to uterine fundus).
- Key Screenings & Diagnostics:
- 15-20 wks: Quad Screen (AFP, hCG, Estriol, Inhibin A).
- 15-20 wks: Amniocentesis for genetic diagnosis if indicated.
- 18-22 wks: Detailed anatomy ultrasound.
- 24-28 wks: Gestational Diabetes (GDM) screen with 50g, 1-hr glucose challenge test.
⭐ Quad Screen Pattern: In Down Syndrome (Trisomy 21), expect ↓ AFP, ↓ Estriol, but ↑ hCG and ↑ Inhibin A.
Third Trimester - The Final Countdown
- Visit Frequency: Every 2 weeks from 28-36 weeks, then weekly from 36 weeks until delivery.
- Key Assessments & Screenings:
- 28 weeks: Administer Rho(D) immune globulin if Rh-negative. Repeat CBC for anemia.
- 36-38 weeks: Group B Strep (GBS) rectovaginal culture.
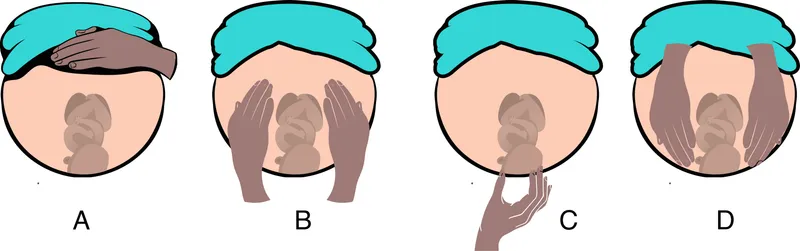
- Assess fetal position and presentation via Leopold maneuvers.
- Consider repeat HIV/RPR for high-risk patients.
⭐ Intrapartum penicillin is indicated for GBS-positive status, unknown GBS status with risk factors (e.g., fever, prolonged rupture of membranes), or a history of an infant with invasive GBS disease.
High-Yield Points - ⚡ Biggest Takeaways
- Visit Frequency: Every 4 weeks until 28 weeks, every 2 weeks until 36 weeks, then weekly until delivery.
- Initial Labs: Type & Rh, CBC, RPR, HIV, HBsAg, rubella immunity, GC/Chlamydia.
- 24-28 Weeks: Screen for gestational diabetes (1-hr GCT); give Rho(D) immune globulin to Rh-negative patients.
- 36-38 Weeks: Perform Group B Strep (GBS) rectovaginal culture.
- Every Visit: Assess fetal heart tones and measure fundal height (after 20 weeks).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

