Principles of Vaccination - The Body's Boot Camp
- Active Immunity: Body produces its own antibodies after exposure to an antigen (infection or vaccine).
- Leads to long-lasting memory (B & T cells).
- Types: Natural (infection), Artificial (vaccination).
- Passive Immunity: Pre-formed antibodies are transferred to a recipient.
- Provides rapid, temporary protection; no memory produced.
- Types: Natural (maternal IgG via placenta, IgA in breast milk), Artificial (monoclonal antibodies).
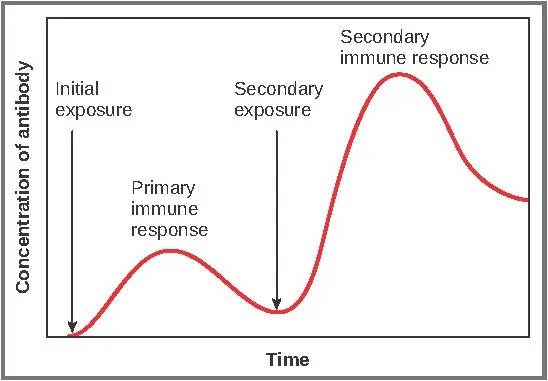
⭐ High-Yield: Maternal IgG wanes by ~6 months. This is why most infant primary vaccine series begin at 2 months, balancing protection with avoiding maternal antibody interference.
- Herd Immunity: Protects unvaccinated individuals when a high percentage of the population is vaccinated (threshold varies by R₀).
Types of Vaccines - The Immunity Arsenal
-
Live Attenuated: Weakened pathogen; mimics natural infection.
- Immunity: Strong, lifelong cell-mediated & humoral response.
- Risks: ⚠️ Contraindicated in pregnancy & immunodeficiency.
- Examples: MMR, Varicella, Rotavirus, Sabin polio, Yellow fever.
- 📌 Rome Is My Best Place To Visit (Rotavirus, Influenza-intranasal, MMR, BCG, Polio-Sabin, Typhoid-oral, Varicella)
-
Inactivated (Killed): Whole, killed pathogen.
- Immunity: Mainly humoral antibody response. Requires boosters.
- Examples: Hepatitis A, Influenza (shot), Polio (Salk), Rabies. (📌 RIP Always)
-
Subunit, Recombinant, Polysaccharide, & Conjugate: Uses only antigenic fragments.
- Recombinant: Hepatitis B, HPV.
- Polysaccharide: Pneumococcal (PPSV23). T-cell independent response.
- Conjugate: Polysaccharide + protein carrier. Elicits a high-affinity, T-cell dependent response. Hib, Pneumococcal (PCV13).
-
Toxoid: Inactivated toxin.
- Examples: Tetanus, Diphtheria.
-
mRNA / Viral Vector:
- mRNA: COVID-19 (Pfizer, Moderna).
- Viral Vector: COVID-19 (J&J), Ebola.
⭐ Conjugate vaccines (e.g., PCV13, Hib) are critical for infants <2 years old because they convert the polysaccharide's T-cell-independent response into a robust T-cell-dependent response, inducing immunologic memory.
Schedules & Safety - Rules of Engagement
- All vaccines can be co-administered in separate sites (≥1 inch apart).
- Inactivated vaccines do not require a minimum interval between different types.
- Live Attenuated Vaccines (LAVs):
- If not given on the same day, must be spaced ≥4 weeks apart. 📌 LIVE for 4 weeks!
- LAVs can cause a false-negative PPD. Administer PPD on the same day or wait 4-6 weeks after the LAV.
- Increasing the interval between multi-dose vaccine series does not reduce efficacy; decreasing it may interfere with the immune response.
⭐ Anaphylactic egg allergy is no longer a contraindication for most influenza vaccines. MMR is safe as it's grown on fibroblast cells.
- Active immunity from vaccines creates long-lasting memory B and T cells, while passive immunity offers immediate but temporary protection.
- Live attenuated vaccines (e.g., MMR, varicella) induce a robust cellular and humoral response but are risky in immunocompromised individuals.
- Killed/inactivated vaccines (e.g., Salk polio, Hepatitis A) are safer, primarily inducing a humoral response, and often require boosters.
- Conjugate vaccines (e.g., Hib, PCV13) link a polysaccharide to a protein to improve the T-cell response in young children.
- Herd immunity protects vulnerable, unvaccinated individuals by reducing pathogen transmission within a community.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

