AKI Fundamentals - The Kidney Crisis
- Definition: Abrupt kidney dysfunction causing ↑ creatinine & ↓ urine output.
- ↑ SCr by ≥0.3 mg/dL within 48h
- ↑ SCr to ≥1.5x baseline
- Urine output <0.5 mL/kg/h for >6 hours
- Types:
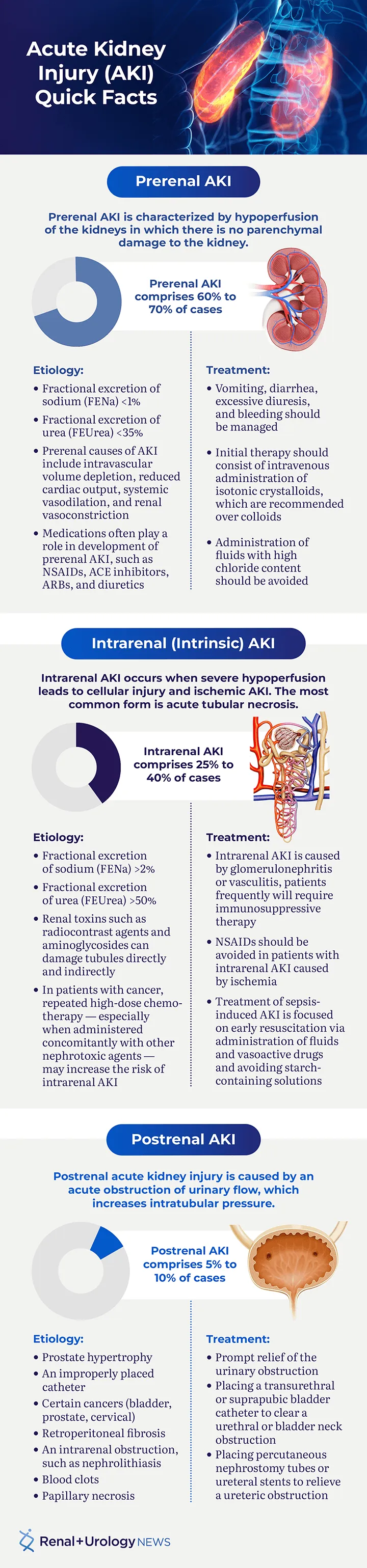
- Prerenal: Hypoperfusion (e.g., dehydration). BUN/Cr >20, $FeNa$ <1%.
- Intrinsic: Direct kidney damage (e.g., ATN, AIN).
- Postrenal: Urinary tract obstruction (e.g., BPH, stones).
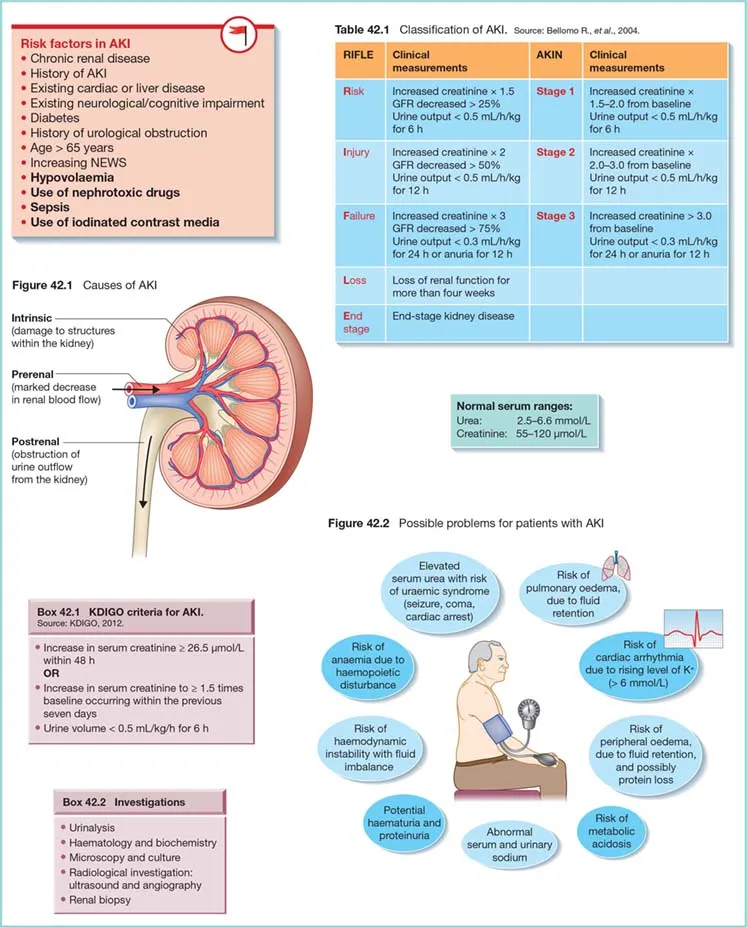
⭐ Fractional excretion of sodium ($FeNa$) is a key test to differentiate prerenal AKI from ATN, but its utility is limited in patients on diuretics.
Prerenal AKI - The Dry Spell
- Pathophysiology: ↓ Renal perfusion triggers physiologic Na⁺/H₂O retention. It is typically reversible with restored blood flow.
- Etiologies:
- True volume loss (e.g., hemorrhage, dehydration).
- ↓ Effective circulating volume (e.g., heart failure, cirrhosis).
- Renal artery stenosis.
- Drugs: NSAIDs, ACE inhibitors, ARBs.
- Key Labs:
- BUN/Cr Ratio > 20:1
- Urine Osmolality > 500 mOsm/kg
- FENa < 1%
- Urine Na⁺ < 20 mEq/L
⭐ The hallmark is a BUN/Cr ratio > 20:1, reflecting increased passive urea reabsorption in the proximal tubule due to enhanced sodium and water reabsorption.
Intrinsic AKI - Muddy Waters
- Direct damage to kidney structures (tubules, interstitium, glomeruli). Characterized by FENa > 2% and Urine Osm < 350 mOsm/kg.
Acute Tubular Necrosis (ATN)
- Most common cause.
- Ischemic: Prolonged hypotension/hypoxia (e.g., shock, sepsis).
- Nephrotoxic: Aminoglycosides, contrast dye, myoglobin, ethylene glycol.
- Urinalysis: Muddy brown granular casts are pathognomonic.
Acute Interstitial Nephritis (AIN)
- Inflammatory infiltrate in the interstitium, often drug-induced.
- Classic Triad: Fever, rash, arthralgias.
- Urinalysis: WBC casts, sterile pyuria, and eosinophiluria.
⭐ Muddy brown casts in ATN are composed of necrotic tubular epithelial cells and Tamm-Horsfall protein.

Postrenal AKI - The Block Party
- Pathophysiology: Urinary tract obstruction → ↑ intratubular pressure → ↓ GFR.
- Etiologies: Benign Prostatic Hyperplasia (BPH) is the most common cause. Others include nephrolithiasis, tumors (prostate, cervical), and neurogenic bladder.
- Diagnosis:
- Bladder ultrasound is the initial test to look for hydronephrosis.
- Catheterization can be both diagnostic and therapeutic.
- Labs: Early phase shows BUN:Cr > 15:1.
⭐ Unilateral obstruction does not cause AKI unless the patient has only one functioning kidney.
AKI Management - Dialysis Decisions
Indications for urgent dialysis (📌 AEIOU):
- Acidosis: Severe, refractory metabolic acidosis (pH < 7.1)
- Electrolytes: Severe, refractory hyperkalemia (K⁺ > 6.5 mEq/L)
- Intoxication: Specific poisons (e.g., salicylates, lithium, methanol, ethylene glycol)
- Overload: Refractory fluid overload causing pulmonary edema
- Uremia: Symptomatic (encephalopathy, seizures, or pericarditis)
⭐ Uremic pericarditis is an absolute indication for immediate dialysis.
High‑Yield Points - ⚡ Biggest Takeaways
- Prerenal AKI, the most common type, shows a BUN/Cr ratio > 20:1 and FeNa < 1%, often from hypovolemia.
- Acute Tubular Necrosis (ATN), the top intrinsic cause, presents with muddy brown granular casts and an FeNa > 2%.
- Postrenal AKI results from obstruction; diagnose with a renal ultrasound looking for hydronephrosis.
- Cardiorenal and hepatorenal syndromes are critical diagnoses in advanced heart failure and cirrhosis, respectively.
- Always review medications for nephrotoxins like NSAIDs and contrast dye, especially in high-risk settings.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

