🔭 Scoping It Out
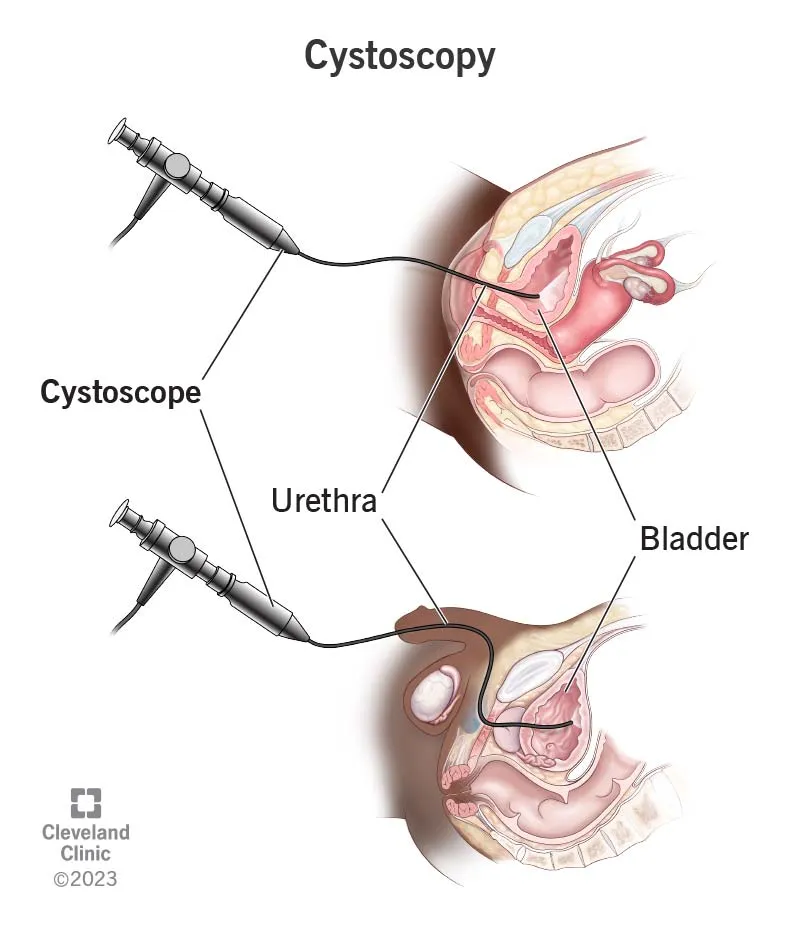
- Cystourethroscopy: Direct endoscopic visualization of the urethra, prostatic urethra (males), ureteric orifices, and bladder.
- Key Indications:
- Diagnostic: Gross/microscopic hematuria, recurrent UTIs, bladder cancer surveillance, voiding symptoms.
- Therapeutic: Biopsy, tumor resection (TURBT), stone removal, stent placement/removal.
- Common Complications: Transient hematuria, dysuria, UTI, urinary retention (esp. with BPH).
Scope Selection:
| Feature | Flexible Cystoscopy | Rigid Cystoscopy |
|---|---|---|
| Setting | Outpatient, office-based | Operating Room (OR) |
| Anesthesia | Local (lidocaine jelly) | General or spinal |
| Primary Use | Diagnostic | Therapeutic |
| Channel Size | Smaller | Larger (for instruments) |
🧐 Clinical Manifestations - The 'Why' We Peek
Key indication is evaluating the source of bleeding or obstruction.
-
Diagnostic & Surveillance
- Bladder Cancer: Initial diagnosis (biopsy) and routine surveillance for recurrence.
- Recurrent UTIs: Evaluate for anatomical causes (stones, diverticula, fistulas).
- Obstructive/Irritative LUTS: Investigate unclear etiology (stricture, BPH complications).
-
Therapeutic Interventions
- Stent Management: Placement or removal of ureteral stents.
- Stone Removal: Crushing and removing bladder stones (cystolitholapaxy).
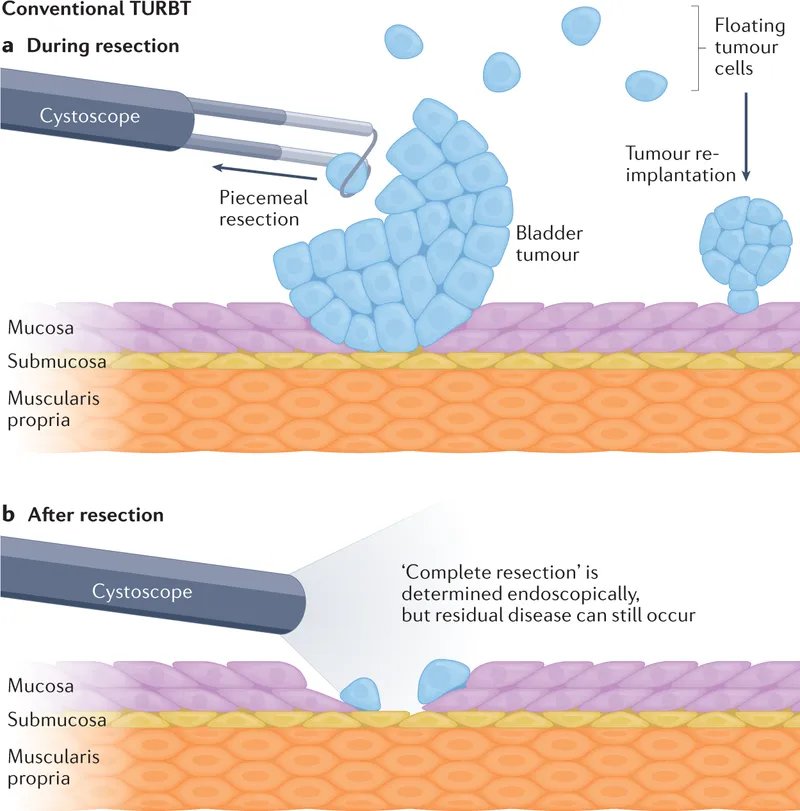
- Tumor Resection: Transurethral Resection of Bladder Tumor (TURBT).
⭐ Painless gross hematuria is bladder cancer until proven otherwise, mandating urgent urologic evaluation.
🗺️ Anatomy - Navigating the Waterworks
A cystoscope follows a specific anatomical path. The male urethra is longer and more complex.
- Male: Longer (~20 cm), S-shaped course. Key landmarks for navigation:
- Verumontanum: A crucial mound in the prostatic urethra where ejaculatory ducts open.
- External Sphincter: Located at the membranous urethra; vital for urinary continence.
- Female: Short (~4 cm) and straight path, making instrumentation easier but increasing UTI risk.
⭐ The verumontanum is the most critical landmark to orient within the prostatic urethra. The external sphincter lies just distal to its apex, a "no-go" zone to prevent incontinence during TURP.
⚠️ Complications - When Scopes Go Rogue
- Infection (UTI/Urosepsis): Most common. Presents with fever, dysuria, urgency. Risk ↑ with pre-existing bacteriuria or obstruction. Prophylactic antibiotics for high-risk patients.
- Bleeding (Hematuria): Typically mild and self-resolving. Persistent or gross hematuria may require catheterization and continuous bladder irrigation (CBI).
- Trauma & Perforation:
- Urethral Stricture: A late complication from instrumentation trauma.
- Bladder Perforation: Rare but serious. Acute abdominal pain, inability to void. Requires urgent surgical repair.
- Urinary Retention: Due to edema, clots, or anesthesia effects.
⭐ Post-cystoscopy fever with rigors and hypotension is a red flag for urosepsis. Obtain cultures and start empiric IV antibiotics immediately before imaging!
⚡ Biggest Takeaways
- Gold standard for evaluating gross hematuria and for bladder cancer surveillance.
- Provides direct visualization of the urethra and bladder to find tumors, stones, and strictures.
- Enables diagnostic biopsies of suspicious lesions and therapeutic interventions like stent placement.
- Flexible cystoscopy is a well-tolerated outpatient procedure; rigid cystoscopy is for OR-based interventions.
- Most common complication is post-procedure UTI. Hematuria and dysuria are also frequent.
- Acute UTI is a major contraindication due to the risk of iatrogenic urosepsis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

