👶 Little Bodies, Big Differences
- Higher Body Surface Area (BSA) to Weight Ratio: ↑ insensible water losses.
- Higher Metabolic Rate: ↑ fluid turnover and oxygen demand.
- Immature Kidneys:
- Lower Glomerular Filtration Rate (GFR).
- Poor urine concentrating ability; can't conserve water efficiently.
- Limited Glycogen Stores: High risk for hypoglycemia with fasting/stress.
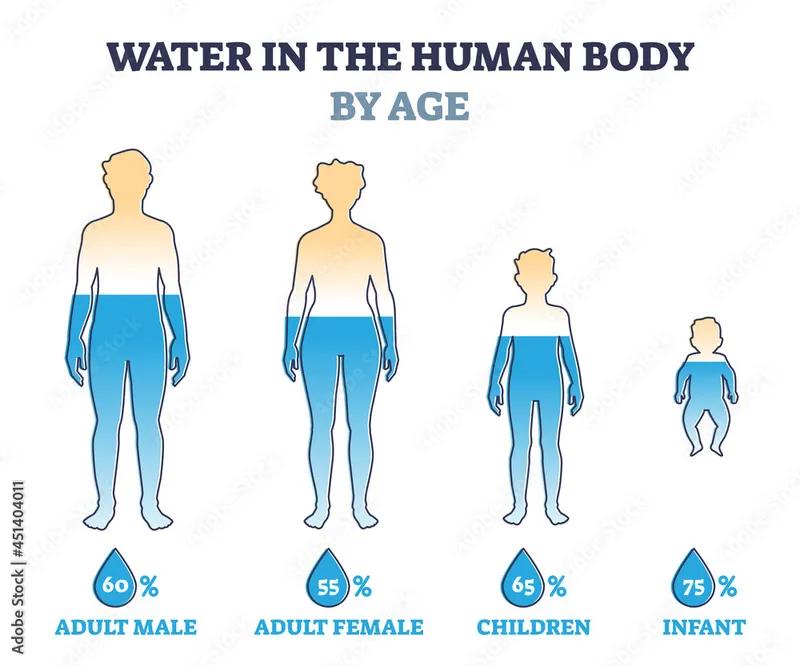
- Body Composition: Higher % of Total Body Water (TBW), especially extracellular fluid (ECF).
⭐ Infants' larger ECF volume (as a % of TBW) means they lose a greater proportion of their total fluid with vomiting or diarrhea, leading to rapid dehydration.
💧 Management - The Fluid Formula
The Holliday-Segar method calculates daily maintenance fluid needs based on weight.
- First 10 kg: $100 \text{ mL/kg/day}$
- Next 10 kg (11-20 kg): $50 \text{ mL/kg/day}$
- Each kg > 20 kg: $20 \text{ mL/kg/day}$
📌 "4-2-1 Rule" for Hourly Rate:
- First 10 kg: $4 \text{ mL/kg/hr}$
- Next 10 kg: $2 \text{ mL/kg/hr}$
- Each kg > 20 kg: $1 \text{ mL/kg/hr}$
⭐ Isotonic fluids (e.g., D5 NS, LR) are now preferred over hypotonic fluids for maintenance in most hospitalized children to reduce the risk of iatrogenic hyponatremia from non-osmotic ADH secretion.
🔧 Management - Fixing the Deficit
-
1. Calculate Fluid Deficit (mL):
- $ \text{Deficit} = % \text{Dehydration} \times \text{Weight (kg)} \times \mathbf{10} $
- e.g., 10% dehydrated 10 kg child = 1000 mL deficit.
-
2. Initial Resuscitation (if needed):
- For moderate-severe dehydration/shock.
- Bolus: 20 mL/kg isotonic crystalloid (NS/LR) over 15-30 min.
- May repeat 2-3 times.
-
3. Plan Deficit Replacement:
- Subtract bolus from total deficit.
- Replace remaining deficit + maintenance fluids over 24-48 hrs.
- 📌 Common plan: 50% of deficit in first 8 hrs, remaining 50% over next 16 hrs.
⭐ Slow is Safe for Sodium!
- Hyponatremia: Correct Na⁺ ≤ 8-12 mEq/L per 24h (prevents ODS).
- Hypernatremia: Correct Na⁺ ≤ 0.5 mEq/L/hr (prevents cerebral edema).
🎢 Pathophysiology - Electrolyte Rollercoaster
- Sodium ($Na^+$):
- Hyponatremia (<135 mEq/L): Often post-op (↑ADH) or from hypotonic fluids. Risk of cerebral edema, seizures.
- Hypernatremia (>145 mEq/L): Dehydration (diarrhea, fever). Risk of intracranial hemorrhage during rehydration.
- Potassium ($K^+$):
- Hypokalemia (<3.5 mEq/L): GI losses (NG suction, vomiting). Causes ileus, ECG changes (U waves).
- Hyperkalemia (>5.5 mEq/L): Renal failure, cell lysis. ECG changes (peaked T waves).
⭐ The most common electrolyte abnormality in hospitalized children is iatrogenic hyponatremia due to hypotonic fluid administration, leading to seizures.
⚡ Biggest Takeaways
- Calculate maintenance fluids with the 4-2-1 rule: 4 mL/kg/hr (first 10 kg), 2 (next 10), 1 (rest).
- Use isotonic fluids (D5 NS/LR) for maintenance to prevent iatrogenic hyponatremia, especially post-op (↑ADH).
- Resuscitate with rapid 20 mL/kg boluses of isotonic crystalloid (NS or LR) for shock.
- Tachycardia is the earliest sign of dehydration; also check for sunken fontanelles and poor turgor.
- Add dextrose to maintenance fluids to prevent hypoglycemia in infants with low glycogen stores.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

