🧠 Pathophysiology - No Nerves, No Go
- Core Defect: Congenital aganglionosis of the distal GI tract, primarily the colon.
- Mechanism: Arrest of craniocaudal migration of neural crest cells during weeks 5-12 of gestation.
- Result: Absence of ganglion cells in the submucosal (Meissner's) and myenteric (Auerbach's) plexuses.
- Genetics: Strongly associated with loss-of-function mutations in the RET proto-oncogene.
- Location: Always affects the rectum and extends proximally for a variable distance.
⭐ The aganglionic segment cannot relax, remaining tonically contracted. This causes a functional obstruction, leading to proximal bowel dilation.
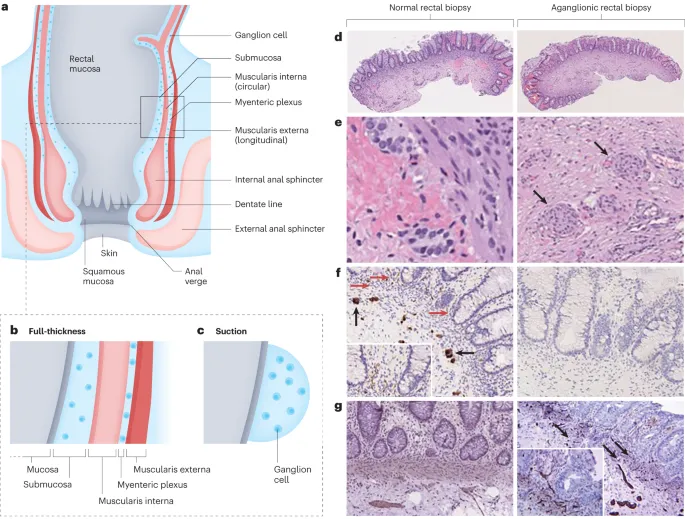
🔍 Diagnosis - Spotting the Stuck Spot
Clinical Red Flags in Newborns:
- Failure to pass meconium within 48 hours.
- Bilious emesis.
- Progressive abdominal distension.
- 💡 "Squirt sign": Explosive release of stool/gas on digital rectal exam (DRE) is highly suggestive.
Diagnostic Pathway:
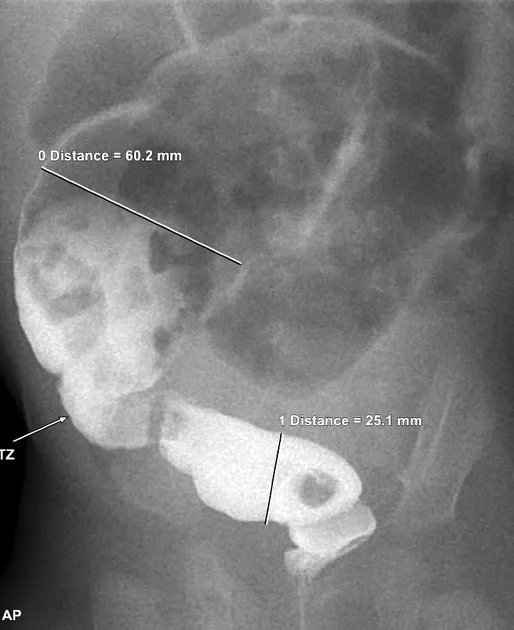
- Contrast Enema: Key initial test. Visualizes a narrow distal segment (aganglionic) and a dilated proximal colon (normally innervated), defining the "transition zone."
- Anorectal Manometry: Useful screening test. Shows failure of internal anal sphincter relaxation upon rectal balloon distension (absent RAIR).
- Rectal Suction Biopsy (Gold Standard): Definitive diagnosis. Histology shows an absence of ganglion cells in the submucosal plexus.
⭐ A full-thickness biopsy is required to assess for ganglion cells in both the submucosal (Meissner) and myenteric (Auerbach) plexuses.
✂️ Management - The Great Pull-Through
The management of Hirschsprung disease is a two-stage process: initial stabilization followed by definitive surgical correction.
- Initial Stabilization (Pre-operative)
- Goal: Decompress the obstructed proximal bowel, prevent Hirschsprung-Associated Enterocolitis (HAEC) and perforation.
- Key interventions:
- NPO (Nil Per Os)
- IV fluids for hydration and electrolyte correction.
- NG decompression to relieve proximal distention.
- Serial rectal irrigations with saline to evacuate stool.
⭐ The primary goal of initial management is to decompress the obstructed proximal bowel to prevent perforation and prepare for definitive surgery.
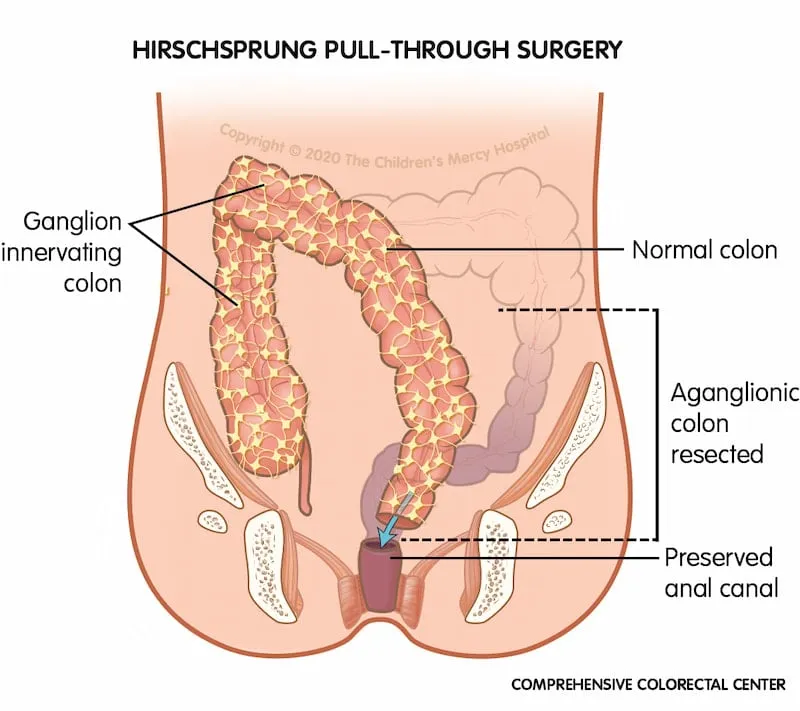
- Definitive Treatment: The Pull-Through
- Surgical resection of the aganglionic segment.
- The normal, ganglionic bowel is then "pulled through" and anastomosed to the anus.
- Commonly performed procedures:
- Swenson: Original full-thickness resection.
- Soave: Endorectal pull-through (leaves a muscular cuff).
- Duhamel: Retrorectal pull-through.
⚠️ Post-Op Perils
-
Hirschsprung-Associated Enterocolitis (HAEC): The most common and life-threatening complication, occurring pre- or post-operatively. Presents as a toxic megacolon-like state.
⭐ HAEC manifests with fever, explosive foul-smelling diarrhea, and abdominal distension. Management is urgent: NPO, IV fluids, broad-spectrum antibiotics, and decompressive rectal irrigations.
-
Anastomotic Complications:
- Leak: Early post-op; presents with fever, abdominal pain, and signs of peritonitis.
- Stricture: Late post-op; causes recurrent constipation and obstructive symptoms.
-
Chronic Dysmotility:
- Persistent constipation
- Fecal incontinence/soiling
⚡ Biggest Takeaways
- Gold standard diagnosis: Rectal suction biopsy showing absent ganglion cells in the submucosal plexus.
- Contrast enema is the best initial imaging test, revealing a transition zone.
- Initial management: Bowel decompression (NG tube, rectal irrigation) and fluid resuscitation.
- Definitive treatment: Surgical resection of the aganglionic segment via a pull-through procedure.
- Most feared complication: Hirschsprung-associated enterocolitis (HAEC), which can be fatal.
- Strongly associated with Down syndrome and MEN 2A/2B.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

