🎗️ Core Concept - Saving the Breast
- Breast Conservation Therapy (BCT) combines lumpectomy (wide local excision) with adjuvant radiation therapy.
- Goal: Achieve oncologic outcomes equivalent to mastectomy while preserving the breast.
- Key Components:
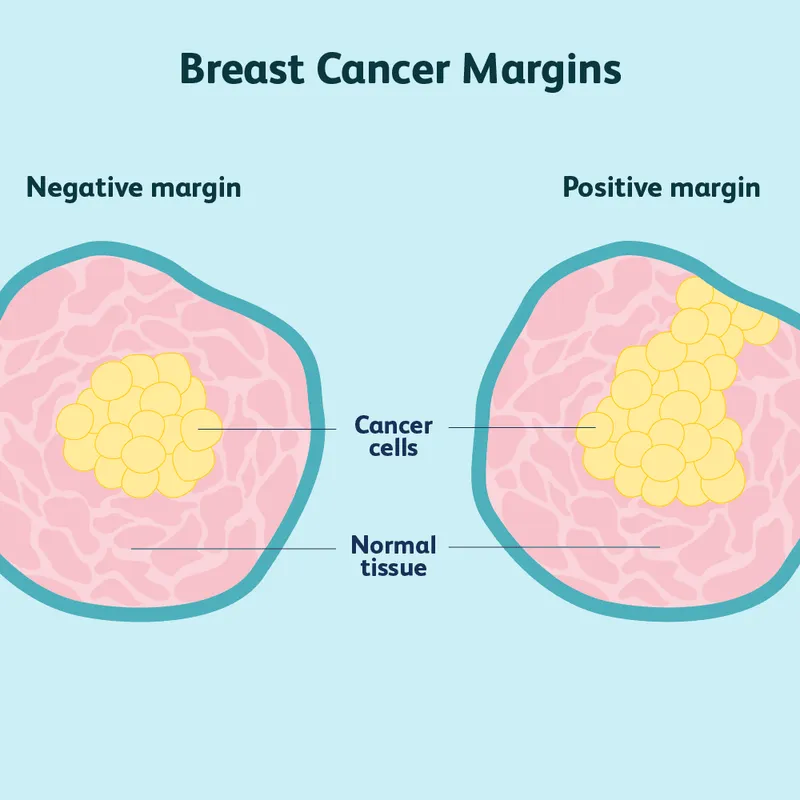
- Surgical Excision: Removal of the tumor with a rim of normal tissue to achieve negative margins ("no ink on tumor").
- Radiation: Adjuvant whole-breast radiation therapy (WBRT) is standard to ↓ local recurrence.
- Axillary Staging: Typically involves sentinel lymph node biopsy (SLNB).
⭐ For early-stage invasive breast cancer (Stage I & II), BCT offers equivalent long-term survival compared to mastectomy.
- Absolute Contraindications:
- Multicentric disease (>1 quadrant)
- Diffuse malignant microcalcifications
- Inflammatory breast cancer
- Prior radiation to the chest/breast
- Inability to achieve negative margins
🎯 The Ideal Candidate
- Primary Goal: Achieve negative surgical margins with a good cosmetic result.
- Core Principle: Patient must be able to receive adjuvant radiation therapy (RT).
Inclusion Criteria:
- Single, unifocal tumor.
- Tumor size < 5 cm (relative to breast size).
- Patient preference for breast conservation.
- No contraindications to RT.
Contraindications to BCT:
- Absolute:
- Multicentric disease (tumors in >1 quadrant).
- Diffuse malignant microcalcifications.
- Inflammatory breast cancer.
- Pregnancy (RT is teratogenic).
- History of prior radiation to the breast/chest.
- Relative:
- Collagen vascular disease (e.g., scleroderma).
- Large tumor in a small breast (poor cosmesis).
⭐ BCT (lumpectomy + radiation) offers equivalent long-term survival rates to mastectomy for most women with early-stage invasive breast cancer.
💃 Management - The Surgical Dance
BCT is a three-part procedure: lumpectomy, nodal evaluation, and radiation.
- Lumpectomy (Wide Local Excision):
- Goal: Achieve negative surgical margins, defined as "no ink on tumor."
- Resects the tumor with a surrounding rim of normal breast tissue.
- Axillary Staging:
- Sentinel Lymph Node Biopsy (SLNB): Standard for clinically node-negative (cN0) patients.
- If SLNB is positive, consider Axillary Lymph Node Dissection (ALND) or regional nodal radiation.
- Adjuvant Radiation Therapy (RT):
- Mandatory component of BCT, typically whole-breast radiation.
- Significantly ↓ risk of ipsilateral breast tumor recurrence.
⭐ For eligible patients with early-stage breast cancer, BCT (lumpectomy + radiation) provides equivalent overall survival rates compared to mastectomy.
⚠️ Complications - When Things Go South
- Surgical (Early):
- Positive Margins: Most common reason for re-operation. Requires re-excision to achieve negative margins ("no ink on tumor").
- Seroma: Most common complication. Fluid collection, usually self-resolves. Symptomatic cases may need aspiration.
- Infection: Cellulitis or abscess.
- Post-Radiation (Late):
- Lymphedema: Chronic arm swelling, risk ↑ with axillary lymph node dissection (ALND).
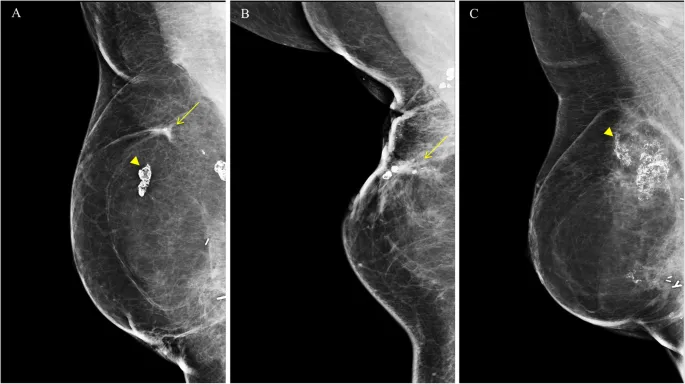
- Fat Necrosis: Benign, can calcify and mimic recurrence on mammogram.
- Poor Cosmesis: Fibrosis, breast asymmetry, skin retraction.
⭐ Positive margins after lumpectomy are the most common indication for re-operation to ensure local control before starting radiation therapy.
⚡ Biggest Takeaways
- Breast Conservation Therapy (BCT) combines lumpectomy with adjuvant radiation.
- Survival rates are equivalent to mastectomy for most early-stage (I/II) invasive cancers.
- Key indications: Unicentric tumor, size typically <5 cm, and ability to achieve negative margins.
- Absolute contraindications: Multicentric disease, diffuse malignant microcalcifications, prior chest radiation, and pregnancy.
- Persistent positive margins after re-excision are an absolute contraindication, requiring mastectomy.
- Sentinel lymph node biopsy (SLNB) is the standard for axillary staging.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

