Islet Anatomy - The Cellular Collective
The Islets of Langerhans are clusters of endocrine cells that act as a coordinated "micro-organ" to regulate blood glucose. Their cellular arrangement is key to their function.
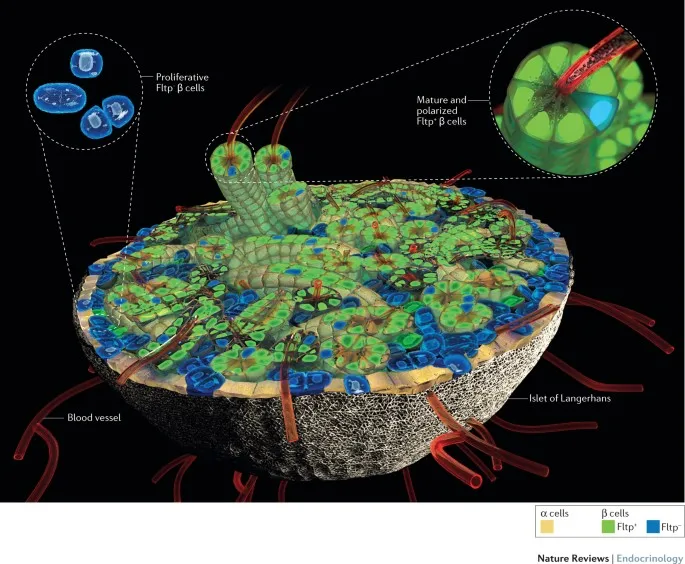
| Cell Type | Hormone(s) | Location in Islet | Primary Function |
|---|---|---|---|
| α (Alpha) | Glucagon | Periphery | ↑ Blood glucose |
| β (Beta) | Insulin, Amylin | Center | ↓ Blood glucose |
| δ (Delta) | Somatostatin | Interspersed | Inhibits α & β cells |
| PP (F cell) | Pancreatic Polypeptide | Periphery | ↓ Exocrine secretion |
Insulin Synthesis & Release - The Glucose Gatekeeper
- Synthesis (in β-cells):
- Preproinsulin synthesized in RER, signal peptide cleaved.
- → Proinsulin folded & disulfide bonds formed in Golgi.
- → Cleaved into Insulin and C-peptide, stored in secretory granules.
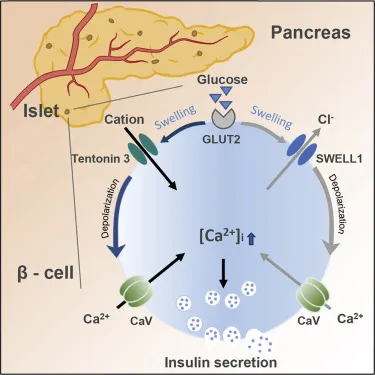
- Glucose-Stimulated Secretion:
⭐ Exam Favorite: Endogenous insulin release produces equimolar amounts of insulin and C-peptide. Measuring C-peptide can differentiate between endogenous insulin production (e.g., insulinoma) and exogenous insulin administration.
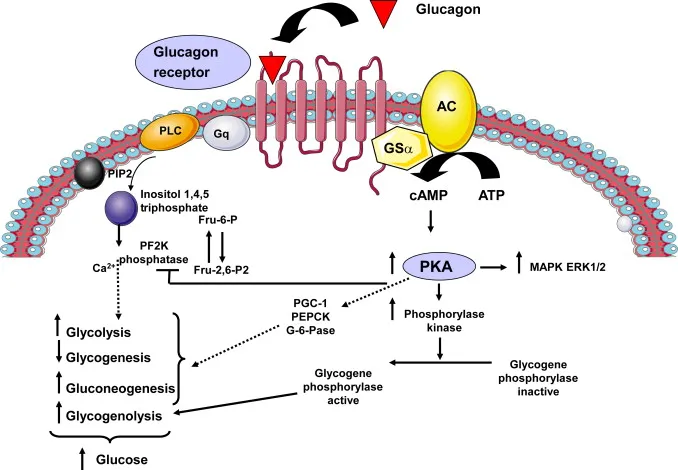
Glucagon & Friends - The Counter-Attack Crew
Secreted by pancreatic α-cells, glucagon is the primary counter-regulatory hormone to insulin.
- Triggers:
- Hypoglycemia (primary stimulus, glucose < 70 mg/dL)
- Amino acids (e.g., arginine)
- Sympathetic stimulation (β-adrenergic)
- Actions (Liver-centric):
- ↑ Glycogenolysis (rapid effect)
- ↑ Gluconeogenesis (slower, sustained effect)
- ↑ Ketogenesis
- Other Players:
- Somatostatin (δ-cells): Universal inhibitor; ↓ insulin & glucagon release.
- Amylin (β-cells): Co-secreted with insulin; ↓ glucagon secretion.
⭐ Glucagonoma: A rare tumor of α-cells, presents with necrolytic migratory erythema, diabetes, and weight loss.
Pancreatic Pathophysiology - When Sweet Goes Sour
| Feature | Type 1 DM | Type 2 DM |
|---|---|---|
| Onset | < 30 years | > 40 years |
| Pathophysiology | Autoimmune β-cell destruction | Insulin resistance, β-cell dysfunction |
| Genetics | HLA-DR3 & DR4 association | Strong polygenic predisposition |
| Insulin Level | ↓↓ | Normal/↑ → ↓ |
| Ketoacidosis | Common | Rare |
| Histology | Islet leukocytic infiltrate | Islet amyloid polypeptide (IAPP) deposits |
- *Whipple's Triad:* ↓ plasma glucose, neuroglycopenic symptoms (e.g., confusion, anxiety), and symptom resolution with glucose administration.
- Glucagonoma: Tumor of α-cells.
- 📌 4 D's: Dermatitis (necrolytic migratory erythema), Diabetes, DVT, Depression.
⭐ Exam Favorite: Autoantibodies against glutamic acid decarboxylase (anti-GAD65) are a key marker for Type 1 Diabetes and can be detected years before clinical onset.
High‑Yield Points - ⚡ Biggest Takeaways
- Insulin, from β-cells, drives glucose into muscle and adipose tissue via GLUT4.
- Glucagon, from α-cells, counters by promoting hepatic glycogenolysis and gluconeogenesis.
- C-peptide is co-secreted with insulin, making it a key marker of endogenous insulin production.
- Somatostatin from δ-cells acts as a universal inhibitor of pancreatic endocrine secretion.
- Glucose is the primary physiological stimulus for insulin release from β-cells.
- Sulfonylureas and meglitinides close the ATP-sensitive K+ channel to trigger insulin secretion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

