Mineralocorticoids - Salty Survival Hormones
- Primary Hormone: Aldosterone, from Zona Glomerulosa.
- Primary Target: Principal cells of the distal convoluted tubule (DCT) & collecting ducts.
- Core Actions:
- ↑ Na⁺ reabsorption (water follows) → ↑ ECF volume & BP.
- ↑ K⁺ secretion.
- ↑ H⁺ secretion (via intercalated cells).
⭐ Aldosterone Escape: In primary hyperaldosteronism, chronic high aldosterone leads to initial Na⁺/water retention, but compensatory mechanisms (like ANP release) cause natriuresis, preventing overt hypernatremia and edema.
Mechanism of Action - The Nuclear Receptor Dance
- Entry & Binding: Lipid-soluble aldosterone freely diffuses into principal cells (distal tubule/collecting duct) and binds to its cytoplasmic Mineralocorticoid Receptor (MR).
- Translocation & Transcription: The hormone-receptor complex translocates to the nucleus, binds to a hormone response element on DNA, and initiates transcription.
- Protein Synthesis: Upregulates synthesis of key transport proteins:
- Apical membrane: Epithelial Na+ Channels (ENaC)
- Basolateral membrane: Na+/K+ ATPase pumps
⭐ Cortisol's Cross-Talk: Cortisol can also activate the MR. In aldosterone-sensitive tissues, the enzyme 11β-hydroxysteroid dehydrogenase type 2 (11β-HSD2) locally inactivates cortisol to cortisone, ensuring aldosterone specificity.
Physiological Effects - Salt, Water, Pressure

- Primary Action: Acts on principal cells of the distal nephron (DCT & collecting duct).
- Mechanism: ↑ synthesis and insertion of key transporters.
- Luminal: ↑ ENaC (Na⁺ reabsorption) & ↑ ROMK (K⁺ secretion).
- Basolateral: ↑ Na⁺/K⁺-ATPase activity to drive the gradients.
- Net Result:
- ↑ Salt Retention: Na⁺ reabsorption from urine.
- ↑ Water Retention: Water follows Na⁺, expanding ECF volume.
- ↑ Blood Pressure: Due to volume expansion.
- ↑ K⁺ & H⁺ excretion, leading to potential hypokalemia and metabolic alkalosis.
⭐ Aldosterone Escape: In states of aldosterone excess, high volume/pressure triggers natriuretic peptides (ANP) to limit edema, but urinary K⁺/H⁺ wasting continues, sustaining hypokalemia and metabolic alkalosis.
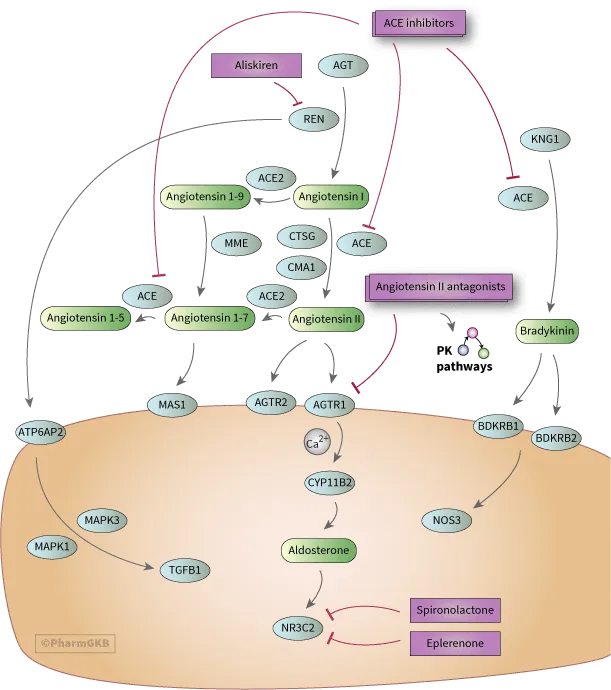
Regulation - The RAAS & Potassium Show
- Primary Drivers: Angiotensin II & extracellular K⁺ concentration.
- RAAS Cascade: The main pathway for aldosterone release.
- Potassium's Role:
- Hyperkalemia is a potent, direct stimulator of aldosterone secretion, acting as a key defense against high K⁺.
- Minor Regulators:
- ACTH: Has a transient, permissive effect.
- ANP: Inhibits renin and aldosterone release in response to atrial stretch (high volume).
⭐ While the RAAS is the classic pathway, severe hyperkalemia can stimulate aldosterone release independently of Angiotensin II.
Pathophysiology - Too Much or Too Little
- Hyperaldosteronism (Conn's Syndrome): ↑Na⁺/H₂O retention → Hypertension. ↑K⁺/H⁺ excretion → Hypokalemic metabolic alkalosis.
- Hypoaldosteronism: ↓Na⁺/H₂O retention → Hypotension. ↓K⁺/H⁺ excretion → Hyperkalemic metabolic acidosis (Type 4 RTA).
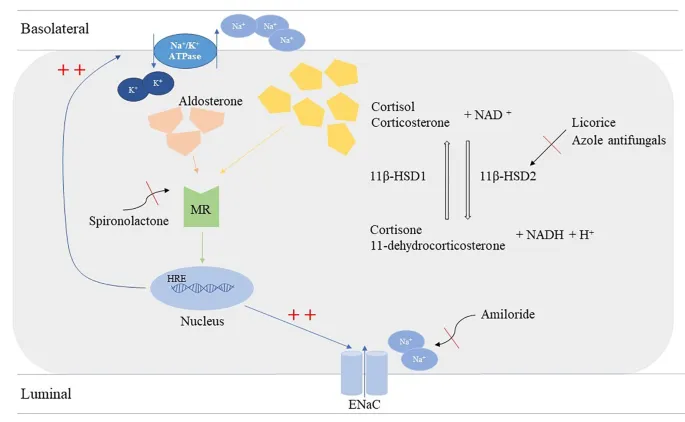
⭐ Licorice (glycyrrhetinic acid) inhibits 11β-HSD2, causing cortisol to activate mineralocorticoid receptors, mimicking hyperaldosteronism.
High‑Yield Points - ⚡ Biggest Takeaways
- Aldosterone primarily acts on the principal cells of the late distal tubule & collecting duct.
- It upregulates ENaC channels to increase Na+ reabsorption and ROMK channels to increase K+ secretion.
- It also stimulates H+ secretion from α-intercalated cells, potentially causing metabolic alkalosis.
- The net effect is increased blood volume and blood pressure.
- Primary regulation is via angiotensin II and serum K+ levels, not ACTH.
- Hyperaldosteronism classically presents with hypertension, hypokalemia, and metabolic alkalosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

