Insulin Synthesis & Secretion - The Sugar Sheriff
- Synthesis: In pancreatic β-cells, preproinsulin is cleaved into insulin and C-peptide. Both are stored in granules. C-peptide has a longer half-life than insulin, making it a stable marker.
- Secretion Triggers:
- Primary: ↑ Blood glucose is the main driver.
- Potentiators: Incretins (GLP-1, GIP), β₂-adrenergic agonists, vagal stimulation (ACh).
- Inhibitors: Somatostatin, α₂-adrenergic agonists, prostaglandins.
Glucose-Stimulated Secretion Pathway:
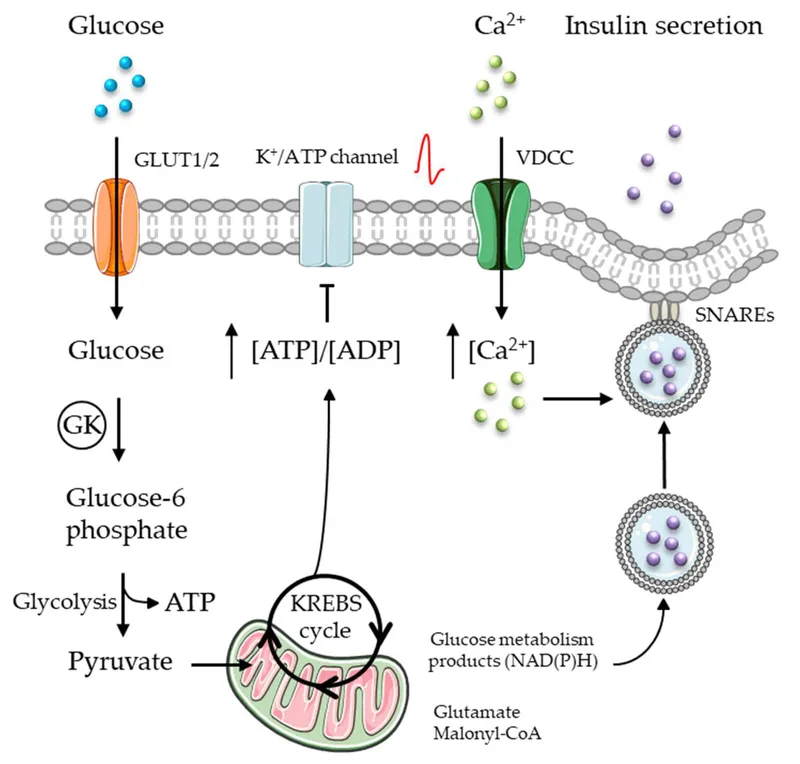
⭐ C-peptide is secreted 1:1 with insulin and is the best measure of endogenous production. This helps distinguish T1DM (low/absent) from T2DM (normal/high) and factitious hypoglycemia.
Insulin's Cellular Action - The Receptor's Reach
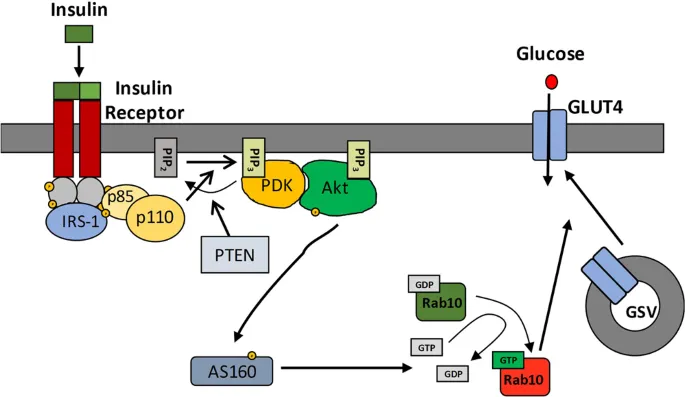
- Receptor: Cell surface tyrosine kinase receptor (2α, 2β subunits).
- Mechanism:
- Insulin binding → receptor autophosphorylation.
- Phosphorylation of Insulin Receptor Substrate (IRS).
- Activation of the PI3K/Akt signaling pathway.
- Key Actions:
- Glucose Transport: Rapid translocation of GLUT4 to cell membranes of skeletal muscle and adipose tissue.
- Metabolic Effects (Anabolic):
- ↑ Glycogen synthesis (liver, muscle).
- ↑ Protein synthesis.
- ↑ Lipogenesis.
- ↓ Gluconeogenesis & lipolysis.
⭐ Insulin-Independent Glucose Uptake: Remember that Brain, RBCs, Intestine, Cornea, Kidney, and Liver (BRICK-L) utilize GLUT1, GLUT2, or GLUT3 and do not depend on insulin for glucose uptake.
Metabolic Effects - Master Fuel Regulator
Insulin is the principal anabolic hormone, promoting fuel storage in the "fed state." It lowers blood glucose by increasing uptake and utilization while inhibiting endogenous production of glucose and fats.
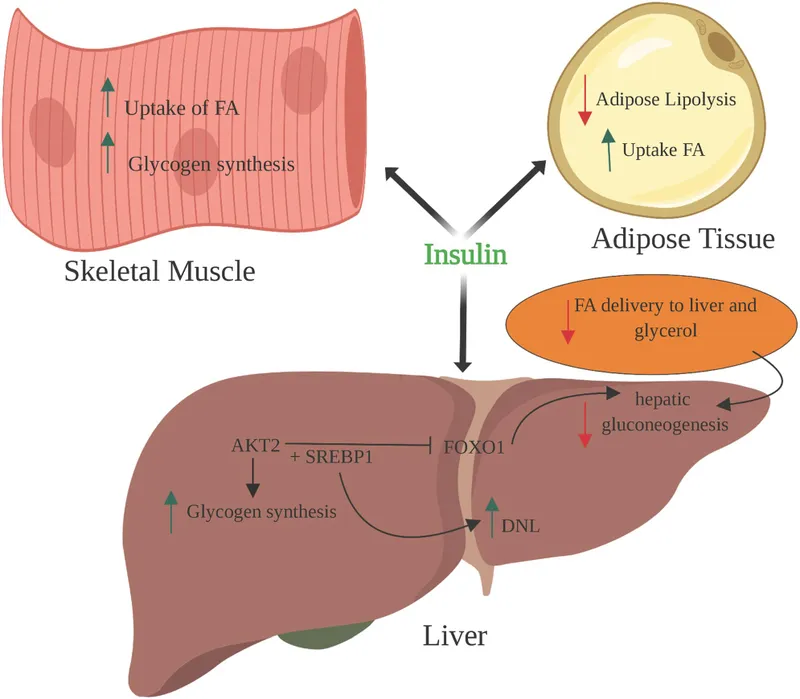
- Carbohydrate Metabolism
- ↑ Glucose uptake (muscle, adipose tissue) via GLUT4 translocation.
- ↑ Glycolysis & Acetyl-CoA production.
- ↑ Glycogen synthesis (liver, muscle).
- ↓ Glycogenolysis & gluconeogenesis.
- Fat Metabolism
- ↑ Lipogenesis & triglyceride storage (adipose).
- ↓ Lipolysis by inhibiting hormone-sensitive lipase.
- ↓ Ketogenesis.
- Protein & Ion Balance
- ↑ Amino acid uptake & protein synthesis (muscle).
- ↑ K+ uptake into cells (activates Na+/K+ ATPase).
⭐ Insulin drives potassium into cells; IV insulin for hyperkalemia can cause iatrogenic hypokalemia if K+ is not co-administered.
Regulation of Secretion - The Control Panel
- Primary Stimulus: ↑ Plasma Glucose
- Amplifiers (Potentiators):
- Hormonal: Incretins (GLP-1, GIP), β2-adrenergic agonists.
- Neural: Vagal stimulation (ACh).
- Nutrients: Amino acids (arginine, leucine), fatty acids.
- Inhibitors:
- Hormonal: Somatostatin, epinephrine (via α2-receptors).
- Neural: Sympathetic stimulation (α2 effect dominates).
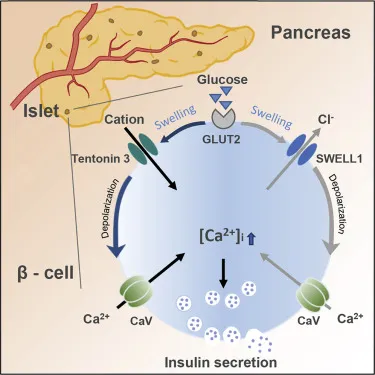
⭐ Exam Favorite: Sulfonylurea drugs (e.g., Glyburide, Glipizide) bypass glucose metabolism and directly close the ATP-sensitive K+ channels to stimulate insulin secretion.
- Glucose enters pancreatic β-cells via GLUT2, serving as the primary stimulus for insulin secretion.
- ↑ATP from glucose metabolism closes ATP-sensitive K+ channels, leading to depolarization and Ca2+-mediated exocytosis of insulin.
- Insulin binds to tyrosine kinase receptors, activating the PI3K/Akt pathway.
- It promotes GLUT4 translocation to the membrane in muscle and adipose tissue.
- Key anabolic effects: ↑glucose uptake, ↑glycogenesis, ↑lipogenesis, and ↑protein synthesis.
- Incretins (GLP-1) potentiate release; somatostatin inhibits it.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

