Thyroid Physiology - Hormone Factory HQ
- Axis: Hypothalamus (TRH) → Anterior Pituitary (TSH) → Thyroid Gland.
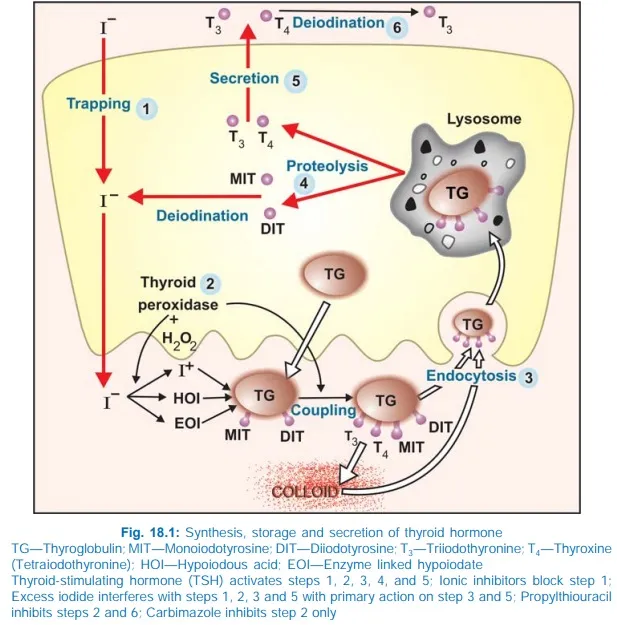
- Key Enzyme: Thyroid Peroxidase (TPO) drives oxidation & organification of iodide.
- Products: Thyroxine ($T_4$) and Triiodothyronine ($T_3$) are synthesized and stored in colloid, bound to thyroglobulin.
- Ratio: Thyroid secretes $T_4$ to $T_3$ in a ~20:1 ratio.
⭐ High-Yield: The vast majority (~80%) of active $T_3$ is generated from the peripheral deiodination of $T_4$, primarily in the liver and kidneys.
The Replacements - Drug Lineup
-
Levothyroxine (Synthroid, Levoxyl): Synthetic T4.
- Drug of choice for hypothyroidism.
- Metabolized to T3 peripherally; long half-life (~7 days) allows for stable, once-daily dosing.
- Take on an empty stomach, 30-60 minutes before breakfast.
- Steady state achieved in 6-8 weeks.
-
Liothyronine (Cytomel): Synthetic T3.
- Faster onset, shorter half-life (~1 day).
- Primarily used for myxedema coma (IV) or short-term TSH suppression.
- Associated with ↑ cardiotoxicity risk.
-
Liotrix: Synthetic T4:T3 in a 4:1 ratio.
-
Desiccated Thyroid Extract (Armour Thyroid): Porcine-derived.
- Contains T4 & T3; inconsistent potency and antigenicity concerns.

⭐ Levothyroxine's long half-life is a key clinical advantage. It ensures a stable reservoir, meaning a missed dose doesn't cause significant fluctuation, making it forgiving for patients and reliable for maintaining euthyroid states.
Dosing & Monitoring - The Titration Game
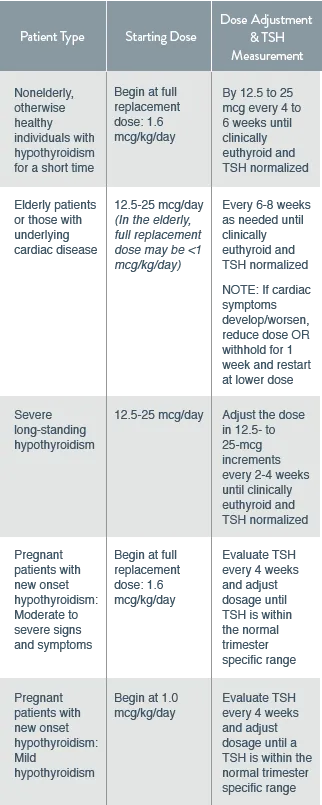
- Initial Dose (Levothyroxine):
- Standard: ~$1.6$ mcg/kg/day (ideal body weight).
- Elderly / Cardiac Disease: Start low, go slow. Initial dose 12.5-25 mcg/day to avoid cardiac stress.
- Titration & Monitoring:
- Primary Goal: Normalize TSH to 0.4-4.0 mIU/L.
- Check TSH 4-6 weeks after any dose change.
- Adjust dose by 12.5-25 mcg increments.
- High TSH (Hypo): ↑ Levothyroxine dose.
- Low TSH (Hyper): ↓ Levothyroxine dose.
- Special Considerations:
- Pregnancy: Often requires a dose ↑ of 30-50%.
⭐ Levothyroxine's long half-life (~7 days) means steady state takes over a month. This is why TSH is re-checked 4-6 weeks post-dose adjustment, not earlier.
Adverse Effects & Interactions - Too Much of a Good Thing
Essentially iatrogenic hyperthyroidism. Symptoms mirror thyrotoxicosis.
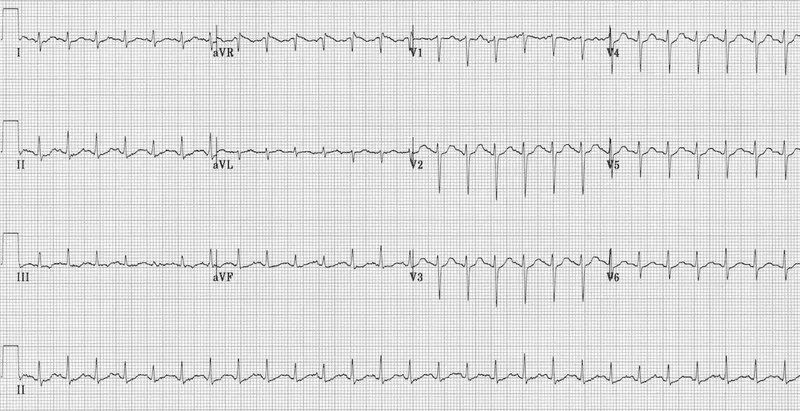
- Cardiovascular: Tachycardia, palpitations, angina, arrhythmias (esp. atrial fibrillation in elderly).
- Neurological: Nervousness, anxiety, tremor, insomnia.
- Metabolic/General: ↑ aBMR, weight loss despite ↑ appetite, heat intolerance, sweating.
- Musculoskeletal: Muscle weakness, ↑ bone turnover leading to osteoporosis with long-term overuse.
⭐> High-Yield: Over-replacement, especially in older adults, significantly increases the risk of atrial fibrillation and accelerated osteoporosis.
Drug Interactions:
- ↓ Absorption: Bile acid sequestrants (cholestyramine), iron, calcium supplements, PPIs.
- ↑ Metabolism: Rifampin, Phenytoin, Carbamazepine induce CYP450 enzymes.
High‑Yield Points - ⚡ Biggest Takeaways
- Levothyroxine (T4) is the mainstay treatment for hypothyroidism, acting as a prodrug converted to active T3 peripherally.
- Liothyronine (T3) has a faster onset and is reserved for severe, acute conditions like myxedema coma.
- Monitor therapy with TSH levels; the goal is to bring TSH into the normal range.
- Adverse effects are symptoms of iatrogenic hyperthyroidism: palpitations, anxiety, and weight loss.
- Take on an empty stomach; absorption is impaired by food, iron, and calcium.
- Increases warfarin's anticoagulant effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

