NSAIDs - The COX Blockers
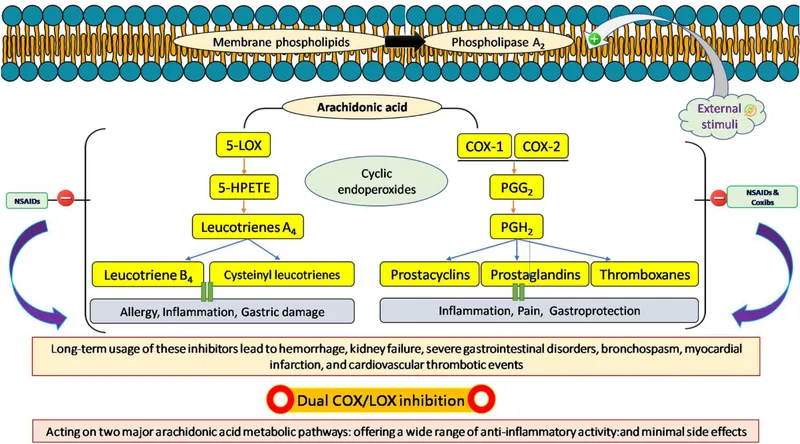
- Mechanism: Inhibit cyclooxygenase (COX) enzymes, blocking prostaglandin (PG) and thromboxane (TXA₂) synthesis from arachidonic acid.
- COX-1 (Constitutive): Protects gastric mucosa, supports renal function, promotes platelet aggregation.
- COX-2 (Inducible): Mediates inflammation, pain, and fever.
-
Classes & Agents:
- Non-selective (COX-1 & COX-2): Ibuprofen, Naproxen, Indomethacin, Ketorolac.
- COX-2 Selective: Celecoxib (less GI toxicity, ↑ CV risk).
- Irreversible (Aspirin): Unique cardioprotective antiplatelet effect.
-
Key Adverse Effects:
- GI: Gastritis, ulcers, bleeding (due to ↓ protective PGs).
- Renal: ↓ GFR, acute kidney injury, interstitial nephritis.
- CV: ↑ BP, edema, ↑ thrombosis risk (especially COX-2 selective).
⭐ Aspirin toxicity classically presents with a mixed respiratory alkalosis (early stimulation of medullary respiratory center) and a high anion gap metabolic acidosis (late). Tinnitus is a common early sign.
Acetaminophen - The Liver's Nemesis
- Mechanism: Reversibly inhibits cyclooxygenase (COX), mostly in the CNS. Inactivated peripherally, so it lacks significant anti-inflammatory effects compared to NSAIDs.
- Use: Antipyretic and analgesic. Used when NSAIDs are contraindicated (e.g., peptic ulcer disease, renal disease, bleeding risk).
- Toxicity: Overdose causes severe hepatotoxicity. The toxic metabolite, N-acetyl-p-benzoquinone imine (NAPQI), depletes glutathione stores, leading to hepatocellular necrosis.
⭐ The Rumack-Matthew nomogram is used to assess hepatotoxicity risk post-ingestion and guide the need for N-acetylcysteine therapy.
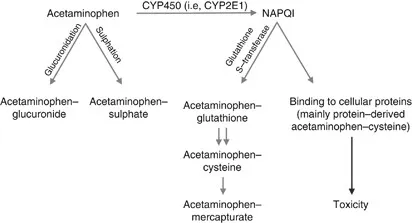
- Antidote: N-acetylcysteine (NAC) regenerates glutathione, which detoxifies NAPQI. Most effective when given within 8-10 hours of ingestion.
Aspirin - The Platelet Poison
- MOA: Irreversibly inhibits cyclooxygenase (COX-1 and COX-2) via acetylation.
- Blocks synthesis of prostaglandins & thromboxane A₂ (TXA₂).
- Dose-Dependent Effects:
- Low (<300 mg/day): ↓ platelet aggregation.
- Intermediate (300-2400 mg/day): Antipyretic & analgesic.
- High (2400-4000 mg/day): Anti-inflammatory.
- Kinetics: Follows zero-order elimination at high, toxic doses.
- Adverse Effects:
- GI bleeding/ulcers, tinnitus (salicylism).
- ⚠️ Reye's syndrome in children with viral illness.
⭐ Clinical Pearl: Due to irreversible inhibition, the antiplatelet effect lasts for the lifespan of the platelet (~7-10 days).
High‑Yield Points - ⚡ Biggest Takeaways
- Acetaminophen acts centrally; its overdose, causing hepatotoxicity, is treated with N-acetylcysteine.
- NSAIDs non-selectively block COX-1 and COX-2, risking GI ulcers, nephrotoxicity, and cardiovascular events.
- Aspirin is an irreversible COX inhibitor with antiplatelet effects; it can cause Reye's syndrome in children.
- Celecoxib, a selective COX-2 inhibitor, spares the GI tract but increases thrombotic risk and carries a sulfa allergy warning.
- Ketamine, an NMDA receptor antagonist, provides potent analgesia and dissociative anesthesia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

