Antimicrobial Stewardship - Saving Bucks & Bugs
- Core Goal: Optimize clinical outcomes while minimizing unintended consequences like resistance, toxicity, and cost. Balances individual patient needs with public health.
- Key Interventions:
- De-escalation: Narrowing antibiotic spectrum based on culture results. Go from broad to targeted.
- IV-to-PO Switch: Convert to oral therapy once patient is stable, afebrile, and can tolerate PO intake. Reduces cost & complications.
- Formulary Restriction: Limiting use of broad-spectrum or high-cost agents to specific criteria or requiring pre-authorization.
- Dose Optimization: Using PK/PD principles for optimal killing and minimal toxicity.
⭐ Rapid Diagnostic Tests (e.g., MALDI-TOF, PCR) can decrease time to effective therapy by >24 hours, reducing length of stay and costs.
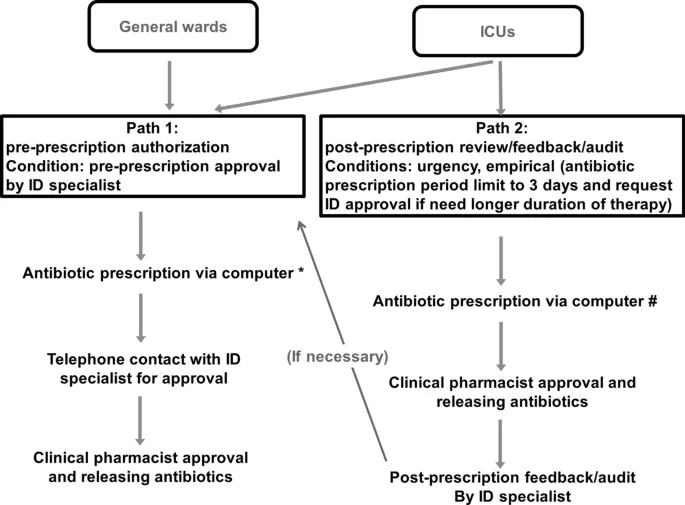
Core Strategies - The Switch & Ditch
Two key principles to reduce antimicrobial cost, resistance, and complications.
1. IV-to-PO Switch Therapy
- When? Patient must be:
- Hemodynamically stable
- Afebrile for >24 hours
- Showing clinical improvement (↓ WBC, ↓ symptoms)
- Able to tolerate oral intake (functioning GI tract)
- Why? ↓ Hospital stay, ↓ costs, ↓ risk of catheter-related infections.
- What? Use drugs with high oral bioavailability.
| Drug Class | Excellent Bioavailability (>90%) |
|---|---|
| Fluoroquinolones | Levofloxacin, Moxifloxacin |
| Azoles | Fluconazole, Voriconazole |
| Tetracyclines | Doxycycline, Minocycline |
| Other | Metronidazole, Linezolid, TMP-SMX |
- When? As soon as culture & sensitivity (C&S) data are available.
- What? Switch from broad-spectrum empiric therapy to a narrow-spectrum agent.
- Why? ↓ Selective pressure for multidrug-resistant organisms & ↓ collateral damage.
- 📌 Mnemonic: Stop the "shotgun" approach; use a "sniper rifle" once the target is known.
⭐ Exam Favorite: Don't assume an oral version exists! IV-only drugs like carbapenems and piperacillin-tazobactam require switching to an entirely different agent (e.g., a fluoroquinolone or cephalosporin) based on sensitivities for the PO route.
Stewardship Metrics - The Numbers Game
- Primary Goal: Quantify antimicrobial use to guide interventions & assess impact.
- Key Consumption Metrics:
- Defined Daily Doses (DDD): Assumed average maintenance dose per day for a drug.
- Unit: DDDs per 100 patient-days.
- Use: Benchmarking consumption across institutions.
- Limitation: Doesn't reflect actual prescribed doses (e.g., renal adjustments).
- Days of Therapy (DOT): Number of days a patient receives an antimicrobial, regardless of dose.
- Unit: DOTs per 1,000 patient-days.
- Use: More patient-centric; reflects true therapy duration.
- Defined Daily Doses (DDD): Assumed average maintenance dose per day for a drug.
⭐ DOT is preferred over DDD for internal hospital tracking as it accurately reflects antibiotic exposure, unlike DDD which can be skewed by dose adjustments (e.g., for renal failure).
- Outcome Metrics:
- ↓ Hospital Length of Stay (LOS).
- ↓ Antimicrobial cost.
- ↓ C. difficile infection rates.
High‑Yield Points - ⚡ Biggest Takeaways
- De-escalation therapy is critical: start with broad-spectrum coverage, then narrow down based on culture and sensitivity results to reduce cost and resistance.
- Early IV-to-PO switch for clinically stable patients significantly cuts costs and shortens hospital stays.
- Utilize dose optimization strategies, like extended-infusion beta-lactams, to maximize efficacy and minimize waste.
- Formulary restrictions and pre-authorization are key tools for antimicrobial stewardship programs (ASPs).
- Always consider generic equivalents over brand-name drugs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

