Tumor Antigens - Spotting the Enemy
-
Tumor-Specific Antigens (TSAs):
- Found exclusively on tumor cells.
- Primarily neoantigens resulting from mutations; these are highly immunogenic.
-
Tumor-Associated Antigens (TAAs):
- Also on normal cells, but expression is altered.
- Oncofetal antigens: AFP, CEA.
- Differentiation antigens: CD20 on B-cells.
- Overexpressed proteins: HER2 in breast cancer.
- Viral antigens: HPV E6/E7 in cervical cancer.
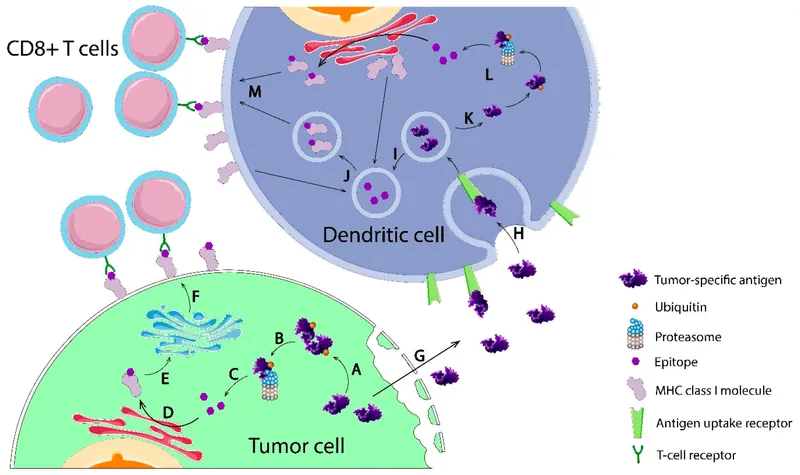
⭐ Neoantigens, arising from somatic mutations, are highly immunogenic and are the principal targets for effective T-cell-mediated tumor destruction.
Immune Surveillance - The Cancer Patrol
The immune system's intrinsic ability to recognize and eliminate cancer cells. This process, primarily cell-mediated, involves a coordinated attack on tumor cells.
-
Key Cellular Players:
- Cytotoxic T-Lymphocytes (CTLs): The primary assassins. Recognize tumor antigens on MHC-I and induce apoptosis.
- Natural Killer (NK) Cells: Innate defenders. Target cells with ↓MHC-I expression (a common tumor evasion tactic).
- Macrophages: Dual role. M1 (pro-inflammatory) are tumoricidal; M2 (pro-tumor) can promote growth.
- Dendritic Cells (DCs): The messengers. Capture tumor antigens and present them to T-cells (cross-presentation).
-
Key Cytokines: IFN-γ, TNF-α, IL-12 orchestrate the anti-tumor response.

⭐ The 'cancer-immunity cycle' describes the series of steps required for an effective anti-tumor immune response, from antigen release to cancer cell killing.
Immune Evasion - Cancer's Cloaking Device
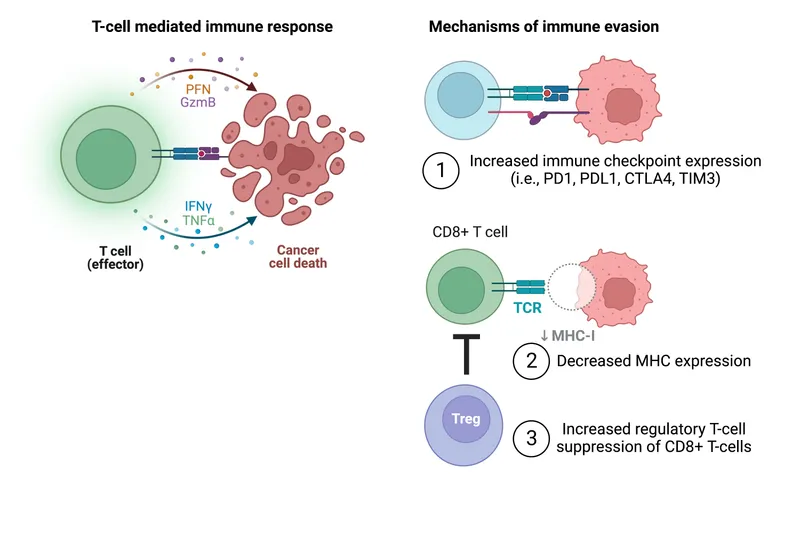
- Antigenic Modulation: Cancer cells lose or mask tumor-specific antigens (TSAs), effectively becoming "invisible" to patrolling T cells.
- MHC Downregulation: ↓ MHC-I expression on the tumor cell surface prevents cytotoxic T lymphocytes (CTLs) from recognizing and killing them.
- Immune Checkpoint Upregulation: ↑ expression of proteins like PD-L1 and CTLA-4, which act as "brakes" to deactivate T cells.
- Immunosuppressive Environment: Secretion of cytokines like TGF-β and IL-10 to inhibit T-cell and NK-cell function.
- Recruitment of Suppressor Cells: Induction of regulatory T cells (Tregs) and Myeloid-Derived Suppressor Cells (MDSCs) to actively turn off the anti-tumor response.
⭐ Tumors frequently upregulate PD-L1 expression, which binds to PD-1 on activated T cells, inducing T-cell 'exhaustion' and allowing the tumor to escape immune destruction.
📌 Mnemonic: "HIDE"
- Hide Antigens
- Inhibit T-cells (PD-L1, CTLA-4)
- Downregulate MHC
- Emit suppressive signals (TGF-β, IL-10)
Immunotherapy - Re-Arming the Guards
Modern therapies leveraging the body's immune system to fight cancer by overcoming tumor defense mechanisms.
-
Checkpoint Inhibitors: Release the "brakes" on T-cells, enabling them to attack cancer.
- Anti-PD-1/PD-L1 (e.g., Pembrolizumab): Blocks T-cell exhaustion signals.
- Anti-CTLA-4 (e.g., Ipilimumab): Prevents early T-cell inactivation.
⭐ Immune-related adverse events (irAEs) are a unique and critical side effect profile of checkpoint inhibitors, caused by generalized immune activation against normal tissues.
-
Adoptive Cell Transfer (ACT): Harvest, modify, and re-infuse a patient's T-cells.
- CAR-T Cells: T-cells engineered with Chimeric Antigen Receptors (e.g., anti-CD19).
- Tumor-Infiltrating Lymphocytes (TIL): Expansion of naturally anti-tumor T-cells.
-
Monoclonal Antibodies: Target specific tumor antigens for destruction.
- Rituximab: anti-CD20 (B-cell lymphomas).
- Trastuzumab: anti-HER2 (breast cancer).
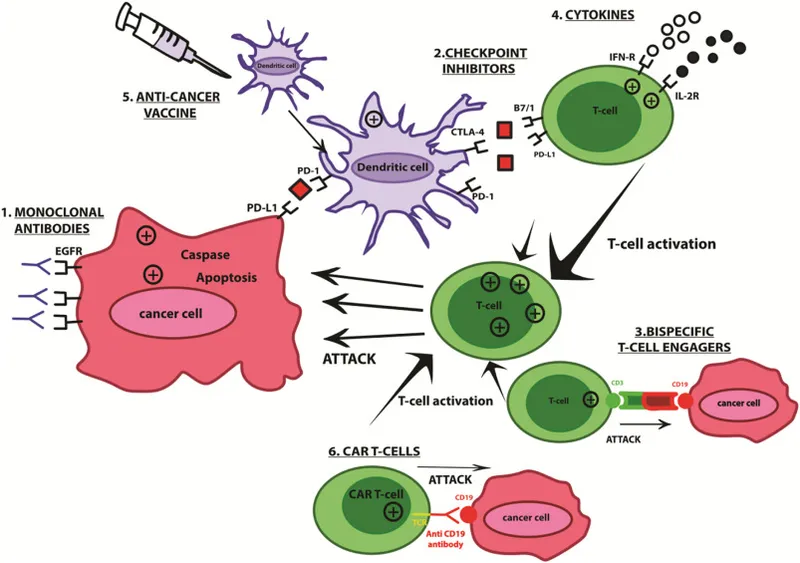
- Cancer Vaccines: Prophylactic (HPV) or therapeutic (Sipuleucel-T).
- Cytokine Therapy: Broad immune stimulation (e.g., IL-2, IFN-α).
High‑Yield Points - ⚡ Biggest Takeaways
- Cytotoxic T-lymphocytes (CTLs) are the primary mediators of anti-tumor immunity, recognizing tumor antigens via MHC-I.
- Tumors evade immunity by downregulating MHC-I, expressing PD-L1 to induce T-cell exhaustion, and secreting immunosuppressive cytokines like TGF-β.
- Checkpoint inhibitors (e.g., anti-PD-1, anti-CTLA-4) block negative signals to T-cells, restoring their anti-cancer activity.
- Natural Killer (NK) cells provide innate immunity by killing cells that have lost MHC-I expression.
- CAR-T cell therapy engineers a patient's T-cells to target tumor antigens, effective in hematologic cancers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

