MHC/HLA - The Body's Barcode
- MHC (Major Histocompatibility Complex), or HLA (Human Leukocyte Antigen) in humans, is the core genetic system for distinguishing self from non-self.
- Allorecognition: The process where a recipient's T-cells recognize donor HLA molecules as foreign, initiating rejection.
- Key Loci & Function:
- Class I (HLA-A, B, C): On all nucleated cells; present endogenous antigens to CD8+ cytotoxic T-cells.
- Class II (HLA-DP, DQ, DR): On antigen-presenting cells (APCs); present exogenous antigens to CD4+ helper T-cells.
📌 Mnemonic: Rule of 8s: Class I binds CD8 (1x8=8); Class II binds CD4 (2x4=8).
⭐ HLA-DR and -DQ mismatches are considered the most critical for initiating both transplant rejection and graft-versus-host disease.
Hyperacute Rejection - Instant Annihilation
- Mechanism: Type II Hypersensitivity. Occurs in minutes to hours due to pre-existing recipient antibodies (e.g., anti-ABO, anti-HLA) binding to donor antigens.
- Pathology: Leads to complement activation, endothelial damage, widespread thrombosis, and ischemic necrosis.

⭐ Prevented by pre-transplant ABO blood typing and lymphocytotoxic cross-match tests to detect reactive antibodies in the recipient against donor cells.
Acute Rejection - The Weeks-Long War
Occurs weeks to months post-transplant; most common type. Often reversible with immunosuppressants.
Two main mechanisms:
-
Cellular (More Common): T-cell mediated (Type IV hypersensitivity).
- Host CD8+ and CD4+ T-cells are sensitized against donor MHC antigens.
- Histology: Dense interstitial lymphocytic infiltrate & endotheliitis (vasculitis).
-
Humoral: Antibody-mediated (Type II hypersensitivity).
- Antibodies develop post-transplant against donor antigens.
- Histology: Necrotizing vasculitis, neutrophils, and C4d deposition.
⭐ C4d deposition in peritubular capillaries is a key indicator of antibody-mediated rejection, acting as a footprint of complement activation.
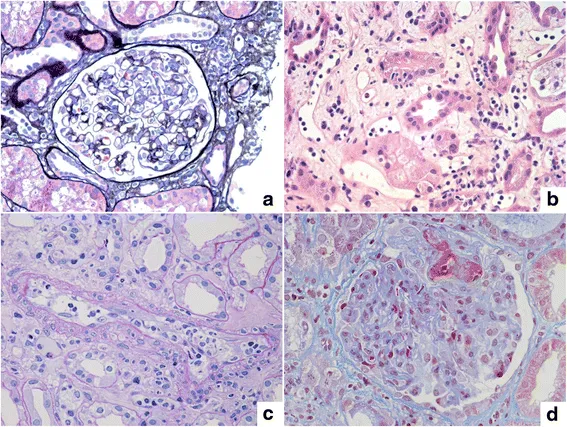
Chronic Rejection - The Slow Burn
- Mechanism: Months to years post-transplant; a slow, progressive T-cell and B-cell mediated response (Type III & IV Hypersensitivity).
- Pathology: Chronic inflammation leads to fibrosis, parenchymal atrophy, and obliterative vasculopathy (graft arteriosclerosis).
- Results in gradual, irreversible loss of graft function.
- Organ-Specific Findings:
- Lung: Bronchiolitis obliterans.
- Liver: Vanishing bile duct syndrome.
- Kidney: Graft nephropathy (fibrosis & atrophy).
⭐ Chronic rejection is the leading cause of long-term graft failure and is often refractory to treatment.

GVHD - When Grafts Attack
- Pathophysiology: Donor T-cells from the graft recognize the recipient's tissues as foreign and attack. This is a Type IV Hypersensitivity reaction, primarily seen in immunocompromised hosts (e.g., bone marrow transplant).
- Clinical Triad:
- Skin: Diffuse maculopapular rash.
- Liver: Jaundice, ↑ LFTs.
- GI Tract: Diarrhea, cramping, bleeding.
- 📌 Mnemonic: See, Yellow, Go (Skin rash, Jaundice, GI upset).
⭐ High-Yield: The same mechanism can be beneficial, causing a "graft-versus-leukemia" effect where donor T-cells attack residual cancer cells.

High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection is a Type II HSR due to pre-formed recipient antibodies attacking the graft within minutes.
- Acute rejection is primarily T-cell mediated (Type IV HSR), occurring weeks to months post-transplant; may also be antibody-mediated.
- Chronic rejection involves T-cells and antibodies (Type II & IV HSR), leading to irreversible fibrosis and arteriosclerosis over months to years.
- Graft-vs-Host Disease (GVHD) results from donor T-cells attacking host tissues, common after bone marrow transplant.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

