First Trimester Screen - The Early Peek
- When: 11-14 weeks gestation.
- Components:
- Maternal Serum: Pregnancy-associated plasma protein-A (PAPP-A) & free β-hCG.
- Ultrasound: Nuchal Translucency (NT).
- Screens for: Aneuploidies, primarily Trisomy 21 & 18.
- Abnormal Patterns:
- Trisomy 21: ↓ PAPP-A, ↑ β-hCG, ↑ NT. (📌 Mnemonic: Down syndrome has High hCG).
- Trisomy 18: ↓ PAPP-A, ↓ β-hCG, ↑ NT.
⭐ The "combined test" (this screen + maternal age) detects ~85% of Down syndrome cases. A positive screen is NOT diagnostic; it indicates increased risk requiring further testing.
Screening Components - The Telltale Trio
Combined first-trimester screening (cFTS) integrates ultrasound findings with maternal serum analytes between 11-14 weeks gestation to calculate aneuploidy risk.
-
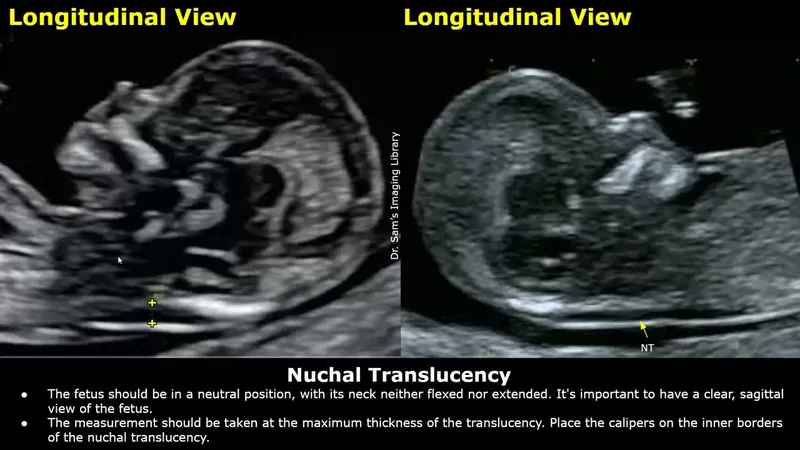
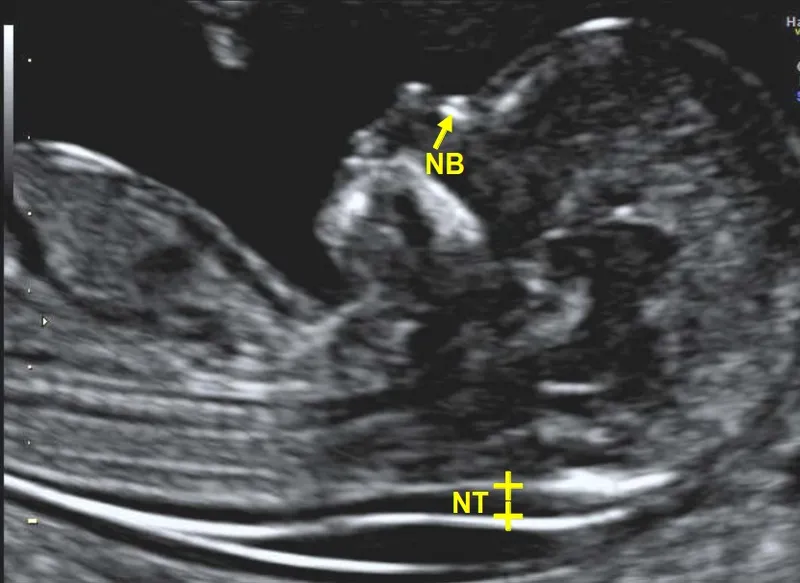
Nuchal Translucency (NT) on Ultrasound
- Measures subcutaneous fluid at the back of the fetal neck.
- ↑ NT suggests increased risk for aneuploidies (Trisomy 21, 18) and cardiac defects.
-
Maternal Serum Analytes
- ↓ PAPP-A (Pregnancy-Associated Plasma Protein-A): Low levels are a consistent marker for Trisomy 21 & 18.
- ↑ free β-hCG (human Chorionic Gonadotropin): Significantly elevated in Trisomy 21; decreased in Trisomy 18.
⭐ The combination of NT, PAPP-A, and β-hCG achieves a detection rate of approximately 85% for Down syndrome.
Interpreting Results - Trisomy Telltales
- Combined First Trimester Screening (CFTS): Integrates Nuchal Translucency (NT) ultrasound with maternal serum markers (PAPP-A, free β-hCG) to calculate an adjusted aneuploidy risk.
| Aneuploidy | Nuchal Translucency (NT) | PAPP-A | Free β-hCG |
|---|---|---|---|
| Trisomy 21 (Down) | ↑ | ↓ | ↑↑ |
| Trisomy 18 (Edwards) | ↑ | ↓↓ | ↓↓ |
| Trisomy 13 (Patau) | ↑ | ↓↓ | ↓↓ |
- 📌 Mnemonic: For T21, remember HI-CG & HI-NT (hCG and NT are HIgh). For T18/13, all markers are profoundly Low.
⭐ Isolated low PAPP-A in the first trimester is a significant marker for adverse pregnancy outcomes like pre-eclampsia, fetal growth restriction, and stillbirth, even with a normal fetal karyotype.
Positive Screen Path - What Now?
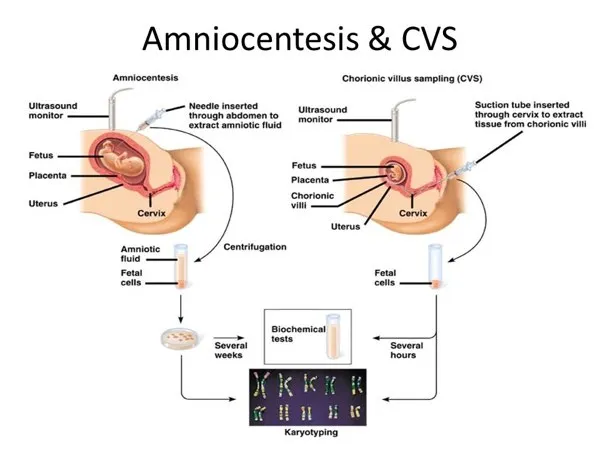
A positive screen requires patient counseling on risks and options. The choice is between proceeding directly to invasive diagnostic testing or opting for non-invasive cell-free fetal DNA (cffDNA) screening first, which has higher sensitivity and specificity.
⭐ Definitive diagnosis requires fetal genetic material. Screening tests only assess risk; they are not diagnostic. Both CVS and amniocentesis carry a small risk of miscarriage.
High‑Yield Points - ⚡ Biggest Takeaways
- First-trimester screening assesses risk for aneuploidies, mainly Trisomies 21, 18, and 13.
- It combines maternal serum analytes (free β-hCG, PAPP-A) with an ultrasound for nuchal translucency (NT).
- Performed between 11 and 14 weeks gestation.
- Trisomy 21 findings: ↑ NT, ↑ free β-hCG, and ↓ PAPP-A.
- Trisomy 18/13 findings: ↑ NT with ↓ free β-hCG and ↓ PAPP-A.
- This is a screening test, not diagnostic; abnormal results require confirmatory testing (CVS or amniocentesis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

