Alcohol Use - The Teratogen Tipple
- A leading preventable cause of birth defects and intellectual disability. No amount of alcohol is safe during pregnancy.
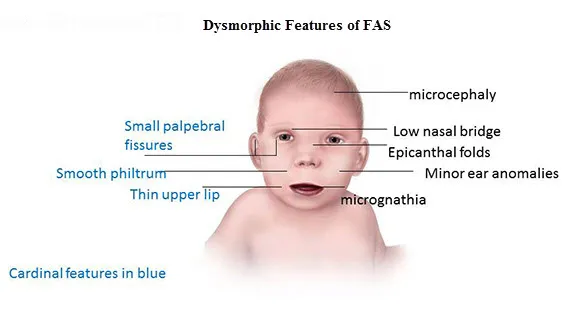
- Fetal Alcohol Syndrome (FAS) triad:
- Facial anomalies: Smooth philtrum, thin vermilion border, small palpebral fissures.
- Growth restriction: Pre- and/or postnatal (≤10th percentile).
- CNS abnormalities: Microcephaly, functional deficits (e.g., ADHD).
⭐ Alcohol is most teratogenic in the first trimester; it induces widespread apoptosis and failed neural crest cell migration.
Tobacco & Nicotine - Up in Smoke
- Pathophysiology: Nicotine (vasoconstrictor) & Carbon Monoxide (↓ $O_2$ delivery) → uteroplacental insufficiency & fetal hypoxia.
- Fetal Risks:
- Symmetrical fetal growth restriction (FGR) / low birth weight (LBW).
- ↑ risk of preterm labor, placental abruption, spontaneous abortion.
- Postnatal: ↑ risk of Sudden Infant Death Syndrome (SIDS), asthma, colic.
- Management: Cessation counseling is first-line. Nicotine replacement therapy (NRT) is a second-line option.
⭐ Exam Favorite: Tobacco is the leading preventable cause of Fetal Growth Restriction (FGR).
Opioids - Narcotic Neonates
- Maternal Management: Opioid use disorder (OUD) managed with methadone or buprenorphine. Avoids withdrawal cycles harmful to the fetus.
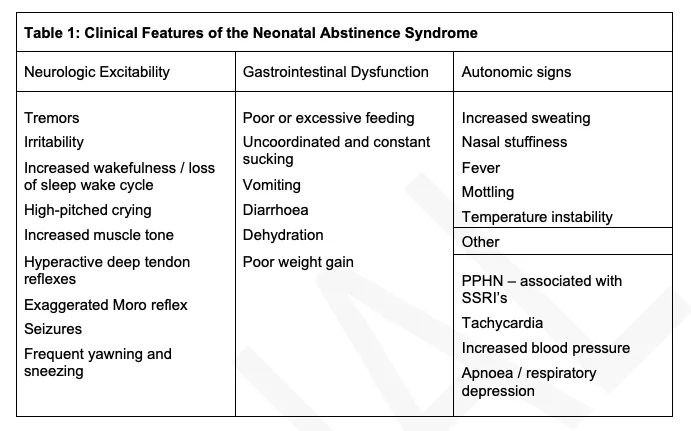
- Neonatal Abstinence Syndrome (NAS): Onset typically 24-72 hours post-birth.
- CNS: Irritability, high-pitched cry, tremors, seizures.
- GI: Poor feeding, vomiting, diarrhea.
- Autonomic: Sweating, fever, tachypnea.
- Management:
- Finnegan scoring to assess severity.
- Supportive: Swaddling, low stimulation, caloric support.
- Pharmacologic: Morphine is first-line.
⭐ High-Yield Fact: Buprenorphine is associated with a shorter duration of treatment and hospital stay for the neonate compared to methadone.
Cocaine & Stimulants - Vasoconstriction Vexation
- Mechanism: Intense sympathomimetic action → potent vasoconstriction → ↓ uteroplacental blood flow & placental ischemia.
- Maternal Risks: Placental abruption, hypertensive crisis, preterm labor, uterine tachysystole, myocardial infarction.
- Fetal & Neonatal Risks: Asymmetric IUGR, low birth weight, neurobehavioral deficits (irritability, hypertonia).
- ⚠️ Management: Avoid β-blockers (e.g., labetalol) due to risk of unopposed α-stimulation. Prefer benzodiazepines for seizures/agitation & hydralazine for hypertension.
⭐ Cocaine is a primary cause of painful third-trimester bleeding from placental abruption.
Screening & Management - Universal Precautions
- Universal Screening: Screen ALL pregnant patients for substance use at the first prenatal visit.
- Use validated questionnaires (e.g., 4P's, NIDA Quick Screen).
- Urine Drug Screen (UDS):
- Not routine; perform based on risk factors identified during screening.
- Requires informed consent; be aware of state-specific reporting laws.
- Management:
- A non-judgmental, supportive approach is crucial.
- Coordinate with a multidisciplinary team (social work, addiction specialists).
⭐ Universal screening is vital as many women with substance use disorder do not fit typical stereotypes.

High-Yield Points - ⚡ Biggest Takeaways
- Alcohol is the leading preventable cause of intellectual disability; look for classic FAS facies (smooth philtrum, thin upper lip).
- Cocaine use is strongly linked to placental abruption and fetal hypoxia due to potent vasoconstriction.
- Opioids (e.g., heroin) classically cause Neonatal Abstinence Syndrome (NAS); manage maternal use with methadone or buprenorphine.
- Tobacco is the most common cause of intrauterine growth restriction (IUGR) and low birth weight.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

