Pathophysiology - Sugar & The Bump
- Maternal hyperglycemia freely crosses the placenta; maternal insulin does not.
- Fetal pancreas responds with islet cell hyperplasia → fetal hyperinsulinemia.
- Insulin acts as a primary growth hormone → macrosomia (birth weight > 4.0-4.5 kg), organomegaly, and polycythemia.
- High insulin antagonizes cortisol, inhibiting surfactant production → neonatal respiratory distress syndrome (RDS).
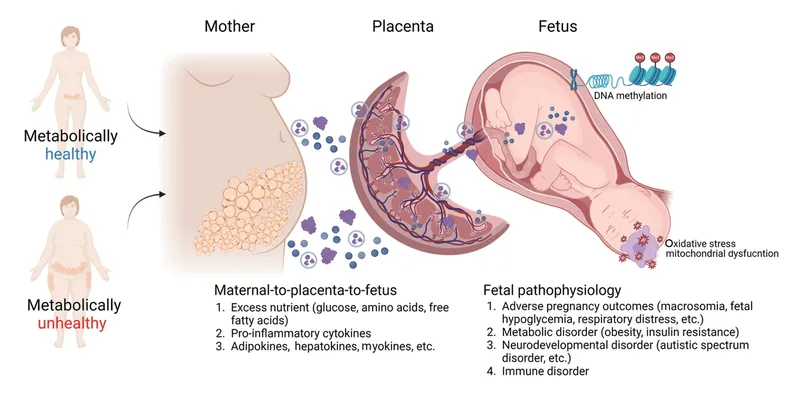
⭐ Fetal hyperinsulinemia is the main driver of macrosomia and can cause profound, persistent neonatal hypoglycemia after birth when the maternal glucose supply is suddenly cut.
Maternal & Fetal Risks - Double Jeopardy Diabetes
-
Maternal Risks:
- Diabetic Ketoacidosis (DKA), often at lower glucose levels (>200 mg/dL).
- Hypertensive Disorders: Chronic hypertension and a 2-4x ↑ risk of preeclampsia.
- Progression of End-Organ Damage: Worsening of proliferative retinopathy and nephropathy.
- Infections: Higher rates of UTIs, chorioamnionitis, and postpartum endometritis.
- Polyhydramnios.
- ↑ Cesarean delivery rates due to macrosomia.
-
Fetal & Neonatal Risks:
- Congenital Anomalies (1st trimester hyperglycemia):
- Most common: Cardiovascular (VSD, TGA).
- Most specific: CNS defects like neural tube defects and caudal regression syndrome.
- Macrosomia (>4.5 kg): Leads to shoulder dystocia, birth trauma (e.g., brachial plexus injury).
- IUGR: Paradoxically can occur with severe, long-standing diabetes with underlying vasculopathy.
- Neonatal Metabolic Issues:
- Hypoglycemia (from fetal hyperinsulinemia).
- Hypocalcemia, polycythemia, hyperbilirubinemia.
- Respiratory Distress Syndrome (RDS): Fetal hyperinsulinism antagonizes cortisol, delaying surfactant production.
- Congenital Anomalies (1st trimester hyperglycemia):
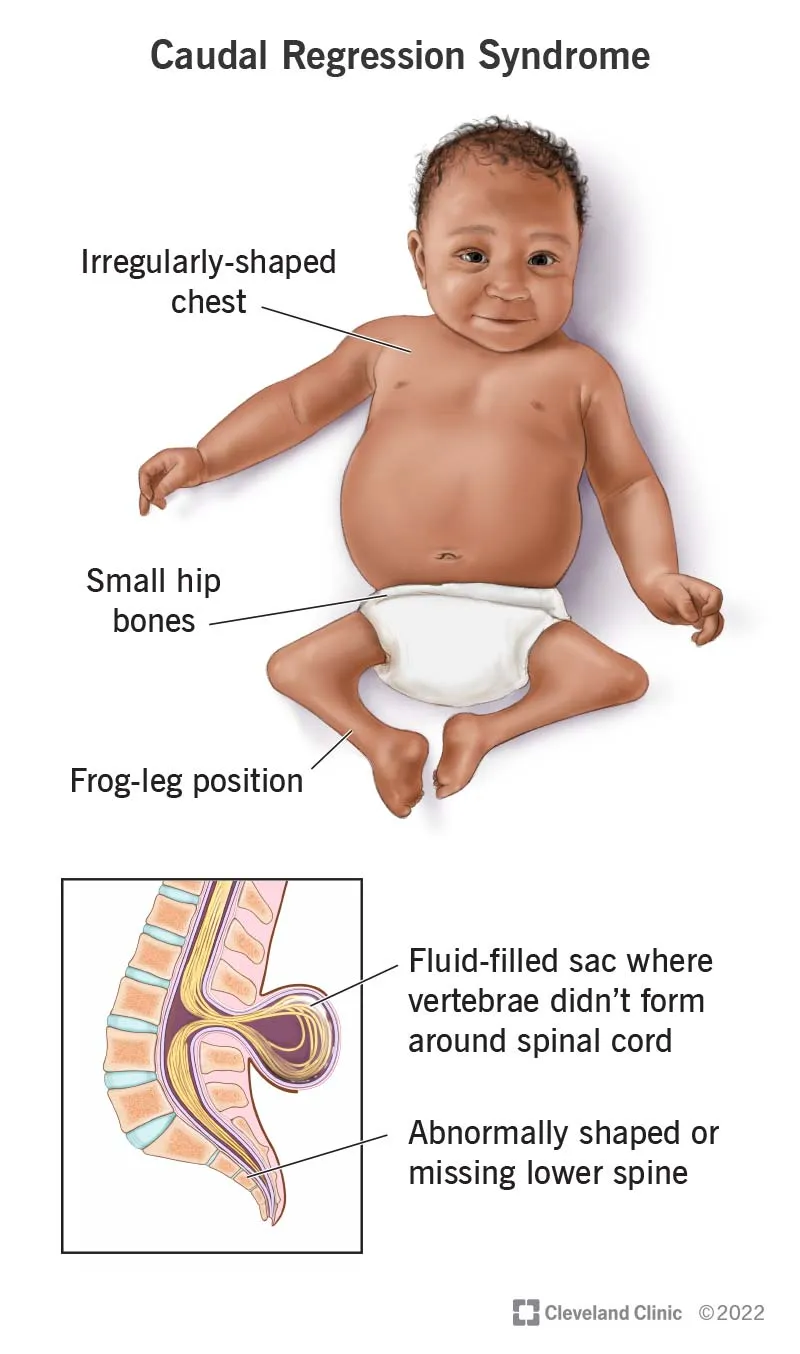
⭐ Caudal regression syndrome, although rare, is a highly specific congenital anomaly associated with pregestational diabetes. An elevated first-trimester HbA1c (>8.5%) is a major predictor.
Management - The Glycemic Gauntlet
- Preconception: Crucial for preventing congenital anomalies.
- Aim for HbA1c < 6.5%.
- High-dose folic acid (4 mg/day) to ↓ neural tube defect risk.
- Antepartum:
- Insulin is the mainstay therapy (doesn't cross placenta). Metformin/glyburide are second-line.
- Target glucose: Fasting <95, 1-hr postprandial <140, 2-hr postprandial <120 mg/dL.
- Fetal surveillance (NST, BPP) initiated at 32-34 weeks.
- Intrapartum:
- IV dextrose and insulin infusion to maintain euglycemia (target 80-110 mg/dL).
⭐ High-Yield: Postpartum insulin requirements plummet dramatically following delivery of the placenta, the primary source of insulin-antagonistic hormones (e.g., hPL). Failure to reduce insulin dosage can lead to severe maternal hypoglycemia.
Intra & Postpartum - The Final Countdown
- Intrapartum Goal: Maintain tight euglycemia (glucose 80-110 mg/dL).
- Requires IV regular insulin drip & dextrose infusion.
- Monitor glucose hourly.
- Postpartum Management: Insulin needs ↓ dramatically immediately after delivery.
- ⚠️ High risk for maternal hypoglycemia.
- Encourage breastfeeding; it improves glycemic control.
- Neonate Care: Monitor for hypoglycemia, hypocalcemia, polycythemia, and hyperbilirubinemia.
⭐ Postpartum, women often require only 50-60% of their pre-pregnancy insulin dose, especially if breastfeeding.
High‑Yield Points - ⚡ Biggest Takeaways
- Poor 1st-trimester glycemic control is the primary driver of congenital anomalies, especially cardiac and neural tube defects.
- Macrosomia (>4 kg) is a classic fetal complication, significantly increasing the risk of shoulder dystocia.
- Maternal risks include preeclampsia, polyhydramnios, and progression of pre-existing nephropathy or retinopathy.
- Management requires tight glucose control; insulin is the preferred agent.
- Begin fetal surveillance (NST, BPP) at 32-34 weeks.
- Neonates are at high risk for hypoglycemia, hypocalcemia, and hyperbilirubinemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

