Initial Assessment - Gauging the Gut Punch
-
Immediate Triage: First, assess for Systemic Inflammatory Response Syndrome (SIRS) and organ failure (e.g., shock, respiratory distress). Their presence mandates ICU-level care.
-
Bedside Scoring - BISAP: Quick and reliable for early risk stratification. 📌 B-I-S-A-P
- BUN >25 mg/dL
- Impaired mental status (GCS <15)
- SIRS criteria met
- Age >60 years
- Pleural effusion on imaging
⭐ A BUN >25 mg/dL is a key BISAP component and a strong independent predictor of mortality.
Prognostic Scores - Rating the Rampage
-
SIRS Criteria (Systemic Inflammatory Response Syndrome): Presence of ≥2 criteria suggests severe disease course. Used in multiple scores.
- Temp <36°C or >38°C
- HR >90
- RR >20 or PaCO₂ <32
- WBC <4k or >12k
-
BISAP Score: Quick assessment at bedside within 24h. Score ≥3 indicates high risk.
- BUN >25 mg/dL
- Impaired mental status
- SIRS present
- Age >60
- Pleural effusion
-
Other Scores:
- Ranson's Criteria: Classic but cumbersome (requires 48h).
- APACHE II: Gold standard in ICU; too complex for initial assessment.
⭐ A BUN level >20-25 mg/dL on admission is one of the strongest independent predictors of mortality in acute pancreatitis.
Imaging & Biomarkers - Scans and Signals
-
Imaging Modalities:
- Abdominal Ultrasound: Best initial test to detect gallstones or biliary duct dilation.
- Contrast-Enhanced CT (CECT):
- Timing: Optimal after 48-72 hours for assessing complications, not for initial diagnosis.
- Role: Identifies pancreatic necrosis (lack of enhancement), fluid collections, and is used for the Balthazar score.
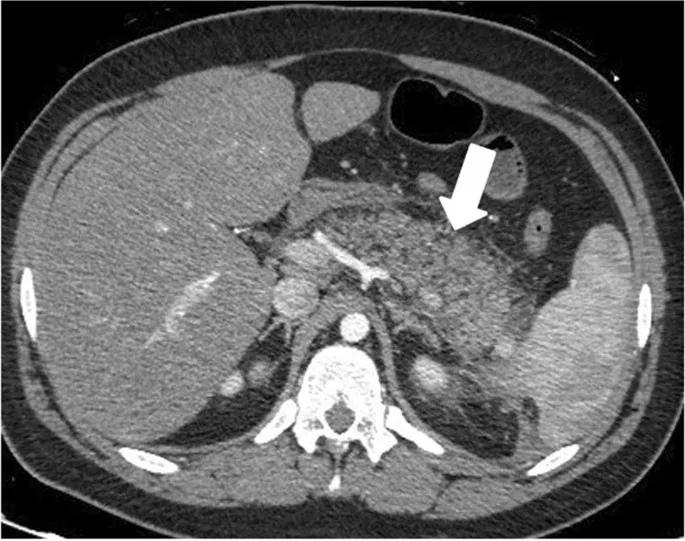
- MRCP: Excellent non-invasive tool for visualizing the biliary and pancreatic ducts if a stone is suspected.
-
Key Lab Markers:
- C-Reactive Protein (CRP): A level >150 mg/L at 48 hours is a marker for severe pancreatitis.
- Blood Urea Nitrogen (BUN): An increase in the first 24 hours signifies significant fluid sequestration.
- Procalcitonin: Elevated levels strongly suggest infected necrosis.
⭐ A rising BUN is one of the most important single predictors of mortality in acute pancreatitis.
- Ranson criteria are assessed at admission and again at 48 hours; a score ≥3 suggests severe pancreatitis.
- The APACHE II score is complex but can be used anytime to assess severity.
- Persistent SIRS (≥2 criteria) for >48 hours is a strong predictor of mortality.
- A rising BUN (e.g., >20-25 mg/dL) is a key single-marker predictor of severe disease.
- Hemoconcentration (Hct >44%) indicates significant fluid sequestration and risk of necrosis.
- CRP >150 mg/L at 48 hours correlates with pancreatic necrosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

